|
Part 1: Parties to the Contract:
|
|
|
This Contract Amendment (the “Amendment”) is between the Texas Health and Human Services Commission (HHSC), an administrative agency within the executive department of the State of Texas, having its principal office at 4900 North Lamar Boulevard, Austin, Texas 78751, and Superior HealthPlan, Inc. (HMO) a corporation organized under the laws of the State of Texas, having its principal place of business at: 2100 South IH-35, Suite 202, Austin, Texas 78704. HHSC and HMO may be referred to in this Amendment individually as a “Party” and collectively as the “Parties.”
The Parties hereby agree to amend their original contract, HHSC contract number 529-06-0280-00014 (the “Contract”) as set forth herein. The Parties agree that the terms of the Contract will remain in effect and continue to govern except to the extent modified in this Amendment.
This Amendment is executed by the Parties in accordance with the authority granted in Attachment A to the HHSC Managed Care Contract document, “HHSC Uniform Managed Care Contract Terms & Conditions,” Article 8, “Amendments and Modifications.”
|
||
|
Part 2: Effective Date of Amendment:
|
Part 3: Contract Expiration Date
|
Part 4: Operational Start Date:
|
|
March 1, 2011
|
August 31, 2013
|
STAR and CHIP HMOs: September 1, 2006
STAR+PLUS HMOs: February 1, 2007
CHIP Perinatal HMOs: January 1, 2007
|
|
Part 5: Project Managers:
|
||
|
HHSC:
Scott Schalchlin
Director, Health Plan Operations
11209 Metric Boulevard, Building H
Austin, Texas 78758
Phone: 512-491-1866
Fax: 512-491-1969
HMO:
Susan Erickson
Director of Contract Management
2100 South IH-35, Suite 202
Austin, Texas 78704
Phone: 512-692-1465
Fax: 512-692-1474
E-mail: serickson@centene.com
|
||
|
Part 6: Deliver Legal Notices to:
|
||
|
HHSC:
General Counsel
4900 North Lamar Boulevard, 4th Floor
Austin, Texas 78751
Fax: 512-424-6586
HMO:
Superior HealthPlan
2100 South IH-35, Suite 202
Austin, Texas 78704
Fax: 512-692-1435
|
||
|
Part 7: HMO Programs and Service Areas:
|
|
This Contract applies to the following HHSC HMO Programs and Service Areas (check all that apply). All references in the Contract Attachments to HMO Programs or Service Areas that are not checked are superfluous and do not apply to the HMO.
x Medicaid STAR HMO Program
Service Areas:
x Bexar x Lubbock
o Dallas x Nueces
x El Paso o Tarrant
o Harris x Travis
See Attachment B-6, “Map of Counties with HMO Program Service Areas,” for listing of counties included within the STAR Service Areas.
|
|
x Medicaid STAR+PLUS HMO Program
Service Areas:
xBexar x Nueces
oHarris oTravis
See Attachment B-6.1, “Map of Counties with STAR+PLUS HMO Program Service Areas,” for listing of counties included within the STAR+PLUS Service Areas.
|
|
xCHIP HMO Program
Core Service Areas:
x Bexar x Nueces
o Dallas oTarrant
x El Paso x Travis
o Harris o Webb
x Lubbock
Optional Service Areas:
x Bexar x Lubbock
x El Paso xNueces
o Harris xTravis
See Attachment B-6, “Map of Counties with HMO Program Service Areas,” for listing of counties included within the CHIP Core Service Areas and CHIP Optional Service Areas.
|
|
xCHIP Perinatal Program
Core Service Areas:
xBexar x Nueces
o Dallas oTarrant
xEl Paso x Travis
oHarris oWebb
xLubbock
Optional Service Areas:
xBexar x Lubbock
xEl Paso xNueces
oHarris xTravis
See Attachment B-6.2, “Map of Counties with CHIP Perinatal HMO Program Service Areas,” for a list of counties included within the CHIP Perinatal Service Areas.
|
|
Part 8: Payment
|
|
Part 8 of the HHSC Managed Care Contract document, “Payment,” is modified to add the capitation rates for Rate Period 5.
|
|
Part 9: Contract Attachments:
|
|
Part 10: Special Provision for Nueces Service Area
|
|
Part 11: Signatures:
|
|
The Parties have executed this Contract Amendment in their capacities as stated below with authority to bind their organizations on the dates set forth by their signatures. By signing this Amendment, the Parties expressly understand and agree that this Amendment is hereby made part of the Contract as though it were set out word for word in the Contract.
Texas Health and Human Services Commission
/s/ Charles E. Bell, M.D.
Charles E. Bell, M.D.
Deputy Executive Commissioner for Health Services
Date: 2/9/11
Superior HealthPlan, Inc.
/s/ Thomas Wise
By: Thomas Wise
Title: President and CEO
Date: 1/26/11
|
|
STATUS1
|
DOCUMENT REVISION2
|
EFFECTIVE DATE
|
DESCRIPTION3
|
|
Baseline
|
n/a
|
Initial version of the Uniform Managed Care Contract Terms & Conditions
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Revised version of the Uniform Managed Care Contract Terms & Conditions that includes provisions applicable to MCOs participating in the STAR+PLUS Program.
Article 2, “Definitions,” is amended to add or modify the following definitions: 1915(c) Nursing Facility Waiver; Community-based Long Term Care Services; Court-ordered Commitment; Default Enrollment; Dual Eligibles; Eligibles; Functionally Necessary Covered Services; HHSC Administrative Services Contractor; HHSC HMO Programs or HMO Programs; Medicaid HMOs; Medical Assistance Only; Member; Minimum Data Set For Home Care (MSD-HC); Nursing Facility Cost Ceiling; Nursing Facility Level of Care; Outpatient Hospital Service; Qualified and Disabled Working Individual (QDWI); Qualified Medicare Beneficiary; Service Coordination; Service Coordinator; Specified Low-income Medicare Beneficiary (SMBL); STAR+PLUS or STAR+PLUS Program; STAR+PLUS HMO; Supplemental Security Income (SSI).
Article 4, “Contract Administration and Management,” is amended to add Sections 4.02(a)(12) and 4.04.1, relating to the STAR+PLUS Service Coordinator.
Article 8, “Amendments and Modifications,” Section 8.06 is amended to clarify that CMS must approve all amendments to STAR and STAR+PLUS HMO contracts.
Article 10, “Terms and Conditions of Payment,” Section 10.05.1 is added to include the Capitation Rate structure provisions relating to STAR+PLUS. Section 10.11 is modified to apply only to STAR and CHIP. Section 10.11.1 is added to include the Experience Rebate provisions relating to STAR+PLUS.
|
|
Revision
|
1.2
|
September 1, 2006
|
Revised version of the Uniform Managed Care Contract Terms & Conditions that includes provisions applicable to MCOs participating in the STAR and CHIP Programs.
Section 4.04(a) is amended to change the reference from “Texas Board of Medical Examiners” to “Texas Medical Board”.
Article 5 is amended to clarify the following sections: 5.02(e)(5), regarding disenrollment of Members; 5.02(i), regarding disenrollment of foster care children; and 5.04(b), regarding CHIP eligibility and enrollment for babies of CHIP Members
|
|
STATUS1
|
DOCUMENT REVISION2
|
EFFECTIVE DATE
|
DESCRIPTION3
|
|
Article 10 is amended to clarify the following sections: 10.01(d), regarding the fixed monthly Capitation Rate components; 10.10(c), regarding updating the state system for Members who become eligible for SSI. Section 10.17 is added regarding recoupment for federal disallowance.
Article 17 is amended to clarify the following section: 17.01, naming HHSC as an additional insured.
|
|||
|
Revision
|
1.3
|
September 1, 2006
|
Article 2 is amended to modify and add the following definitions to include the CHIP Perinatal Program- Appeal, CHIP Perinatal Program, CHIP Perinatal HMO, CHIP Perinate, CHIP Perinate Newborn, Covered Services, Complaint, Delivery Supplemental Payment, Eligibles, Experience Rebate, HHSC Administrative Services Contractor, Major Population Group, Member, Optional Service Area, and Service Management.
Article 5 is amended to add the following sections: 5.04.1 CHIP Perinatal eligibility and enrollment; 5.05(c) CHIP Perinatal HMOs.
Article 10 is amended to apply to the CHIP Perinatal Program. Section 10.06(a) is amended to add the Capitation Rates Structure for CHIP Perinates and CHIP Perinate Newborns. Section 10.06(e) is added to include a description of the rate-setting methodology for the CHIP Perinatal Program. 10.09(b) is modified to include CHIP Perinatal Program; Section 10.11 is amended to add the CHIP Perinatal Program to the STAR and CHIP Experience Rebate. Section 10.12(c) amended to clarify cost sharing for the CHIP Perinatal Program.
|
|
Revision
|
1.4
|
September, 1 2006
|
Contract amendment did not revise Attachment A HHSC Uniform Managed Care Terms and Conditions
|
|
Revision
|
1.5
|
January 1, 2007
|
Revised version of the Uniform Managed Care Contract Terms & Conditions that includes provisions applicable to MCOs participating in the STAR, STAR+PLUS, CHIP, and CHIP Perinatal Programs.
Section 5.04(a) is amended to clarify the period of CHIP continuous coverage.
Section 5.04.1 is amended to clarify the process for a CHIP Perinatal Newborn to move into CHIP at the end of the 12month CHIP Perinatal Program eligibility.
Section 5.08 is added to include STAR+PLUS special default language.
Section 10.06.1 is amended to correct the FPL percentages for CHIP Perinates and CHIP Perinate Newborns.
Section 17.01 is amended to clarify the insurance requirements for the HMOs and Network Providers and to remove the insurance requirements for Subcontractors.
|
|
STATUS1
|
DOCUMENT REVISION2
|
EFFECTIVE DATE
|
DESCRIPTION3
|
|
Section 17.02(b) is added to clarify that a separate Performance Bond is not needed for the CHIP Perinatal Program.
|
|||
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment A HHSC Uniform Managed Care Terms and Conditions
|
|
Revision
|
1.7
|
July 1, 2007
|
Article 2 is modified to correct and align definition for “Clean Claim” with the UMCM.
Section 4.08(c) is modified to add a cross-reference to new Attachment B-1, Section 8.1.1.2.
Section 5.05(a), Medicaid HMOs, is amended to clarify provisions regarding enrollment into Medicaid Managed Care from Medicaid Fee-for-Service while in the hospital, changing HMOs while in the hospital, and addressing which HMO is responsible for professional and hospital charges during the hospital stay.
New Section 10.05.1 (c) is added to clarify capitation payments (delays in payment and levels of capitation) for Members certified to receive STAR+PLUS Waiver Services.
Section 10.06.1 is modified to include the CHIP Perinatal pass through for delivery physician services for women under 185% FPL.
Section 10.11 is modified to include treatment of the new Incentives and Disincentives (within the Experience Rebate determination); additionally, several clarifications are added with respect to the continuing accrual of any unpaid interest, etc.
Section 10.11.1 is modified to include treatment of the new Incentives and Disincentives (within the Experience Rebate determination); additionally, several clarifications are added with respect to the continuing accrual of any unpaid interest, etc.
|
|
Revision
|
1.8
|
September 1, 2007
|
Article 2 is modified to add definitions for Migrant Farmworker and FWC as a result of the Frew litigation corrective action plans.
Article 2 is modified to reflect legislative changes required by SB 10 to the definition for Value-added Services.
New Section 5.03.1 is added to clarify the enrollment process for infants born to pregnant women in STAR+PLUS.
Section 5.04 is modified to reflect legislative changes required by HB 109.
Section 10.18 is added to clarify the required pass through of physician rate increases for all programs to comply with HHSC directives.
|
|
STATUS1
|
DOCUMENT REVISION2
|
EFFECTIVE DATE
|
DESCRIPTION3
|
|
Revision
|
1.9
|
December 1, 2007
|
Section 10.11(d) is modified to increase the Experience rebate loss carry forward from 1 year to 2 years.
Section 10.11(e) is modified to eliminate the plan's responsibility to submit the actuarial certification on the 90 day FSR.
Section 10.11.1 (d) is modified to increase the Experience rebate loss carry forward from 1 year to 2 years.
Section 10.11.1 (e) is modified to eliminate the plan's responsibility to submit the actuarial certification on the 90 day FSR.
|
| Revision | 1.10 | March 1, 2008 |
Article 2 is modified to remove the word “administrative” from the definition for Allowable Expenses”.
Article 2 is modified to update the definition for Affiliate.
Section 4.08 is modified to provide consistency of language in sections 4.08(b)(3), and to obligate the HMOs to provide HHSC with copies of amended Subcontracts.
Section 7.05 is modified to update the requirements regarding with state and federal anti-discrimination laws.
Section 10.06.1 is modified to clarify the CHIP Perinatal pass through for delivery physician services for women under 185% FPL.
Section 10.11 (b) is modified to change the heading in the table from Experience Rebate as a % of Revenues to Pre-tax Income as a % of Revenues
Section 10.11 (c) (1) is modified to remove the word “administrative” from the title of UMCM chapter reference.
Section 10.11 (e) (4) is modified to remove the word “administrative” from the title of UMCM chapter reference.
Section 10.11.1 (b) is modified to establish new STAR+PLUS rebate brackets for Rate Period 2 and after.
Section 10.11.1 (c) (1) is modified to remove the word “administrative” from the title of UMCM chapter reference.
|
| Revision | 1.11 | September 1, 2008 |
Article 2 is modified to add definitions for Discharge and Transfer.
Article 2 is modified to remove the “Pediatric and Family” qualifier from Advanced Practice Nurses in the definition for PCP.
Section 5.02 is modified to clarify that only Medicaid HMOs have a limited right to request that a Member be disenrolled.
Section 5.03 is modified to clarify that newborns must remain in their mother’s Medicaid HMO for at least 90 days following the date of birth, unless the mother request s a plan change.
Section 5.05(a), is modified to clarify provisions regarding enrollment into Medicaid Managed Care from Medicaid Fee-for-Service while in the hospital and changing HMOs while in the hospital.
Section 5.05(c) is modified to clarify the span of coverage for CHIP Perinate Newborns who are in the hospital on the effective date of disenrollment.
Section 05.07.1 is added to establish a special temporary STAR default process for service areas with HMOs that did not contract with HHSC prior to September 1, 2006.
Section 05.08.1 is added to establish a special temporary STAR+PLUS default process for service areas with HMOs that did not contract with HHSC prior to September 1, 2006.
Section 09.06 is added to require the HMOs to notify HHSC of legal and other proceedings, and related events.
Section 10.11 (e) is modified to clarify the settlement process.
Section 10.11 (f) is modified to require the payment of interest on any Experience Rebate unpaid 35 days after the due date for the 90-day FSR Report.
Section 10.11.1 (e) is modified to reference the process defined in Sections 10.11 (e) and (f).
Section 10.11.1 (f) is deleted as part of the Section 10.11.1 (e) alignment with the process defined in Sections 10.11 (e) and (f).
Section 10.11.2 is added to institute the STAR, CHIP, CHIP Perinatal, and STAR+PLUS Administrative Expense Cap.
Section 10.12 (b) is modified to address federal CHIP regulations.
Section 11.07 is modified to remove extraneous word.
|
| Revision | 1.12 | March 1, 2009 |
Article 2 is modified to add the definitions for Bariatric Supplemental Payment and TP 13; and to clarify the definitions for Migrant Farmworker, TP 40, and TP 45.
Section 5.05 is modified to add item (a)(6) to clarify movement from STAR+PLUS to STAR Health; add item (a)(7) regarding movement from STAR, STAR+PLUS, or FFS due to SSI status; clarify item (c); and add item (d) regarding effective date of SSI status. These ratifications of existing policies and processes are effective 9/1/08. Any future change to such policies or processes will require adjustments to the capitation payments.
Section 5.07.1 is modified to include the Harris Expansion Service Area.
Section 10.06.1(a) is modified to accurately reflect the percentage breakdown.
Section 10.09(b) is modified to accurately reflect the percentage breakdown.
Section 10.10(c) is modified to conform to clarifications in Section 5.05(d).
Section 10.11.2 is modified to add Bariatric Supplemental Payments.
Section 10.11.2(d) is modified to correct a contract reference.
Section 10.19, Bariatric Supplemental Payment for STAR and STAR+PLUS HMOs is added.
|
| Revision | 1.13 | September 1, 2009 |
All references to “THSteps” are changed to “Texas Health Steps”
Article 2 is amended to add the definitions for Rate Period 3, and Rate Period 4.
Section 5.05 is amended to clarify that Hospital facility charges for inpatient mental health Covered Services will be paid by the STAR+PLUS HMO.
Section 5.09 Default Methodology for Frew Incentives and Disincentives is added.
Section 7.02 is modified to add references to 1 T.A.C. Part 15, Chapter 371 and the Frew Consent Decree and Alberto N. Partial Settlement Agreements
Section 10.11(a) is amended to change “Rate Year” to “Rate Period”
Section 10.11(b) is amended to reflect the change in the SFY 2010 sharing tier structure for the Experience Rebate.
Section 10.11(d) is amended to clarify the two year loss carry forward.
Section 10.11(e) is amended to clarify the required documentation for non-scheduled payments.
Section 10.11.1(a) is amended to change “Rate Year” to “Rate Period” and to clarify when the HMO must pay an Experience Rebate.
Section 10.11.1(b) is amended to reflect the change in the SFY 2010 sharing tier structure for the Experience Rebate.
Section 10.11.1(d) is amended to clarify the two year loss carry forward.
Section 10.12 is modified to include CHIP enrollees in prohibition against liability for payment (Balance Billing).
Section 12.15 is added to establish a pre-termination process.
Section 17.01(a) is modified to provide clarification of required insurance coverage, including deletion of Standard Worker’s
Section 17.01(b) is modified to correctly identify the type of professional liability coverage required.
Section 17.01(c)(4) is modified to require that HHSC is named as loss payee of insurance coverage.
Section 17.01(c)(5) is modified to require continuous coverage during Term of Contract.
Section 17.01(c)(6) is modified to require notification prior to reduction in coverage and to add provision to insurance policy
requiring 30-day notice prior to reduction in, cancellation, or non-renewal of, the policy.
Section 17.02(a) is modified to align the performance bond requirements with insurance practices by requiring one bond per MCO with a defined term and amount and to require annual renewal of the bond.
Section 17.02(c) is added to establish a process for release of previous performance bonds received by HHSC.
|
| Revision | 1.14 | December 1, 2009 | Section 17.02 (a) is modified to require the single bond per MCO with a defined term and amount beginning in SFY2010. |
| Revision | 1.15 | March 1, 2010 | Article 2 is amended to revise the definition for "Material Subcontractor or Major Subcontractor" |
| Revision | 1.16 | September 1, 2010 |
All references to “Frew vs. Hawkins” are changed to “Frew vs. Suehs”.
Definition of CHIP Perinate Newborn is modified.
Definition for Medicaid HMOs is modified to include the STAR Health Program.
Definition for Primary care Physician or Primary Care Provider (PCP) is modified to clarify that APNs and PAs must practice under the supervision of a PCP.
Definitions for Rate Periods 5 and 6 are added.
Section 4.02 is amended to clarify that STAR+PLUS HMOs must notify HHSC when the management/leadership for the STAR+PLUS Service Coordinators changes.
Section 4.08(b)(3) and (4) are modified to clarify the timeframes for notification.
Section 5.04.1 is modified to reflect changes to CHIP Perinatal Program eligibility, effective 9/1/10. The section is also modified to clarify that CHIP Perinatal members have 90 days to select an HMO if defaulted upon enrollment.
Section 5.05 is modified to reflect changes to CHIP Perinatal Program eligibility, effective 9/1/10, and to remove (d)(4) reference to ICM Program.
Section 7.07 is amended to add subsection (b).
Section 9.02(c) is modified to add “the Medicaid Fraud Control Unit of the Texas Attorney General's Office or its designee”.
Section 10.06.1 has been modified to clarify the CHIP Perinate Newborn 0% to 185% rate cell
|
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment A HHSC Uniform Managed Care Terms and Conditions |
| Revision | 1.18 | March 1, 2011 |
Definition of "Major Population Group" is modified
The definition of "Medically Necessary" is revised to address the review criteria applicable to children in Medicaid, consistent with 42 USC § 1396(r)(5) and Alberto N requirements. The HMOs are already contractually obligated to comply with these requirments, so the change is for clarification only.
Definition of "Outpatient Hospital Services" is modifed to remove language that is included in UMCM.
Definition of "Post-stabilization Care Services" is modified.
Definition of "Texas Health Network" is deleted.
Definition of "Uniform Managed Care Manual" is modified.
Section 4.08 is modified to prohibit Medicaid payments to entities located outside the U.S. in conformance with the Affordable Care Act.
Section 4.10 is modifed to prohibit medicaid payments to entities located outside the U.S. in conformance with the Affordable Care Act.
Section 5.04 is modified to clarify that infants born to CHIP members are not automatically enrolled in CHIP.
Section 5.05(a)(3) is modified to correct contract cross-reference.
Section 7.02(a) is modified to remove case identification information from the Frew and Alberto N items.
Section 8.06 is revised to apply generally to all HMO contracts.
Section 9.01 is revised to clarify the requirments for record retention in accordance with Federal requirments.
Section 10.11.1 is modified to let the HMOs consoldiate their DFW STAR+PLUS experience with their other STAR+PLUS products.
|
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
Responsibility for Inpatient Stay Services
|
||
|
Exception
|
Hospital Facility Charges
|
Professional Services Charges
|
|
Member Retroactively Enrolled in STAR per Section 5.03
|
STAR HMO
|
STAR HMO
|
|
Member ≤ 12 Months of Age Who Is Prospectively Enrolled in STAR
|
Medicaid FFS*
|
STAR HMO
|
|
Member ≤ 12 Months of Age Who Is Prospectively Enrolled in STAR+PLUS
|
STAR+PLUS HMO for Inpatient Mental Health Covered Services
Medicaid FFS for all Other Inpatient Facility Services*
|
STAR+PLUS HMO
|
|
Pre-Tax Income as a % of Revenues
|
HMO Share
|
HHSC Share
|
|
< 3%
|
100%
|
0%
|
|
> 3% and < 7%
|
75%
|
25%
|
|
> 7% and < 10%
|
50%
|
50%
|
|
> 10% and < 15%
|
25%
|
75%
|
|
> 15%
|
0%
|
100%
|
|
Pre-tax Income as a % of Revenues
|
HMO Share
|
HHSC Share
|
|
≤ 3%
|
100%
|
0%
|
|
> 3% and ≤ 5%
|
80%
|
20%
|
|
> 5% and ≤ 7%
|
60%
|
40%
|
|
> 7% and ≤ 9%
|
40%
|
60%
|
|
> 9% and ≤ 12%
|
20%
|
80%
|
|
> 12%
|
0%
|
100%
|
|
Pre-tax Income as a % of Revenues
|
HMO Share
|
HHSC Share
|
|
< 3%
|
50%
|
50%
|
|
> 3%
|
75%
|
25%
|
|
Pre-tax Income as a % of Revenues
|
HMO Share
|
HHSC Share
|
|
≤ 2%
|
100%
|
0%
|
|
> 2% and ≤ 6%
|
75%
|
25%
|
|
> 6% and ≤ 10%
|
50%
|
50%
|
|
> 10% and ≤ 15%
|
25%
|
75%
|
|
> 15%
|
0%
|
100%
|
|
Pre-tax Income as a % of Revenues
|
HMO Share
|
HHSC Share
|
|
≤ 3%
|
100%
|
0%
|
|
> 3% and ≤ 5%
|
80%
|
20%
|
|
> 5% and ≤ 7%
|
60%
|
40%
|
|
> 7% and ≤ 9%
|
40%
|
60%
|
|
> 9% and ≤ 12%
|
20%
|
80%
|
|
> 12%
|
0%
|
100%
|
|
|
(1) The total premiums paid by HHSC (earned by the HMO), and corresponding Member Months, will be taken from the relevant FSR (or audit report) for the Rate Period.
|
|
|
(2) There are two components of the administrative expense portion of the Capitation Rate structure: the percentage rate to apply against the total premiums paid (the “percentage of premium” within the administrative expenses), and, the dollar rate per Member Month (the “fixed amount” within the administrative expenses). These will be taken from the supporting details associated with the official notification of final Capitation Rates, as supplied by HHSC. This notification is sent to the HMOs during the annual rate setting process via email, labeled as “the final rate exhibits for your health plan.” The email has one or more spreadsheet files attached, which are particular to the given HMO. The spreadsheet(s) show the fixed amount and percentage of premium components for the administrative component of the Capitation Rate.
|
|
1. Multiply the predetermined administrative expense rate structure “fixed amount,” or dollar rate per Member Month (for example, $11.00), by the actual number of Member Months for the Program and Service Area during the Rate Period (for example, 70,000):
|
|
|
• $11.00 x 70,000 = $770,000.
|
|
2. Multiply the predetermined percent of premiums in the administrative expense rate structure (for example, 5.75%), by the actual aggregate premiums earned for the Program and Service Area during the Rate Period (for example, $6,000,000).
|
|
|
• 5.75% x $6,000,000 = $345,000.
|
|
3. For SFY 2009, add the totals of items 1-2 and multiply the sum by the adjustment factor of 1.05. To this product, add applicable premium taxes and maintenance taxes (for example, $112,000), to determine the Admin Cap for the Program and Service Area:
|
|
|
• 1.05($770,000 + $345,000) + $112,000 = $1,282,750.
|
|
In this example, $1,282,750 would be the Admin Cap for a single Program in a given Service Area for an HMO in a particular Rate Period.
|
|
|
• $770,000 + $345,000 + $112,000 = $1,227,000.
|
|
|
In this example, $1,227,000 would be the Admin Cap for a single Program in a given Service Area for an HMO in a particular Rate Period.
|
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
n/a
|
Initial version Attachment B-1, Section 6
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Revised version of the Attachment B-1, Section 6, that includes provisions applicable to MCOs participating in the STAR+PLUS Program.
Section 6.3.2.1, Experience Rebate Reward, is modified to delete references to the selected performance indicators and the Quality Challenge Pool.
Section 6.3.2.2, Performance-Based Capitation Rate, is modified to include STAR+PLUS and to add Additional STAR+PLUS Performance Indicators. Section 6.3.2.3, Quality Challenge Award, is modified to include STAR+PLUS. Section 6.3.2.5, STAR+PLUS Hospital Inpatient Performance Based Capitation Rate: Hospital Inpatient Stay Cost Incentives and Disincentives, is added.
Section 6.3.2.5.1, STAR+PLUS Hospital Inpatient Disincentive – Administrative Fee at Risk, is added.
Section 6.3.2.5.2, STAR+PLUS Hospital Inpatient Incentive – Shared Savings Award, is added.
|
|
Revision
|
1.2
|
September 1, 2006
|
Revised version of the Attachment B-1, Section 6, that includes provisions applicable to MCOs participating in the STAR and CHIP Programs.
Section 6.3.2.2, Performance-Based Capitation Rate, modifies the standard performance indicator for the Behavioral Health Hotline to change the maximum abandonment rate from 5% to 7% (except in the Dallas Core Service Area).
Section 6.3.2.3, Quality Challenge Award, is modified to reflect the new start date for the Quality Challenge Award, which will not be implemented until State Fiscal Year 2008.
|
|
Revision
|
1.3
|
September 1, 2006
|
Revised version of the Attachment B-1, Section 6, that includes provisions applicable to MCOs participating in the CHIP Perinatal Program.
Section 6.3.2.1 modified to clarify that the Experience Rebate Reward incentive may apply to the CHIP Perinatal Program at a later date.
Section 6.3.2.2 modified to clarify that the Performance-based Capitation Rate will not apply for the CHIP Perinatal Program in SFY 2007.
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment did not revise Attachment B-1 Section 6 – Premium Payment, Incentives, and Disincentives
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 6 – Premium Payment, Incentives, and Disincentives
|
|
Revision
|
1.6
|
February 1, 2007
|
Revised version of the Attachment B-1, Section 6, that includes provisions applicable to MCOs participating in the STAR+PLUS Program.
Section 6.3.2.5 is modified to clarify the months included in Rate Period 1.
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 6 – Premium Payment, Incentives, and Disincentives
|
|
Revision
|
1.8
|
September 1, 2007
|
Section 6.3 is modified as a result of SB 10 legislation and the Frew litigation to prohibit HMOs from passing down financial disincentives or sanctions to providers.
Section 6.3.1.1 is modified as a result of the Frew litigation to allow HHSC to post information regarding poor HMO performance on the HHSC website.
Section 6.3.2.2 is modified to clarify language regarding the Performance Indicator Dashboard and the reapportionment of points for the 1% at-risk premium.
Section 6.3.2.3 is modified as a result of the Frew litigation to clarify language.
New Section 6.3.2.6 is added as a result of the Frew litigation to clarify requirements for additional incentives and disincentives.
|
|
Revision
|
1.9
|
December 1, 2007
|
Section 6.3.2.3 is modified to outline the calculation methodology for STAR, STAR+PLUS, and CHIP.
|
| Revision | 1.10 | March 1, 2008 | Contract amendment did not revise Attachment B-1 Section 6 - Premium Payment, Incentives, and Disincentives. |
| Revision | 1.11 | September 1, 2008 | Contract amendment did not revise Attachment B-1 Section 6 - Premium Payment, Incentives, and Disincentives. |
| Revision | 1.12 | March 1, 2009 | Section 6.2.1 is modified to add Bariatric Supplemental Payments. |
| Revision | 1.13 | September 1, 2009 |
Section 6.3.2.2 is modified to remove the list of performance indicators.
Section 6.3.2.5.1 is amended to clarify the 22% reduction.
Section 6.3.2.7 Frew Incentives and Disincentives is added.
Section 6.3.2.8 Nursing Facility Utilization Disincentive – 1% At-Risk Performance Indicator is added
|
| Revision | 1.14 | December 1, 2009 | Contract amendment did not revise Attachment B-1 Section 6 - Premium Payment, Incentives, and Disincentives |
| Revision | 1.15 | March 1, 2010 | Contract amendment did not revise Attachment B-1 Section 6 - Premium Payment, Incentives, and Disincentives |
| Revision | 1.16 | September 1, 2010 | Section 6.3.2.7 reference to "Frew v. Hawkins" changed to "Frew v. Suehs". |
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment B-1 Section 6 - Premium Payment, Incentives, and Disincentives |
| Revision | 1.18 | March 1, 2011 | Section 6.3.2.8 is modified to remove "1% At-Risk Performance Indicator" from the section name, and to clarify that nursing facility utilization will be measured in the Performance Based Capitation Rate and the Quality Challenge Award. |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
6. Premium Payment, Incentives, and Disincentives
|
|
6.1 Capitation Rate Development
|
|
6.2 Financial Payment Structure and Provisions
|
|
6.2.1 Capitation Payments
|
|
6.3 Performance Incentives and Disincentives
|
|
6.3.1 Non-financial Incentives
|
|
6.3.1.1 Performance Profiling
|
|
6.3.1.2 Auto-assignment Methodology for Medicaid HMOs
|
|
6.3.2 Financial Incentives and Disincentives
|
|
6.3.2.1 Experience Rebate Reward
|
|
6.3.2.3 Quality Challenge Award
|
|
6.3.2.5 STAR+PLUS Hospital Inpatient Performance-Based Capitation Rate: Hospital Inpatient Stay Cost Incentives & Disincentives
|
|
6.3.2.5.2 STAR+PLUS Hospital Inpatient Incentive – Shared Savings Award
|
|
6.3.2.6 Additional Incentives and Disincentives
|
|
DOCUMENT HISTORY LOG
|
||||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
|
Baseline
|
n/a
|
Initial version Attachment B-1, Section 7
|
||
|
Revision
|
1.1
|
June 30, 2006
|
Revised version of the Attachment B-1, Section 7, that includes provisions applicable to MCOs participating in the STAR+PLUS Program.
Sections 7.1 to 7.3 modified to include STAR+PLUS.
|
|
|
Revision
|
1.2
|
September 1, 2006
|
Revised version of the Attachment B-1, Section 7, that includes provisions applicable to MCOs participating in the STAR and CHIP Programs.
Section 7.3.1.7, Operations Readiness, changes reference from “Operational Date” to “Effective Date.”
|
|
|
Revision
|
1.3
|
September 1, 2006
|
Revised version of the Attachment B-1, Section 7, that includes provisions applicable to MCOs participating in the CHIP Perinatal Program.
Sections 7.2, 7.3, and 7.3.1.2 through 7.3.1.7 modified to include the CHIP Perinatal Program.
|
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements
|
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements
|
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements
|
|
|
Revision
|
1.7
|
July 1, 2007
|
Section 7.3.1.9 is modified to add a cross-reference to Attachment B-1, Sections 8.1.1.2 and 8.1.18.
|
|
|
Revision
|
1.8
|
September 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements
|
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements
|
|
| Revision | 1.10 | March 1, 2008 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.11 | September 1, 2008 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.12 | March 1, 2009 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.13 | September 1, 2009 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.14 | December 1, 2009 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.15 | March 1, 2010 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.16 | September 1, 2010 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
| Revision | 1.18 | March 1, 2011 | Contract amendment did not revise Attachment B-1 Section 7 – Transition Phase Requirements | |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
||||
|
|
7. Transition Phase Requirements
|
|
|
7.1 Introduction
|
|
|
7.2 Transition Phase Scope for HMOs
|
|
|
7.3 Transition Phase Schedule and Tasks
|
|
|
7.3.1 Transition Phase Tasks
|
|
|
7.3.1.1 Contract Start-Up and Planning
|
|
|
• define project management and reporting standards;
|
|
|
• establish communication protocols between HHSC and the HMO;
|
|
|
• establish contacts with other HHSC contractors;
|
|
|
• establish a schedule for key activities and milestones; and
|
|
|
• clarify expectations for the content and format of Contract Deliverables.
|
|
|
7.3.1.2 Administration and Key HMO Personnel
|
|
|
7.3.1.3 Financial Readiness Review
|
|
|
1. The Contractor’s legal name, trade name, or any other name under which the Contractor does business, if any.
|
|
|
2. The address and telephone number of the Contractor’s headquarters office.
|
|
|
3. A copy of its current Texas Department of Insurance Certificate of Authority to provide HMO or ANHC services in the applicable Service Area(s). The Certificate of Authority must include all counties in the Service Area(s) for which the Contractor is proposing to serve HMO Members.
|
|
|
4. Indicate with a “Yes-HMO”, “Yes-ANHC” or “No” in the applicable cell(s) of the Column B of the following chart whether the Contractor is currently certified by TDI as an HMO or ANHC in all counties in each of the CSAs in which the Contractor proposes to participate in one or more of the HHSC HMO Programs. If the Contractor is not proposing to serve a CSA for a particular HMO Program, the Contractor should leave the applicable cells in the table empty.
|
|
Column A
|
Column B
|
Column C
|
|
Core Service Area (CSA)
|
TDI Certificate of Authority
|
Counties/Partial Counties without a TDI Certificate of Authority
|
|
Bexar
|
||
|
Dallas
|
||
|
El Paso
|
||
|
Harris
|
||
|
Lubbock
|
||
|
Nueces
|
||
|
Tarrant
|
||
|
Travis
|
||
|
Webb
|
|
|
5. For Contractors serving any CHIP and CHIP Perinatal OSAs, indicate with a “Yes-HMO”, “Yes-ANHC” or “No” in the applicable cell(s) of the Column C of the following chart whether the Contractor is currently certified by TDI as an HMO or ANHC in the entire county in the OSA. If the Contractor is not proposing to serve an OSA, the Contractor should leave the applicable cells in the table empty.
|
|
CHIP Program
|
|||
|
Column A
|
Column B
|
Column C
|
|
|
Core Service Area (CSA)
|
Affiliated CHIP OSA
|
TDI Certificate of Authority
|
|
|
Bexar
|
|||
|
El Paso
|
|||
|
Harris
|
|||
|
Lubbock
|
|||
|
Nueces
|
|||
|
Travis
|
|||
|
CHIP Perinatal Program
|
||
|
Column A
|
Column B
|
Column C
|
|
Core Service Area (CSA)
|
Affiliated CHIP OSA
|
TDI Certificate of Authority
|
|
Bexar
|
||
|
El Paso
|
||
|
Harris
|
||
|
Lubbock
|
||
|
Nueces
|
||
|
Travis
|
||
|
|
6. If the Contractor proposes to participate in STAR or STAR+PLUS and seeks to be considered as an organization meeting the requirements of Section §533.004(a) or (e) of the Texas Government Code, describe how the Contractor meets the requirements of §§533.004(a)(1), (a)(2), (a)(3), or (e) for each proposed Service Areas.
|
|
|
7. The type of ownership (proprietary, partnership, corporation).
|
|
|
8. The type of incorporation (for profit, not-for-profit, or non-profit) and whether the Contractor is publicly or privately owned.
|
|
|
9. If the Contractor is an Affiliate or Subsidiary, identify the parent organization.
|
|
|
10. If any change of ownership of the Contractor’s company is anticipated during the 12 months following the Proposal due date, the Contractor must describe the circumstances of such change and indicate when the change is likely to occur.
|
|
|
11. The name and address of any sponsoring corporation or others who provide financial support to the Contractor and type of support, e.g., guarantees, letters of credit, etc. Indicate if there are maximum limits of the additional financial support.
|
|
|
12. The name and address of any health professional that has at least a five percent financial interest in the Contractor and the type of financial interest.
|
|
|
13. The names of officers and directors.
|
|
|
14. The state in which the Contractor is incorporated and the state(s) in which the Contractor is licensed to do business as an HMO. The Contractor must also indicate the state where it is commercially domiciled, if applicable.
|
|
|
15. The Contractor’s federal taxpayer identification number.
|
|
|
16. The Contractor’s Texas Provider Identifier (TPI) number if the Contractor is Medicaid-enrolled in Texas.
|
|
|
17. Whether the Contractor had a contract terminated or not renewed for non-performance or poor performance within the past five years. In such instance, the Contractor must describe the issues and the parties involved, and provide the address and telephone number of the principal terminating party. The Contractor must also describe any corrective action taken to prevent any future occurrence of the problem leading to the termination.
|
|
|
18. A current Certificate of Good Standing issued by the Texas Comptroller of Public Accounts, or an explanation for why this form is not applicable to the Contractor.
|
|
|
19. Whether the Contractor has ever sought, or is currently seeking, National Committee for Quality Assurance (NCQA) or American Accreditation HealthCare Commission (URAC) accreditation status, and if it has or is, indicate:
|
|
|
• its current NCQA or URAC accreditation status;
|
|
|
• if NCQA or URAC accredited, its accreditation term effective dates; and
|
|
|
• if not accredited, a statement describing whether and when NCQA or URAC accreditation status was ever denied the Contractor.
|
|
|
1. A signed letter of commitment from each Material Subcontractor that states the Material Subcontractor’s willingness to enter into a Subcontractor agreement with the Contractor and a statement of work for activities to be subcontracted. Letters of Commitment must be provided on the Material Subcontractor’s official company letterhead and signed by an official with the authority to bind the company for the subcontracted work. The Letter of Commitment must state, if applicable, the company’s certified HUB status.
|
|
|
2. The Material Subcontractor’s legal name, trade name, or any other name under which the Material Subcontractor does business, if any.
|
|
|
3. The address and telephone number of the Material Subcontractor’s headquarters office.
|
|
|
4. The type of ownership (e.g., proprietary, partnership, corporation).
|
|
|
5. The type of incorporation (i.e., for profit, not-for-profit, or non-profit) and whether the Material Subcontractor is publicly or privately owned.
|
|
|
6. If a Subsidiary or Affiliate, the identification of the parent organization.
|
|
|
7. The name and address of any sponsoring corporation or others who provide financial support to the Material Subcontractor and type of support, e.g., guarantees, letters of credit, etc. Indicate if there are maximum limits of the additional financial support.
|
|
|
8. The name and address of any health professional that has at least a five percent (5%) financial interest in the Material Subcontractor and the type of financial interest.
|
|
|
9. The state in which the Material Subcontractor is incorporated, commercially domiciled, and the state(s) in which the organization is licensed to do business.
|
|
|
10. The Material Subcontractor’s Texas Provider Identifier if Medicaid-enrolled in Texas.
|
|
|
11. The Material Subcontractor’s federal taxpayer identification number.
|
|
|
12. Whether the Material Subcontractor had a contract terminated or not renewed for non-performance or poor performance within the past five years. In such instance, the Contractor must describe the issues and the parties involved, and provide the address and telephone number of the principal terminating party. The Contractor must also describe any corrective action taken to prevent any future occurrence of the problem leading to the termination.
|
|
|
13. Whether the Material Subcontractor has ever sought, or is currently seeking, National Committee for Quality Assurance (NCQA) or American Accreditation HealthCare Commission (URAC) accreditation or certification status, and if it has or is, indicate:
|
|
|
• its current NCQA or URAC accreditation or certification status;
|
|
|
• if NCQA or URAC accredited or certified, its accreditation or certification term effective dates; and
|
|
|
• if not accredited, a statement describing whether and when NCQA or URAC accreditation status was ever denied the Material Subcontractor.
|
|
|
1. Submit an organizational chart (labeled Chart A), showing the corporate structure and lines of responsibility and authority in the administration of the Bidder’s business as a health plan.
|
|
|
2. Submit an organizational chart (labeled Chart B) showing the Texas organizational structure and how it relates to the proposed Service Area(s), including staffing and functions performed at the local level. If Chart A represents the entire organizational structure, label the submission as Charts A and B.
|
|
|
3. Submit an organizational chart (labeled Chart C) showing the Management Information System (MIS) staff organizational structure and how it relates to the proposed Service Area(s) including staffing and functions performed at the local level.
|
|
|
4. If the Bidder is proposing to use a Material Subcontractor(s), the Bidder shall include an organizational chart demonstrating how the Material Subcontractor(s) will be managed within the Bidder’s Texas organizational structure, including the primary individuals at the Bidder’s organization and at each Material Subcontractor organization responsible for overseeing such Material Subcontract. This information may be included in Chart B, or in a separate organizational chart(s).
|
|
|
5. Submit a brief narrative explaining the organizational charts submitted, and highlighting the key functional responsibilities and reporting requirements of each organizational unit relating to the Bidder’s proposed management of the HMO Program(s), including its management of any proposed Material Subcontractors.
|
|
|
1. Briefly describe any regulatory action, sanctions, and/or fines imposed by any federal or Texas regulatory entity or a regulatory entity in another state within the last 3 years, including a description of any letters of deficiencies, corrective actions, findings of non-compliance, and/or sanctions. Please indicate which of these actions or fines, if any, were related to Medicaid or CHIP programs. HHSC may, at its option, contact these clients or regulatory agencies and any other individual or organization whether or not identified by the Contractor.
|
|
|
2. No later than ten (10) days after the Contract Effective Date, submit documentation that demonstrates that the HMO has secured the required insurance and bonds in accordance with TDI requirements and Attachment B-1, Section 8.
|
|
|
3. Submit annual audited financial statement for fiscal years 2004 and 2005 (2005 to be submitted no later than six months after the close of the fiscal year).
|
|
|
4. Submit an Affiliate Report containing a list of all Affiliates and for HHSC’s prior review and approval, a schedule of all transactions with Affiliates that, under the provisions of the Contract, will be allowable as expenses in the FSR Report for services provided to the HMO by the Affiliate. Those should include financial terms, a detailed description of the services to be provided, and an estimated amount that will be incurred by the HMO for such services during the Contract Period.
|
|
|
7.3.1.4 System Testing and Transfer of Data
|
|
|
7.3.1.5 System Readiness Review
|
|
|
1. Joint Interface Plan.
|
|
|
2. Disaster Recovery Plan
|
|
|
3. Business Continuity Plan
|
|
|
4. Risk Management Plan, and
|
|
|
5. Systems Quality Assurance Plan.
|
|
|
7.3.1.6 Demonstration and Assessment of System Readiness
|
|
|
7.3.1.7 Operations Readiness
|
|
|
1. Develop new, or revise existing, operations procedures and associated documentation to support the HMO’s proposed approach to conducting operations activities in compliance with the contracted scope of work.
|
|
|
2. Submit to HHSC, a listing of all contracted and credentialed Providers, in a HHSC approved format including a description of additional contracting and credentialing activities scheduled to be completed before the Operational Start Date.
|
|
|
3. Prepare and implement a Member Services staff training curriculum and a Provider training curriculum.
|
|
|
4. Prepare a Coordination Plan documenting how the HMO will coordinate its business activities with those activities performed by HHSC contractors and the HMO’s Material Subcontractors, if any. The Coordination Plan will include identification of coordinated activities and protocols for the Transition Phase.
|
|
|
5. Develop and submit to HHSC the draft Member Handbook, draft Provider Manual, draft Provider Directory, and draft Member Identification Card for HHSC’s review and approval. The materials must at a minimum meet the requirements specified in Section 8.1.5 and include the Critical Elements to be defined in the HHSC Uniform Managed Care Manual.
|
|
|
6. Develop and submit to HHSC the HMO’s proposed Member complaint and appeals processes for Medicaid, CHIP, and CHIP Perinatal as applicable to the HMO’s Program participation.
|
|
|
7. Provide sufficient copies of the final Provider Directory to the HHSC Administrative Services Contractor in sufficient time to meet the enrollment schedule.
|
|
|
8. Demonstrate toll-free telephone systems and reporting capabilities for the Member Services Hotline, the Behavioral Health Hotline, and the Provider Services Hotline.
|
|
|
9. Submit a written Fraud and Abuse Compliance Plan to HHSC for approval no later than 30 days after the Contract Effective Date. See Section 8.1.19, Fraud and Abuse, for the requirements of the plan, including new requirements for special investigation units. As part of the Fraud and Abuse Compliance Plan, the HMO shall:
|
|
|
• designate executive and essential personnel to attend mandatory training in fraud and abuse detection, prevention and reporting. Executive and essential fraud and abuse personnel means HMO staff persons who supervise staff in the following areas: data collection, provider enrollment or disenrollment, encounter data, claims processing, utilization review, appeals or grievances, quality assurance and marketing, and who are directly involved in the decision-making and administration of the fraud and abuse detection program within the HMO. The training will be conducted by the Office of Inspector General, Health and Human Services Commission, and will be provided free of charge. The HMO must schedule and complete training no later than 90 days after the Effective Date.
|
|
|
• designate an officer or director within the organization responsible for carrying out the provisions of the Fraud and Abuse Compliance Plan.
|
|
|
• The HMO is held to the same requirements and must ensure that, if this function is subcontracted to another entity, the subcontractor also meets all the requirements in this section and the Fraud and Abuse section as stated in Attachment B-1, Section 8.
|
|
|
• Note: STAR+PLUS HMOs who have already submitted and received HHSC’s approval for their Fraud and Abuse Compliance Plans must submit acknowledgement that the HMO’s approved Fraud and Abuse Compliance Plan also applies to the STAR+PLUS program, or submit a revised Fraud and Abuse Compliance Plan for HHSC’s approval, with an explanation of changes to be made to incorporate the STAR+PLUS program into the plan, by July 10, 2006.
|
|
|
• CHIP Perinatal HMOs who have already submitted and received HHSC’s approval for their Fraud and Abuse Compliance Plans must submit acknowledgement that the HMO’s approved Fraud and Abuse Compliance Plan also applies to the CHIP Perinatal Program, or submit a revised Fraud and Abuse Compliance Plan for HHSC’s approval, with an explanation of changes to be made to incorporate the CHIP Perinatal program into the plan, by September 15, 2006.
|
|
|
• Complete hiring and training of STAR+PLUS Service Coordination staff, no later than 45 days prior to the STAR+PLUS Operational Start Date.
|
|
|
7.3.1.8 Assurance of System and Operational Readiness
|
|
|
7.3.1.9 Post-Transition
|
|
|
1. freeze enrollment into the HMO’s plan for the affected HMO Program(s) and Service Area(s);
|
|
|
2. freeze enrollment into the HMO’s plan for all HMO Programs or for all Service Areas of an affected HMO Program;
|
|
|
3. impose contractual remedies, including liquidated damages; or
|
|
|
4. pursue other equitable, injunctive, or regulatory relief.
|
|
DOCUMENT HISTORY LOG
|
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
|
Baseline
|
n/a
|
Initial version Attachment B-1, Section 8
|
||
|
Revision
|
1.1
|
June 30, 2006
|
Revised version of the Attachment B-1, Section 8, that includes provisions applicable to MCOs participating in the STAR+PLUS Program.
Section 8.1.1.1, Performance Evaluation, is modified to include STAR+PLUS Performance Improvement Goals.
Section 8.1.2, Covered Services, is modified to include Functionally Necessary Community Long-term Care Services for STAR+PLUS.
Section 8.1.2.1 Value-Added Services, is modified to add language allowing for the HMO to distinguish between the Dual Eligible and non-Dual Eligible populations.
Section 8.1.2.2 Case-by-Case Added Services, is modified to clarify for STAR+Plus members it is based on functionality.
Section 8.1.3, Access to Care, is modified to include STAR+PLUS Functional Necessity and 1915(c) Nursing Facility Waiver clarifications.
Section 8.1.4, Provider Network, is modified to include STAR+PLUS.
Section 8.1.4.2, Primary Care Providers, is modified to include STAR+PLUS
Section 8.1.4.8, Provider Reimbursement, is modified to include Functionally Necessary Long-term care services for STAR+PLUS.
Section 8.1.7.7, Provider Profiling, is modified to include STAR+PLUS.
Sections 8.1.12 and 8.1.12.2, Services for People with Special Health Care Needs, are modified to include STAR+PLUS.
Section 8.1.13, Service Management for Certain Populations, is modified to include STAR+PLUS.
Section 8.1.14, Disease Management, is modified to include STAR+PLUS.
Section 8.2, Additional Medicaid HMO Scope of Work, is modified to include STAR+PLUS.
Section 8.3, Additional STAR+PLUS Scope of Work, is added.
|
|
|
Revision
|
1.2
|
September 1, 2006
|
Revised version of Attachment B-1, Section 8, that includes provisions applicable to MCOs participating in the STAR and CHIP Programs.
Section 8.1.1.1, Performance Evaluation, is modified to clarify that the HMOs goals are Service Area and Program specific; when the percentages for Goals 1 and 2 are to be negotiated; and when Goal 3 is to be negotiated.
Section 8.1.2.1, Value-Added Services, is modified to add language allowing for the addition of two Value-added Services during the Transition Phase of the Contract and to clarify the effective dates for Value Added Services for the Transition Phase and the Operation Phase of the Contract.
Section 8.1.3.2, Access to Network Providers, is modified to delete references to Open Panels.
Section 8.1.4, Provider Network, is modified to clarify that “Out-of-Network reimbursement arrangements” with certain providers must be in writing.
Section 8.1.5.1, Member Materials, is modified to clarify the date that the member ID card and the member handbook are to be sent to members.
Section 8.1.5.6, Member Hotline, is modified to clarify the hotline performance requirements.
Section 8.1.17.2, Financial Reporting Requirements, is modified to clarify that the Bonus Incentive Plan refers to the Employee Bonus Incentive Plan. It has also been modified to clarify the reports and deliverable due dates and to change the name of the Claims Summary Lag Report and clarify that the report format has been moved to the Uniform Managed Care Manual.
Section 8.1.18.5, Claims Processing Requirements, is modified to revise the claims processing requirements and move many of the specifics to the Uniform Managed Care Manual.
Section 8.1.20, Reporting Requirements, is modified to clarify the reports and deliverable due dates.
Section 8.1.20.2, Reports, is modified to delete the Claims Data Specifications Report, amend the All Claims Summary Report, and add two new provider-related reports to the contract.
Section 8.2.2.10, Cooperation with Immunization Registry, is added to comply with legislation, SB 1188 sec. 6(e)(1), 79th Legislature, Regular Session, 2005.
Section 8.2.2.11, Case Management for Children and Pregnant Women, is added.
Section 8.2.5.1, Provider Complaints, is modified to include the 30-day resolution requirement.
Section 8.2.10.2, Non-Reimbursed Arrangements with Local Public Health Entities, is modified to update the requirements and delete the requirement for an MOU.
Section 8.2.11, Coordination with Other State Health and Human Services (HHS) Programs, is modified to update the requirements and delete the requirement for an MOU.
Section 8.4.2, CHIP Provider Complaint and Appeals, is modified to include the 30-day resolution requirement.
|
|
|
Revision
|
1.3
|
September 1, 2006
|
Revised version of Attachment B-1, Section 8, that includes provisions applicable to MCOs participating in the CHIP Perinatal Program.
Section 8.1.1.1, Performance Evaluation, is modified to clarify that HHSC will negotiate and implement Performance Improvement Goals for the first full State Fiscal Year following the CHIP Perinatal Operational Start Date
Section 8.1.2, Covered Services is amended to: (a) clarify that Fee For Service will pay the Hospital costs for CHIP Perinate Newborns; (b) add a reference to new Attachment B-2.2 concerning covered services; (c) add CHIP Perinate references where appropriate.
Section 8.1.2.2 Case-by-Case Added Services, is modified to clarify that this does not apply to the CHIP Perinatal Program.
Section 8.1.3, Access to Care, is amended to include emergency services limitations.
Section 8.1.3.2, Access to Network Providers, is amended to include the Provider access standards for the CHIP Perinatal Program.
Section 8.1.4.2 Primary Care Providers, is modified to clarify the development of the PCP networks between the CHIP Perinates and the CHIP Perinate Newborns.
Section 8.1.4.6 Provider Manual, Materials and Training, modified to include the CHIP Perinatal Program
Section 8.1.4.9 Termination of Provider Contracts modified to include the CHIP Perinatal Program.
Section 8.1.5.2 Member Identification (ID) Card, modified to include the CHIP Perinatal Program.
Section 8.1.5.3 Member Handbook, modified to include the CHIP Perinatal Program.
Section 8.1.5.4 Provider Directory, modified to include the CHIP Perinatal Program.
Section 8.1.5.6 Member Hotline, modified to include the CHIP Perinatal Program.
Section 8.1.5.7 Member Education, modified to include the CHIP Perinatal Program.
Section 8.1.5.9 Member Complaint and Appeal Process, modified to include the CHIP Perinatal Program.
Section 8.1.7.7, Provider Profiling, is modified to include the CHIP Perinatal Program.
Section 8.1.12, Services for People with Special Health Care Needs, modified to clarify between CHIP Perinatal Program and CHIP Perinatal Newborn.
Section 8.1.13, Service Management for Certain Populations, modified to clarify the CHIP Perinatal Program.
Section 8.1.15, Behavioral Health (BH) Network and Services, modified to clarify between CHIP Perinatal and Perinate members.
Section 8.1.17.2, Financial Reporting Requirements, modified to include the CHIP Perinatal Program.
Section 8.1.18.3, System-wide Functions, modified to include the CHIP Perinatal Program.
Section 8.1.18.5, Claims Processing Requirements, modified to include the CHIP Perinatal Program.
Section 8.1.19, Fraud and Abuse, modified to include the CHIP Perinatal Program
Section 8.1.20.2, Provider Termination Report and Provider Network Capacity Report, is modified to include the CHIP Perinatal Program.
Section 8.5, Additional Scope of Work for CHIP Perinatal Program HMOs, is added to Attachment B-1.
|
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment did not revise Attachment B-1, Section 8-Operations Phase Requirements.
|
|
|
Revision
|
1.5
|
January 1, 2007
|
Revised version of the Attachment B-1, Section 8, that includes provisions applicable to MCOs participating in the STAR and STAR+PLUS Program.
Section 8.1.2 is modified to include a reference to STAR and STAR+PLUS covered services.
Section 8.1.20.2 is modified to update the references to the Uniform Managed Care Manual for the “Summary Report of Member Complaints and Appeals” and the “Summary Report of Provider Complaints.”
Section 8.2.2.5 is modified to require the Provider to coordinate with the Regional Health Authority.
Section 8.2.4 is amended to clarify cost settlements and encounter rates for Federally Qualified Health Centers (FQHCs) and Rural Health Clinics (RHCs) for STAR and STAR+PLUS service areas.
Section 8.3.2.4 is amended to clarify the timeframe for initial STAR+PLUS assessments. Section 8.3.3 is amended to: (1) clarify the use of the DHS Form
2060; (2) require the HMO to complete the Individual Service Plan (ISP), Form 3671 for each Member receiving 1915(c) Nursing Facility Waiver Services; (3) require HMOs to complete Form 3652 and Form 3671annually at reassessment; (4) allow the HMOs to administer the Minimum Data Set for Home Care (MDS-HC) instrument for non-waiver STAR+PLUS Members over the course of the first year of operation; (5) allow HMOs to submit other supplemental assessment instruments.
Section 8.3.4 is modified to include the criteria for participation in 1915(c) nursing facility waiver services.
Section 8.3.4.3 is amended to remove the six-month timeframe for Nursing Facility Cost Ceiling. Deletes provision stating DADS Commissioner may grant exceptions in individual cases.
Section 8.3.5 is amended to delete the requirement that HMOs use the Consumer Directed Services option for the delivery of Personal Attendant Services. The new language provides HMOs with three options for delivering these services. The options are described in the following new subsections: 8.3.5.1, Personal Attendant Services Delivery Option – Self-Directed Model; 8.3.5.2, Personal Attendant Services Delivery Option – Agency Model, Self-Directed; and 8.3.5.3, Personal Attendant Services Delivery Option – Agency Model.
Section 8.3.7.3 is modified to reflect the changes made by the HMO workgroup regarding enhanced payments for attendant care. The section also includes a reference to new Attachment B-7, which contains the HMO’s methodology for implementing and paying the enhanced payments.
|
|
|
Revision
|
1.6
|
February 1, 2007
|
Revised version of the Attachment B-1, Section 8, that includes provisions applicable to MCOs participating in the STAR+PLUS and CHIP Perinatal Programs.
Section 8.1 is modified to clarify the Operational Start Date of the STAR+PLUS Program.
Section 8.1.3.2 is modified to allow exceptions to hospital access standards on a case-by-case basis only for HMOs participating in the CHIP Perinatal Program.
Section 8.3.3 is modified to clarify when the 12-month period begins for the STAR+PLUS HMOs to complete the MDS-HC instruments for non-1915(c) Nursing Facility Waiver Members who are receiving Community-based Long-term Care Services.
|
|
|
Revision
|
1.7
|
July 1, 2007
|
New Section 8.1.1.2 is added to require the HMOs to pay for any additional readiness reviews beyond the original ones conducted before the Operational Start Date.
Section 8.1.5.5 is modified to add a requirement that all HMOs must list Home Health Ancillary providers on their websites, with an indicator for Pediatric services.
Section 8.1.17.2 is modified to remove the requirement that the Claims Lag Report separate claims by service categories.
Section 8.1.18 is modified to update the cross-references to sections of the contract addressing remedies and damages and to add cross-references to sections of the contract addressing Readiness Reviews.
Section 8.1.18.5 is modified to require the HMO to make an electronic funds transfer payment process available when processing claims for Medically Necessary covered STAR+PLUS services.
Section 8.1.19 is modified to comply with a new federal law that requires entities that receive or make Medicaid payments of at least $5 million annually to educate employees, contractors and agents and to implement policies and procedures for detecting and preventing fraud, waste and abuse.
Section 8.1.20.2 is modified to require Provider Termination Reports for STAR+PLUS as required by the Dashboard. The amendment also requires Claims Summary Reports be submitted by claim type.
Section 8.2.7.5 is modified to comply with the settlement agreement in the Alberto N. litigation.
Section 8.3.4.3 is modified to remove references to the cost cap for 1915(c) Nursing Facility Waiver services.
|
|
|
Revision
|
1.8
|
September 1, 2007
|
Section 8.1.2.1 is modified to reflect legislative changes required by SB 10.
Section 8.1.3.2 is modified to reflect legislative changes required by SB 10.
Section 8.1.5.6 is modified to comply with the Frew litigation corrective action plans.
New Section 8.1.5.6.1 is added to comply with the Frew litigation corrective action plans.
Section 8.1.5.7 is modified to comply with the Frew litigation corrective action plans.
Section 8.1.11 is modified to delete language included in error and to clarify the coverage for children in foster care.
Section 8.1.13 is added to comply with the Frew litigation corrective action plans.
Section 8.1.17.2 is modified to reflect legislative changes required by SB 10.
Section 8.1.20.2 is modified to comply with the Frew litigation corrective action plans by adding two new reports: Medicaid Medical Check-ups Report and Medicaid FWC Report.
Section 8.2.2.3 is modified to comply with Frew litigation correction action plans.
New Section 8.2.2.12 is added to comply with the Frew litigation correction action plans to enhance care for children of Migrant Farmworkers. Section 8.2.4 is modified to clarify cost settlement requirements and
encounter and payment reporting requirements for the Nueces Service Area and the STAR+PLUS Service Areas.
Section 8.2.7.4 is amended to reflect the new fair hearings process for Medicaid Members that will be effective 9/1/07.
Section 8.2.11 is modified to comply with the Frew litigation corrective action plans.
|
|
|
Revision
|
1.9
|
December 1, 2007
|
Section 8.1.17.1 is modified to include provider contracts in the documentation HMOs must provide upon request and the timeframes in which documents must be provided.
Section 8.1.17.2 is modified to eliminate the plan's responsibility to submit the actuarial certification on the 90 day FSR.
Section 8.1.20.2 is modified to change the name of the Medicaid Medical Check-ups Report to the Medicaid Managed Care Texas Health Steps Medical Checkups Annual Report (90-Day FREW Report) and to clarify the term “not previously enrolled”.
Section 8.2.2.8 is modified to reflect changes as a result of the Alberto N litigation Second Partial Settlement Agreement. Services for person under age 21 are being carved out of the STAR Program and provided through the Personal Care Services (PCS) benefit in traditional Medicaid Fee-for-Service.
Section 8.2.7.4 is modified to clarify the HMO’s role in filling out the request for Fair Hearing and to conform to Fair Hearings time requirements.
Section 8.2.12 is modified to remove the outdated reference to 42 C.F.R. 434.28.
Section 8.3.4 is modified to specify that plan of care at initial determination must be 200% or less of nursing facility cost.
Section 8.3.5 is modified to clarify when the HMO must provide PAS information to Members receiving PAS services.
|
|
| Revision | 1.10 | March 31, 2008 |
Section 8.1.4.4 is modified to add language regarding expedited credentialing as required by HB 1594.
Section 8.1.12.2 is modified to transfer the Medical Transportation Program back to HHSC.
Section 8.1.17 is modified to add a reference to Federal Acquisition Regulations (“FAR”).
Section 8.1.20.2 is modified to change the name of the Medicaid FWC Report to the Children of Migrant Farm Workers Annual Report (FWC Annual Report) Section 8.2.4 is modified to include Municipal Health Department’s Public Clinics.
|
|
| Revision | 1.11 | September 1, 2008 |
Section 8.1.4 is modified to reflect waiver requirements.
Section 8.1.4.2 is modified to remove the “Pediatric and Family” qualifier from Advanced Practice Nurses.
Section 8.1.4.7 is modified to require the HMOs to pay all reasonable costs for HHSC to conduct onsite monitoring of the HMO’s Provider Hotline functions.
Section 8.1.5.6 is modified to require the HMOs to pay all reasonable costs for HHSC to conduct onsite monitoring of the HMO’s Member Hotline functions.
Section 8.1.14 is modified to require the HMO to coordinate continuity of care for Members in Disease Management who change plans.
Section 8.1.15.3 is modified to clarify the first sentence.
Section 8.1.18.1 is modified to clarify encounter data submission requirements.
Section 8.1.18.2 is modified to require HMOs to follow applicable JIPs and required field submissions. This requirement has been moved from Attachment B-1, Section 8.1.20.2.
Section 8.1.20.2 is modified to require the HMOs to submit copies of all internal and external audit reports. The requirement to follow applicable JIPs and required field submissions has been moved to Attachment B-1, Section 8.1.18.2.
Section 8.2.1 is modified to add a cross reference to Section 8.1.14 for specific requirements for Members transferring to and from the HMO’s DM Program.
Section 8.2.2.3.1 is added to require the HMO to educate Texas Health Steps providers on the availability of the Oral Evaluation and Fluoride Varnish (OEVS) Medicaid benefit.
Section 8.2.4 is modified to require the HMOs to pay full encounter rates to RHCs on or after September 1, 2008.
Section 8.2.7.2 is modified to align contract references to TDI’s recodification.
Section 8.3.3 is modified to reflect current Waiver requirements and the conversion from the TILE to the RUG assessment instrument.
Section 8.3.4.1 is modified to reflect the conversion from the TILE to the RUG assessment instrument.
Section 8.3.4.2 is modified to reflect the conversion from the TILE to the RUG assessment instrument.
Section 8.3.4.3 is modified to reflect current Waiver requirements and the conversion from the TILE to the RUG assessment instrument.
|
|
| Revision | 1.12 | March 1, 2009 |
Section 8.1.2.1 is modified to conform to timeframes for the Health Plan Comparison Chart process.
Section 8.1.4 is modified to include performance standards for out of network utilization.
Section 8.1.5.5 is modified to require the HMOs to update their online provider directory at least twice a month.
Section 8.1.5.6 is modified to clarify the maximum acceptable hold time.
Section 8.1.15.3 is modified to clarify the maximum acceptable hold time and to require the HMOs to pay all reasonable costs for HHSC to conduct onsite monitoring of the HMO’s Behavioral Health Hotline functions.
Section 8.1.17.2 is modified to add Bariatric Supplemental Payment Reports and to clarify DSH report language.
Section 8.1.19 is modified to clarify that a written Fraud and Abuse compliance plan must be submitted annually and to list the legal citations.
Section 8.1.20.2 (h) Hotline Reports is modified to correct a contract reference.
Section 8.2.2.8 is modified to reflect that Nursing facilities services will be carved out of the capitation payment to the HMOs.
Section 8.3.2.7 is modified to reflect a corrective action plan required by CMS to address the funding methodology used by HHSC to pay for nursing facility services used by STAR+PLUS members. Nursing facilities services will be carved out of the capitation payment to the HMOs.
Section 8.3.3 is modified to change the name from “Children’s Comprehensive Assessment Form (CCAF Form)” to “Personal Care Assessment Form (PCAF Form)”, to require PCAF reassessments every 12 months, and to allow HMOs until the end of the ISP period to submit the reassessment paperwork.
Section 8.3.4.4 is modified to allow the use of General Revenue to cover costs above the 200% limit.
|
|
| Revision | 1.13 | September 1, 2009 |
All references to “check-ups” are changed to “checkups”
All references to “Medicaid Provider Procedures Manual” are changed to “Texas Medicaid Provider Procedures Manual”
All references to “THSteps” are changed to “Texas Health Steps”
Section 8.1.1.1 is modified to update Goal 3, change SFY2007 to SFY2010, and clarify the applicability of Goals 1 and 2.
Section 8.1.2 is modified to delete the reference to the Texas Health Steps Manual.
Section 8.1.3.1 is amended to change from checkup requirement from “60” days to “90” days and to replace the reference to the AAP periodicity schedule with the Texas Health Steps periodicity schedule.
Section 8.1.3.2 is revised to provide additional clarity as it relates to Qualified Mental Health Providers – Community Services (QMHP-CS).
Section 8.1.4.2 is amended to change the reference from the “THSteps Manual” to the “Texas Medicaid Provider Procedures Manual” and to clarify requirements for CHIP and Medicaid.
Section 8.1.17.2 is modified to require CHIP and CHIP Perinatal HMOs to submit TPR reports.
Section 8.1.18.1 is modified in compliance with HB 1218 to require HMOs to submit encounter data not later than the 30th day after the last day of the month in which the claim was adjudicated.
Section 8.1.20.2 (j) is modified to remove the references to “annual”, change “check-ups” to checkups”, and change “90-Day FREW Report” to “Frew 90-Day Reports”.
Section 8.1.20.2 (l) Frew Quarterly Monitoring Report is added.
Section 8.1.20.2 (m) Frew Health Care Provider Training Report is added.
Section 8.2.2.2 is amended to prohibit HMO from requiring pre-authorization for family planning services.
Section 8.2.2.3 is amended to change from checkup requirement from “60” days to “90” days; change the periodicity schedule from “AAP” to “Texas Health Steps”; remove the reference to the Texas Department of Transportation; add “Corrective Action Orders” to the training requirements; change “DSHS THSteps outreach staff” to “the Texas Health Steps outreach unit”; change “again within two weeks from the time of birth” to “in accordance with the Texas Health Steps periodicity schedule”; change “two-week follow-up” to “newborn follow ups”; to spell out the acronym for ACIP; and change “HCFA 1500” to “CMS 1500”.
Section 8.3.2.8 is added to require all STAR+PLUS plans to provide or have applied to provide MA/SNP services in all counties in which they offer STAR+PLUS services.
Section 8.3.5 is amended to change the name from “Personal Attendant Services” to “Consumer Directed Services Options” and “In-Home or Out-of-Home Respite” is added as an option.
Section 8.3.5.1 is amended to delete “Personal Attendant Services Delivery Option” from the name of the section and “In-Home or Out-of-Home Respite” is added as an option.
Section 8.3.5.2 is amended to delete “Personal Attendant Services Delivery Option” from the name of the section and “In-Home or Out-of-Home Respite” is added as an option.
Section 8.3.5.3 is amended to delete “Personal Attendant Services Delivery Option” from the name of the section and “In-Home or Out-of-Home Respite” is added as an option.
Section 8.3.6.3 is modified to remove references to the DADS enhancement program.
Section 8.4.5 Third Party Liability and Recovery is added to clarify the third party recovery requirements for CHIP HMOs.
Section 8.4.6 is added to require CHIP HMOs to pay full encounter rates.
Section 8.5.4 Dental Coverage for CHIP Perinate Newborn Members is added to clarify that the dental coverage requirements applicable to CHIP Members also apply to CHIP Perinate Newborns.
Section 8.5.5 Third Party Liability and Recovery is added to clarify the third party recovery requirements for CHIP Perinatal HMOs.
Section 8.5.6 is added to require CHIP Perinatal HMOs to pay full encounter rates.
|
|
| Revision | 1.14 | December 1, 2009 |
Section 17.02(a) is modified to require the single bond per MCO with a defined term and amount beginning in SFY2010.
Section 8.1.3.2 is revised to update the TAC citation.
Section 8.1.4.4 is amended to add references to 42 C.F.R. §438.12 and 28 T.A.C. §11.1402.
Section 8.1.12.2 is modified to remove references to PACT.
Section 8.1.17.2 DSH Reports is modified to change the report due dates.
Section 8.1.18 is modified to change the notification period from “generally 90 days” to “no later than 180 days prior to the planned change or implementation”.
Section 8.1.18.2 is modified to require HMOs to submit their Disaster Recovery Plan, Business Continuity Plan, and Security Plan annually and to require HMOs to include checklists when submitting modified JIPs, Risk Management Plans and Systems Quality Assurance Plans.
Section 8.2.2.8 is modified to remove references to PACT and to clarify that for STAR+PLUS, while inpatient stays are non-capitated, mental health inpatient stays are capitated.
Section 8.4.6 is modified to omit the CHIP reporting requirement for FQHC and RHC payments.
Section 8.5.6 is modified to omit the CHIP Perinatal Program reporting requirement for FQHC and RHC payments.
|
|
| Revision | 1.15 | March 1, 2010 |
Section 8.1.3.1 is revised to conform to THSteps policy regarding timeliness of medical checkups for existing members ages 36 months and older which will be effective 9/1/10.
Section 8.1.17.2 Financial Disclosure Report is revised to conform to federal requirements.
Section 8.2.2.3 is revised to conform to THSteps policy regarding timeliness of medical checkups for existing members ages 36 months and older which will be effective 9/1/10.
Section 8.2.8.2 “Substance Abuse Benefit” is added. This amendment will be effective the later of: September 1, 2010 or upon final approval of the Medicaid State Plan, 1915(b) STAR+PLUS waiver and/or the 1915(b) STAR waiver, as applicable to the HMO Program.
Section 8.3.6.5 “STAR+PLUS Handbook” is added.
|
|
| Revision | 1.16 | September 1, 2010 |
All references to “Frew vs. Hawkins” are changed to “Frew vs. Suehs”.
Section 8.1.1.1 is modified to establish new Overarching Goals for FY2011 and to remove Service Areas as a category for sub-goals.
Section 8.1.1.2 is modified to change the title to “Additional Readiness Reviews and Monitoring Efforts”, to clarify that HHSC may conduct desk and/or onsite reviews as part of its normal Contract monitoring activities, and to require the HMOs to pay all reasonable costs for HHSC to conduct those onsite reviews.
Section 8.1.2.1 is modified to conform to timeframes for the Health Plan Comparison Chart process.
Section 8.1.4.2 is modified to remove Certified Nurse Midwives and add Advanced Practice Nurses to the list of Providers eligible to be PCPs.
Section 8.1.5.5 is modified to require identification of providers that provide long-term services and supports.
Section 8.1.17.2 Financial Disclosure Report is revised to clarify federal requirements.
Section 8.1.18 is modified to require the HMOs to pay all reasonable costs for HHSC to conduct onsite reviews.
Section 8.1.18.5 is modified to conform to the timeframes for notification in Attachment A, Section 4.08(b)(3).
New Section 8.1.18.6 is added, as required by Section 6507 of the Patient Protection and Affordable Care Act of 2010 (PPACA).
Section 8.1.20.2 (j) is modified to remove “Frew 90-Day Reports” from the name of the report; to clarify what constitutes an Existing Member; and to remove the definition of “New Members”.
Section 8.1.20.2 (n) Frew Provider Recognition Report is added.
Section 8.2.2.8 is amended to clarify disenrollment for utilizing DADS hospice services and to add Span of Coverage exceptions for STAR and STAR+PLUS members described in Attachment A, Section 5.05(a)(2).
Section 8.2.5.1 is modified to add liquidated damages.
Section 8.5.2 is modified to clarify that the HMO not the Provider must respond to Providers’ appeals.
Section 8.2.7.1 is modified to add liquidated damages.
Section 8.2.8.2 “Substance Abuse Benefit” is modified to clarify that this section does not apply to the Dallas Service Area and that HMOs must contract with all qualified interested STPs. This amendment will be effective the later of: September 1, 2010 or upon final approval of the Medicaid State Plan, 1915(b) STAR+PLUS waiver and/or the 1915(b) STAR waiver, as applicable to the HMO Program.
Section 8.2.9 is modified to change “date of service” to “date of adjudication”.
|
|
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment B-1, Section 8-Operations Phase Requirements. | |
| Revision | 1.18 | March 1, 2010 |
Section 8.1.1.1 is modified to change all "Performance Improvement Projects" and to establish new Overarching Goals for FY2011.
Section 8.1.3.2 is revised to be consistent with the TDI requirement to allow pregnant Members past the 24th week of pregnancy to remain under the coare of their current OB/GYN, even if provider is Out-of-Network.
Section 8.1.4.8 is modified to prohibit Medicaid payments to entities located outside the U.S. in conformance with the Affordable Care Act.
Section 8.1.19 is modified to require HMOs to designate a primary and secondary contact for all OIG requests and to outline the process and timeframes for responding to the OIG.
Immunization requirements from Section 8.2.2.3 "Texas Health Steps (EPSDT)" are moved to new Section 8.1.21 "Immunizations" as the requirements apply to both Medicaid and CHIP.
Section 8.2.1 is revised to conform to the TDI requirement to allow pregnant Members past the 24th week of pregnancy to remain under the care of their current OB/GYN, even if provider is Out-of-Network.
Section 8.2.2.3 is modified to reorder requirements and add subsection headings. Additional training requirements are added to the new Section 8.1.21 "Immunizations" as the requirements apply to both Medicaid and CHIP.
Section 8.2.2.4 is amended to clarify that the 45 hour and 96 hour limits do not apply to neonatal care.
Section 8.2.2.8 is amended to add "Texas Health Steps environmental lead investigation (ELI)". Remainder of list is renumbered. In addition, the section is amended to clarify disenrollment for utilizing DADS hospice services to add Span of Coverage exceptions for STAR and STAR+PLUS members described in Attachment A, Section 5.05(a)(2).
Section 8.2.5.1 is revised to add the 98% standard for complaint resolution and to remove the 30 day request for extension requirementfor complaints received directly by the HMO.
Section 8.3.1.1 is modified to change the name from 'Community-based Long-Term Care Services Available to all All Members' to "Community-based Long-Term Services and Supports Available to All Members" and to clarify that "Personal Assistance Services" is also called "Primary Home Care" for (b) Waiver Members.
Section 8.3.1.2 is revised to change the name from "1915(c) Nursing Facility Waiver Services Available to Members Who Qualify for 1915(c) Nursing Facility Waiver Services" to "1915(c) STAR+PLUS Waiver Services Available to Members Who Qualify for 1915(c) STAR+PLUS Waiver Services" and to update the licensure and certification requirements.
Section 8.3.6.6 is added to require STAR+PLUS HMOs to contact Members at least twice a year and to document that contact.
Section 8.4.2 is revised to add the 98% standard for complaint resolution.
|
|
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
||||
|
8. OPERATIONS PHASE REQUIREMENTS
|
|
8.1 General Scope of Work
|
|
|
1. previous coverage, if any, or the reason for termination of such coverage;
|
|
|
2. health status;
|
|
|
3. confinement in a health care facility; or
|
|
|
4. for any other reason.
|
|
|
a. Define and describe the proposed Value-added Service;
|
|
|
b. Specify the Service Areas and HMO Programs for the proposed Value-added Service;
|
|
|
c. Identify the category or group of mandatory Members eligible to receive the Value-added Service if it is a type of service that is not appropriate for all mandatory Members;
|
|
|
d. Note any limits or restrictions that apply to the Value-added Service;
|
|
|
e. Identify the Providers responsible for providing the Value-added Service;
|
|
|
f. Describe how the HMO will identify the Value-added Service in administrative (Encounter) data;
|
|
|
g. Propose how and when the HMO will notify Providers and mandatory Members about the availability of such Value-added Service;
|
|
|
h. Describe how a Member may obtain or access the Value-added Service; and
|
|
|
i. Include a statement that the HMO will provide such Value-added Service for at least 12 months from the September 1 effective date.
|
|
|
(1) HHSC-specified co-payments for CHIP Members, where applicable; and
|
|
|
(2) STAR+PLUS Members who qualify for 1915(c) Nursing Facility Waiver services and enter a 24-hour setting will be required to pay the provider of care room and board costs and any income in excess of the personal needs allowance, as established by HHSC. If the HMO provides Members who do not qualify for the 1915(c) Nursing Facility Waiver services in a 24-hour setting as an alternative to nursing facility or hospitalization, the Member will be required to pay the provider of care room and board costs and any income in excess of the personal needs allowance, as established by HHSC.
|
|
|
1. Emergency Services must be provided upon Member presentation at the service delivery site, including at non-network and out-of-area facilities;
|
|
|
2. Urgent care, including urgent specialty care, must be provided within 24 hours of request.
|
|
|
3. Routine primary care must be provided within 14 days of request;
|
|
|
4. Initial outpatient behavioral health visits must be provided within 14 days of request;
|
|
|
5. Routine specialty care referrals must be provided within 30 days of request;
|
|
|
6. Pre-natal care must be provided within 14 days of request, except for high-risk pregnancies or new Members in the third trimester, for whom an appointment must be offered within five days, or immediately, if an emergency exists;
|
|
|
7. Preventive health services for adults must be offered to a Member within 90 days of request; and
|
|
|
8. Preventive health services for children, including well-child checkups should be offered to CHIP Members in accordance with the American Academy of Pediatrics (AAP) periodicity schedule. Medicaid HMOs should utilize the Texas Health Steps periodicity schedule. For a New Members under age 21, overdue or upcoming well-child checkups, including Texas Health Steps medical checkups, should be offered as soon as practicable, but in no case later than 14 days of enrollment for newborns, and no later than 90 days of enrollment for all other eligible child Members. Effective September 1, 2010, the Texas Health Steps annual medical checkup for an Existing Member age 36 months and older is due on the child’s birthday. The annual medical checkup is considered timely if it occurs no later than 364 calendar days after the child’s birthday. For purposes of this requirement, the terms “New Member” and “Existing Member” are defined in Chapter 12.4 of the Uniform Managed Care Manual.
|
|
|
1. the Provider assumes all HMO PCP responsibilities for such Members in a specific age group under age 21,
|
|
|
2. the Provider has a history of practicing as a PCP for the specified age group as evidenced by the Provider’s primary care practice including an established patient population under age 20 and within the specified age range, and
|
|
|
3. the Provider has admitting privileges to a local hospital that includes admissions to pediatric units.
|
|
|
1. The office telephone is answered after-hours by an answering service, which meets language requirements of the Major Population Groups and which can contact the PCP or another designated medical practitioner. All calls answered by an answering service must be returned within 30 minutes;
|
|
|
2. The office telephone is answered after normal business hours by a recording in the language of each of the Major Population Groups served, directing the patient to call another number to reach the PCP or another provider designated by the PCP. Someone must be available to answer the designated provider’s telephone. Another recording is not acceptable; and
|
|
|
3. The office telephone is transferred after office hours to another location where someone will answer the telephone and be able to contact the PCP or another designated medical practitioner, who can return the call within 30 minutes.
|
|
|
1. The office telephone is only answered during office hours;
|
|
|
2. The office telephone is answered after-hours by a recording that tells patients to leave a message;
|
|
|
3. The office telephone is answered after-hours by a recording that directs patients to go to an Emergency Room for any services needed; and
|
|
|
4. Returning after-hours calls outside of 30 minutes.
|
|
|
1. Covered Services and the Provider’s responsibilities for providing and/or coordinating such services. Special emphasis must be placed on areas that vary from commercial coverage rules (e.g., Early Intervention services, therapies and DME/Medical Supplies); and for Medicaid, making referrals and coordination with Non-capitated Services;
|
|
|
2. Relevant requirements of the Contract;
|
|
|
3. The HMO’s quality assurance and performance improvement program and the Provider’s role in such a program; and
|
|
|
4. The HMO’s policies and procedures, especially regarding in-network and Out-of-Network referrals.
|
|
|
1. 99% of calls are answered by the fourth ring or an automated call pick-up system is used;
|
|
|
2. no more than one percent of incoming calls receive a busy signal;
|
|
|
3. the average hold time is 2 minutes or less; and
|
|
|
4. the call abandonment rate is 7% or less.
|
|
|
1. the Member’s name;
|
|
|
3. the effective date of the PCP assignment (excluding CHIP Perinates);
|
|
|
4. the PCP’s name, address (optional for all products), and telephone number (excluding CHIP Perinates);
|
|
|
5. the name of the HMO;
|
|
|
6. the 24-hour, seven (7) day a week toll-free Member services telephone number and BH Hotline number operated by the HMO; and
|
|
|
7. any other critical elements identified in the Uniform Managed Care Manual.
|
|
|
1. Written in Major Population Group languages (which under this contract include only English and Spanish);
|
|
|
2. Culturally appropriate;
|
|
|
3. Written for understanding at the 6th grade reading level; and
|
|
|
4. Be geared to the health needs of the enrolled HMO Program population.
|
|
|
1. Knowledgeable about Covered Services;
|
|
|
2. Able to answer non-technical questions pertaining to the role of the PCP, as applicable;
|
|
|
3. Able to answer non-clinical questions pertaining to referrals or the process for receiving authorization for procedures or services;
|
|
|
4. Able to give information about Providers in a particular area;
|
|
|
5. Knowledgeable about Fraud, Abuse, and Waste and the requirements to report any conduct that, if substantiated, may constitute Fraud, Abuse, or Waste in the HMO Program;
|
|
|
6. Trained regarding Cultural Competency;
|
|
|
7. Trained regarding the process used to confirm the status of persons with Special Health Care Needs;
|
|
|
8. For Medicaid members, able to answer non-clinical questions pertaining to accessing Non-capitated Services.
|
|
|
9. For Medicaid Members, trained regarding: a) the emergency prescription process and what steps to take to immediately address problems when pharmacies do not provide a 72-hour supply of emergency medicines; and b) DME processes for obtaining services and how to address common problems.
|
|
|
10. For CHIP Members, able to give correct cost-sharing information relating to premiums, co-pays or deductibles, as applicable. (Cost-sharing does not apply to CHIP Perinates or CHIP Perinate Newborns.)
|
|
|
1. 99% of calls are answered by the fourth ring or an automated call pick-up system;
|
|
|
2. no more than one percent (1%) of incoming calls receive a busy signal;
|
|
|
3. at least 80% of calls must be answered by toll-free line staff within 30 seconds measured from the time the call is placed in queue after selecting an option;
|
|
|
4. the call abandonment rate is 7% or less; and
|
|
|
5. the average hold time is 2 minutes or less.
|
|
8.1.5.6.1 Nurseline
|
|
|
1. How the HMO system operates, including the role of the PCP;
|
|
|
2. Covered Services, limitations and any Value-added Services offered by the HMO;
|
|
|
3. The value of screening and preventive care, and
|
|
|
4. How to obtain Covered Services, including:
|
|
|
a. Emergency Services;
|
|
|
b. Accessing OB/GYN and specialty care;
|
|
|
c. Behavioral Health Services;
|
|
|
d. Disease Management programs;
|
|
|
e. Service Coordination, treatment for pregnant women, Members with Special Health Care Needs, including Children with Special Health Care Needs; and other special populations;
|
|
|
f. Early Childhood Intervention (ECI) Services;
|
|
|
g. Screening and preventive services, including well-child care (Texas Health Steps medical checkups for Medicaid Members);
|
|
|
h. For CHIP Members, Member co-payments
|
|
|
i. Suicide prevention;
|
|
|
j. Identification and health education related to Obesity; and
|
|
|
k. Obtaining 72 hour supplies of emergency prescriptions from pharmacies enrolled with HHSC as Medicaid providers.
|
|
|
1. Evaluate performance using objective quality indicators;
|
|
|
2. Foster data-driven decision-making;
|
|
|
3. Recognize that opportunities for improvement are unlimited;
|
|
|
4. Solicit Member and Provider input on performance and QAPI activities;
|
|
|
5. Support continuous ongoing measurement of clinical and non-clinical effectiveness and Member satisfaction;
|
|
|
6. Support programmatic improvements of clinical and non-clinical processes based on findings from on-going measurements; and
|
|
|
7. Support re-measurement of effectiveness and Member satisfaction, and continued development and implementation of improvement interventions as appropriate.
|
|
|
1. Is organization-wide, with clear lines of accountability within the organization;
|
|
|
2. Includes a set of functions, roles, and responsibilities for the oversight of QAPI activities that are clearly defined and assigned to appropriate individuals, including physicians, other clinicians, and non-clinicians;
|
|
|
3. Includes annual objectives and/or goals for planned projects or activities including clinical and non-clinical programs or initiatives and measurement activities; and
|
|
|
4. Evaluates the effectiveness of clinical and non-clinical initiatives.
|
|
2. Establishing PCP, Provider, group, Service Area or regional Benchmarks for areas profiled, where applicable, including STAR, STAR+PLUS, CHIP and CHIP Perinatal Program-specific Benchmarks, where appropriate; and
|
|
3. Providing feedback to individual PCPs and Providers regarding the results of their performance and the overall performance of the Provider Network.
|
|
|
1. Use the results of its Provider profiling activities to identify areas of improvement for individual PCPs and Providers, and/or groups of Providers;
|
|
|
2. Establish Provider-specific quality improvement goals for priority areas in which a Provider or Providers do not meet established HMO standards or improvement goals;
|
|
|
3. Develop and implement incentives, which may include financial and non-financial incentives, to motivate Providers to improve performance on profiled measures; and
|
|
|
4. At least annually, measure and report to HHSC on the Provider Network and individual Providers’ progress, or lack of progress, towards such improvement goals.
|
|
|
1. Procedures to evaluate the need for Medically Necessary Covered Services;
|
|
|
2. The clinical review criteria used, the information sources, the process used to review and approve the provision of Covered Services;
|
|
|
3. The method for periodically reviewing and amending the UM clinical review criteria; and
|
|
|
4. The staff position functionally responsible for the day-to-day management of the UM function.
|
|
|
• Within three (3) business days after receipt of the request for authorization of services;
|
|
|
• Within one (1) business day for concurrent hospitalization decisions; and
|
|
|
• Within one (1) hour for post-stabilization or life-threatening conditions, except that for Emergency Medical Conditions and Emergency Behavioral Health Conditions, the HMO must not require prior authorization.
|
|
|
1. Consistent application of review criteria that are compatible with Members’ needs and situations;
|
|
|
2. Determinations to deny or limit services are made by physicians under the direction of the Medical Director;
|
|
|
3. Appropriate personnel are available to respond to utilization review inquiries 8:00 a.m. to 5:00 p.m., Monday through Friday, with a telephone system capable of accepting utilization review inquiries after normal business hours. The HMO must respond to calls within one business day;
|
|
|
4. Confidentiality of clinical information; and
|
|
|
5. Quality is not adversely impacted by financial and reimbursement-related processes and decisions.
|
|
1. Routinely assess the effectiveness and the efficiency of the UM Program;
|
|
2. Evaluate the appropriate use of medical technologies, including medical procedures, drugs and devices;
|
|
3. target areas of suspected inappropriate service utilization;
|
|
4. Detect over- and under-utilization;
|
|
5. Routinely generate Provider profiles regarding utilization patterns and compliance with utilization review criteria and policies;
|
|
6. Compare Member and Provider utilization with norms for comparable individuals;
|
|
7. Routinely monitor inpatient admissions, emergency room use, ancillary, and out-of-area services;
|
|
|
• A court order (Order) entered by a Court of Continuing Jurisdiction placing a child under the protective custody of TDFPS.
|
|
|
• A TDFPS Service Plan entered by a Court of Continuing Jurisdiction placing a child under the protective custody of TDFPS.
|
|
|
• A TDFPS Service Plan voluntarily entered into by the parents or person having legal custody of a Member and TDFPS.
|
|
|
1. Providing medical records to TDFPS;
|
|
|
2. Scheduling medical and Behavioral Health Services appointments within 14 days unless requested earlier by TDFPS; and
|
|
|
3. Recognition of abuse and neglect, and appropriate referral to TDFPS.
|
|
|
1. Participate in hospital discharge planning;
|
|
|
2. Participate in pre-admission hospital planning for non-emergency hospitalizations;
|
|
|
3. Develop specialty care and support service recommendations to be incorporated into the Service Plan; and
|
|
|
4. Provide information to the Member, or when applicable, the Member’s legal guardian concerning the specialty care recommendations.
|
|
|
• Community Resource Coordination Groups (CRCGs);
|
|
|
• Early Childhood Intervention (ECI) Program;
|
|
|
• Local school districts (Special Education);
|
|
|
• Health and Human Services Commission’s Medical Transportation Program (MTP);
|
|
|
• Texas Department of Assistive and Rehabilitative Services (DARS) Blind Children’s Vocational Discovery and Development Program;
|
|
|
• Texas Department of State Health (DSHS) services, including community mental health programs, and Title V Maternal and Child Health and Children with Special Health Care Needs (CSHCN) Programs;
|
|
|
• Other state and local agencies and programs such as food stamps, and the Women, Infants, and Children’s (WIC) Program;
|
|
|
• Civic and religious organizations and consumer and advocacy groups, such as United Cerebral Palsy, which also work on behalf of the MSHCN population.
|
|
|
1. High-cost catastrophic cases;
|
|
|
2. Women with high-risk pregnancies (STAR and STAR+PLUS Programs only);
|
|
|
3. Individuals with mental illness and co-occurring substance abuse; and
|
|
|
4. FWC (STAR and STAR+PLUS Programs only).
|
|
|
1. Patient self-management education;
|
|
|
2. Provider education;
|
|
|
3. Evidence-based models and minimum standards of care;
|
|
|
4. Standardized protocols and participation criteria;
|
|
|
5. Physician-directed or physician-supervised care;
|
|
|
6. Implementation of interventions that address the continuum of care;
|
|
|
7. Mechanisms to modify or change interventions that are not proven effective; and
|
|
|
8. Mechanisms to monitor the impact of the DM Program over time, including both the clinical and the financial impact.
|
|
|
1. Implement a system for Providers to request specific DM interventions;
|
|
|
2. Give Providers information, including differences between recommended prevention and treatment and actual care received by Members enrolled in a DM Program, and information concerning such Members’ adherence to a service plan; and
|
|
|
3. For Members enrolled in a DM Program, provide reports on changes in a Member’s health status to their PCP.
|
|
|
1. 99% of calls are answered by the fourth ring or an automated call pick-up system;
|
|
|
2. no incoming calls receive a busy signal;
|
|
|
3. at least 80% of calls must be answered by toll-free line staff within 30 seconds measured from the time the call is placed in queue after selecting an option;
|
|
|
4. the call abandonment rate is 7% or less; and
|
|
|
5. the average hold time is 2 minutes or less.
|
|
|
1. Maintain accounting records for each applicable HMO Program separate and apart from other corporate accounting records;
|
|
|
2. Maintain records for all claims payments, refunds and adjustment payments to providers, capitation payments, interest income and payments for administrative services or functions and must maintain separate records for medical and administrative fees, charges, and payments;
|
|
|
3. Maintain an accounting system that provides an audit trail containing sufficient financial documentation to allow for the reconciliation of billings, reports, and financial statements with all general ledger accounts; and
|
|
|
4. Within 60 days after Contract execution, submit an accounting policy manual that includes all proposed policies and procedures the HMO will follow during the duration of the Contract. Substantive modifications to the accounting policy manual must be approved by HHSC.
|
|
|
1. Cooperate with the State and federal governments in their evaluation, inspection, audit, and/or review of accounting records and any necessary supporting information;
|
|
|
2. Permit authorized representatives of the State and federal governments full access, during normal business hours, to the accounting records that the State and the Federal government determine are relevant to the Contract. Such access is guaranteed at all times during the performance and retention period of the Contract, and will include both announced and unannounced inspections, on-site audits, and the review, analysis, and reproduction of reports produced by the HMO;
|
|
|
3. Make copies of any accounting records or supporting documentation relevant to the Contract, including Network Provider agreements, available to HHSC or its agents within seven (7) Business Days, or as otherwise specified by HHSC, of receiving a written request from HHSC for specified records or information. If such documentation is not made available as requested, the HMO agrees to reimburse HHSC for all costs, including, but not limited to, transportation, lodging, and subsistence for all State and federal representatives, or their agents, to carry out their inspection, audit, review, analysis, and reproduction functions at the location(s) of such accounting records; and
|
|
|
4. Pay any and all additional costs incurred by the State and federal government that are the result of the HMO’s failure to provide the requested accounting records or financial
|
|
|
information within ten (10) business days of receiving a written request from the State or federal government.
|
|
|
1. A list of all Affiliates, and
|
|
|
2. For HHSC’s prior review and approval, a schedule of all transactions with Affiliates that, under the provisions of the Contract, will be allowable as expenses in the FSR Report for services provided to the HMO by the Affiliate. Those should include financial terms, a detailed description of the services to be provided, and an estimated amount that will be incurred by the HMO for such services during the Contract Period.
|
|
|
• unduplicated reports of bariatric surgeries;
|
|
|
• bariatric surgeries that the HMO has paid under the group of procedure codes defined as allowable for bariatric reimbursement, as designated in the “Texas Medicaid Providers Procedures Manual”, including the Texas Medicaid Bulletins; and
|
|
|
• bariatric surgeries that were performed no earlier than 210 days prior to the date HHSC receives the Report, or that were included in the Report within thirty days from the date of discharge from the hospital for the stay related to the bariatric surgery, whichever is later. If a medical service provider does not submit a claim to the HMO by the deadline described herein, the HMO may request and exception to include the claim in the BSP report. HHSC may, at its sole discretion, grant or deny the request.
|
|
|
1. a Financial Disclosure Report prior to the start of Operations;
|
|
|
2. an updated Financial Disclosure Report no later than 30 days after the end of each Contract Year; and
|
|
|
3. a “change notification” abbreviated version of the report, no later than 30 days after any of the following events:
|
|
|
a. entering into, renewing, modifying, or terminating a relationship with an affiliated party;
|
|
|
b. after any change in control, ownership, or affiliations; or,
|
|
|
c. after any material change in, or need for addition to, the information previously disclosed.
|
|
|
1. Enrollment/Eligibility Subsystem;
|
|
|
2. Provider Subsystem;
|
|
|
3. Encounter/Claims Processing Subsystem;
|
|
|
4. Financial Subsystem;
|
|
|
5. Utilization/Quality Improvement Subsystem;
|
|
|
6. Reporting Subsystem;
|
|
|
7. Interface Subsystem; and
|
|
|
8. TPR Subsystem, as applicable to each HMO Program.
|
|
|
1. A new plan is brought into the HMO Program;
|
|
|
2. An existing plan begins business in a new Service Area;
|
|
|
3. An existing plan changes location;
|
|
|
4. An existing plan changes its processing system, including changes in Material Subcontractors performing MIS or claims processing functions; and
|
|
|
5. An existing plan in one or two HHSC HMO Programs is initiating a Contract to participate in any additional HMO Programs.
|
|
|
1. Joint Interface Plan;
|
|
|
2. Risk Management Plan; and
|
|
|
3. Systems Quality Assurance Plan.
|
|
|
1. Process electronic data transmission or media to add, delete or modify membership records with accurate begin and end dates;
|
|
|
2. Track Covered Services received by Members through the system, and accurately and fully maintain those Covered Services as HIPAA-compliant Encounter transactions;
|
|
|
3. Transmit or transfer Encounter Data transactions on electronic media in the HIPAA format to the contractor designated by HHSC to receive the Encounter Data;
|
|
|
4. Maintain a history of changes and adjustments and audit trails for current and retroactive data;
|
|
|
5. Maintain procedures and processes for accumulating, archiving, and restoring data in the event of a system or subsystem failure;
|
|
|
6. Employ industry standard medical billing taxonomies (procedure codes, diagnosis codes) to describe services delivered and Encounter transactions produced;
|
|
|
7. Accommodate the coordination of benefits;
|
|
|
8. Produce standard Explanation of Benefits (EOBs);
|
|
|
9. Pay financial transactions to Providers in compliance with federal and state laws, rules and regulations;
|
|
|
10. Ensure that all financial transactions are auditable according to GAAP guidelines.
|
|
|
11. Relate and extract data elements to produce report formats (provided within the Uniform Managed Care Manual) or otherwise required by HHSC;
|
|
|
12. Ensure that written process and procedures manuals document and describe all manual and automated system procedures and processes for the MIS;
|
|
|
13. Maintain and cross-reference all Member-related information with the most current Medicaid, CHIP or CHIP Perinatal Program Provider number; and
|
|
|
14. Ensure that the MIS is able to integrate pharmacy data from HHSC’s Drug Vendor file (available through the Virtual Private Network (VPN)) into the HMO’s Member data.
|
-
1099 data and other financial information - five (5) Business Days.
-
Claims data for sampling - 20 Business Days.
-
Urgent claims data requests - 15 Business Days (with OIG manager's approval).
-
Provider education information - 10 Business Days.
-
Files associated with an HMO conducted investigation - 15 Business Day.
-
Other time-sensitive requests - as needed.
|
|
1. Establish written policies for all employees, managers, officers, contractors, subcontractors, and agents of the HMO, which provide detailed information about the False Claims Act, administrative remedies for false claims and statements, any state laws pertaining to civil or criminal penalties for false claims, and whistleblower protections under such laws, as described in Section 1902(a)(68)(A).
|
|
|
2. Include as part of such written policies, detailed provisions regarding the HMO’s policies and procedures for detecting and preventing fraud, waste, and abuse.
|
|
|
3. Include in any employee handbook a specific discussion of the laws described in Section 1902(a)(68)(A), the rights of employees to be protected as whistleblowers, and the HMO’s policies and procedures for detecting and preventing fraud, waste, and abuse.
|
|
|
1. All information required under the Contract, including but not limited to, the reporting requirements or other information related to the performance of its responsibilities hereunder as reasonably requested by the HHSC; and
|
|
|
2. Any information in its possession sufficient to permit HHSC to comply with the Federal Balanced Budget Act of 1997 or other Federal or state laws, rules, and regulations. All information must be provided in accordance with the timelines, definitions, formats and instructions as specified by HHSC. Where practicable, HHSC may consult with HMOs to establish time frames and formats reasonably acceptable to both parties.
|
|
|
(a) Claims Summary Report - The HMO must submit quarterly Claims Summary Reports to HHSC by HMO Program, Service Area and claim type by the 30th day following the end of the reporting period unless otherwise specified. Claim Types include facility and/or professional services for Acute Care, Behavioral Health, Vision, and Long Term Services and Supports. Within each claim type, claims data must be reported separately on the UB and CMS 1500 claim forms. The format for the Claims Summary Report is contained in Chapter 5, Section 5.6.1 of the Uniform Managed Care Manual.
|
|
|
(b) QAPI Program Annual Summary Report - The HMO must submit a QAPI Program Annual Summary in a format and timeframe as specified in the Uniform Managed Care Manual.
|
|
|
(c) Fraudulent Practices Report - Utilizing the HHSC-Office of Inspector General (OIG) fraud referral form, the HMO’s assigned officer or director must report and refer all possible acts of waste, abuse or fraud to the HHSC-OIG within 30 working days of receiving the reports of possible acts of waste, abuse or fraud from the HMO’s Special Investigative Unit (SIU). The report and referral must include: an investigative report identifying the allegation, statutes/regulations violated or considered, and the results of the investigation; copies of program rules and regulations violated for the time period in question; the estimated overpayment identified; a summary of the interviews conducted; the encounter data submitted by the provider for the time period in question; and all supporting documentation obtained as
|
|
|
the result of the investigation. This requirement applies to all reports of possible acts of waste, abuse and fraud.
|
|
|
(d) Provider Termination Report: (CHIP (including integrated CHIP Perinatal Program data), STAR, and STAR+PLUS) - MCO must submit a quarterly report that identifies any providers who cease to participate in MCO's provider network, either voluntarily or involuntarily. The report must be submitted to HHSC in the format specified by HHSC, no later than 30 days after the end of the reporting period.
|
|
|
(e) PCP Network & Capacity Report: (CHIP only (including integrated CHIP Perinatal Program data)) - For the CHIP Program, MCO must submit a quarterly report listing all unduplicated PCPs in the MCO's Provider Network. For the CHIP Perinatal Program, the Perinatal Newborns are assigned PCPs that are part of the CHIP PCP Network. The report must be submitted to HHSC in the format specified by HHSC, no later than 30 days after the end of the reporting quarter.
|
|
|
(f) Summary Report of Member Complaints and Appeals - The HMO must submit quarterly Member Complaints and Appeals reports. The HMO must include in its reports Complaints and Appeals submitted to its subcontracted risk groups (e.g., IPAs) and any other subcontractor that provides Member services. The HMO must submit the Complaint and Appeals reports electronically on or before 45 days following the end of the state fiscal quarter, using the format specified by HHSC in the HHSC Uniform Managed Care Manual, Chapter 5.4.2.
|
|
|
(g) Summary Report of Provider Complaints - The HMO must submit Provider complaints reports on a quarterly basis. The HMO must include in its reports complaints submitted by providers to its subcontracted risk groups (e.g., IPAs) and any other subcontractor that provides Provider services. The complaint reports must be submitted electronically on or before 45 days following the end of the state fiscal quarter, using the format specified by HHSC in the HHSC Uniform Managed Care Manual, Chapter 5.4.2.
|
|
|
(h) Hotline Reports - The HMO must submit, on a quarterly basis, a status report for the Member Hotline, the Behavioral Health Services Hotline, and the Provider Hotline in comparison with the performance standards set out in Sections 8.1.5.6, 8.1.15.3, and 8.1.4.7. The HMO shall submit such reports using a format to be prescribed by HHSC in consultation with the HMOs.
|
|
|
(i) Audit Reports – The HMO must comply with the Uniform Managed Care Manual’s requirements regarding notification and/or submission of audit reports.
|
|
|
(j) Medicaid Managed Care Texas Health Steps Medical Checkups Reports – Medicaid HMOs must submit reports identifying the number of New Members and Existing Members receiving Texas Health Steps medical checkups.
|
|
|
(k) Children of Migrant Farm Workers Annual Report (FWC Annual Report) Beginning in SFY 2008, Medicaid HMOs must submit an annual report, in the timeframe and format described in the Uniform Managed Care Manual, about the identification of and delivery of services to children of migrant farm workers (FWC). The report will include a description and results of the each of the following:
|
|
|
(1) the HMO’s efforts to identify as many community and statewide groups that work with FWC as possible within each of its Service Areas;
|
|
|
(2) the HMO’s efforts to coordinate and cooperate with as many of such groups as possible; and
|
|
|
(3) the HMO’s efforts to encourage the community groups to assist in the identification of FWC.
|
|
|
(l) Frew Quarterly Monitoring Report
|
|
|
(m) Frew Health Care Provider Training Report
|
|
|
(n) Frew Provider Recognition Report
|
|
|
1. More than 90 days after a Member enrolls in the HMO’s Program, or
|
|
|
2. For more than nine (9) months in the case of a Member who, at the time of enrollment in the HMO, has been diagnosed with and receiving treatment for a terminal illness and remains enrolled in the HMO.
|
|
|
1. The HMO does not respond to a request for pre-approval within 1 hour;
|
|
|
2. The HMO cannot be contacted; or
|
|
|
3. The HMO representative and the treating physician cannot reach an agreement concerning the Member’s care and a Network physician is not available for consultation. In this situation, the HMO must give the treating physician the opportunity to consult with a Network physician and the treating physician may continue with care of the patient until an HMO physician is reached. The HMO’s financial responsibility ends as follows: the HMO physician with privileges at the treating hospital assumes responsibility for the Member’s care; the HMO physician assumes responsibility for the Member’s care through transfer; the HMO representative and the treating physician reach an agreement concerning the Member’s care; or the Member is discharged.
|
|
|
1. Texas Health Steps benefits;
|
|
|
2. the periodicity schedule for Texas Health Steps medical checkups and immunizations;
|
|
|
3. the required elements of Texas Health Steps medical checkups;
|
|
|
4. providing or arranging for all required lab screening tests (including lead screening), and Comprehensive Care Program (CCP) services available under the Texas Health Steps program to Members birth through age 20;
|
|
5. Medical Transportation services avilable to Members such as rides to healthcare service by bus, taxi, van, airfare, etc., gas money, mileage reimbursement, meals and lodging when away from home;
|
|
6. importance of updating contact information to ensure accurate provider directories and the Medicaid Online Povider Lookup;
|
|
7. information about HMO's process for acceleration of THSteps services for Children of Migrant Farm Workers;
|
|
8. missed appointment referrals and assistance provided by the THSteps Outreach and Informing Unit; and
|
|
9. administrative issues such as claims filing and services available to Members.
|
HMO must also educate and train Providers regarding the requirements imposed on HHSC and contracting HMOs under the Consent Decree and Corrective Action Orders entered in Frew v. Suehs, et. al., Civil Action No. 3:93CV65, in the United States District Court for the Eastern District of Texas, Paris Division. Providers should be educated and trained to treat each Texas Health Steps visit as an opportunity for a comprehensive assessment of the Member.
|
|
1. Pregnancy planning and perinatal health promotion and education for reproductive- age women;
|
|
|
2. Perinatal risk assessment of non-pregnant women, pregnant and postpartum women, and infants up to one year of age;
|
|
|
3. Access to appropriate levels of care based on risk assessment, including emergency care;
|
|
|
4. Transfer and care of pregnant women, newborns, and infants to tertiary care facilities when necessary;
|
|
|
5. Availability and accessibility of OB/GYNs, anesthesiologists, and neonatologists capable of dealing with complicated perinatal problems; and
|
|
|
6. Availability and accessibility of appropriate outpatient and inpatient facilities capable of dealing with complicated perinatal problems.
|
|
|
1. Texas Health Steps dental (including orthodontia);
|
|
|
2. Texas Health Steps environmental lead investigation (ELI)
|
|
|
3. Early Childhood Intervention (ECI) case management/service coordination;
|
|
|
4. DSHS targeted case management;
|
|
|
5. DSHS mental health rehabilitation;
|
|
|
6. DSHS case management for Children and Pregnant Women;
|
|
|
7. Texas School Health and Related Services (SHARS);
|
|
|
8. Department of Assistive and Rehabilitative Services Blind Children’s Vocational Discovery and Development Program;
|
|
|
9. Tuberculosis services provided by DSHS-approved providers (directly observed therapy and contact investigation);
|
|
|
10. Vendor Drug Program (out-of-office drugs);
|
|
|
11. Health and Human Services Commission’s Medical Transportation;
|
|
|
12. DADS hospice services (all Members are disenrolled from their health plan upon enrollment into hospice except STAR+PLUS members);
|
|
|
13. Audiology services and hearing aids for children (birth through age 20) (hearing screening services are provided through the Texas Health Steps Program and are capitated).
|
|
|
14. For STAR+PLUS, Inpatient Stays are Non-capitated (with the exception of inpatient mental health services, which are capitated).
|
|
|
15. For STAR, Personal Care Services for persons under age 21 are Non-capitated Services.
|
|
|
16. For STAR+PLUS, nursing facility services are Non-capitated Services; and
|
|
|
17. For Members who are enrolled in STAR or STAR+PLUS during and Inpatient Stay under one of the exceptions identified in Attachment A, Section 5.05(a)(2), Hospital facility charges associated with the Inpatient Stay are Non-Capitated Services under the circumstances described in Attachment A, Section 5.05(a)(2)..
|
|
|
• Identification of community and statewide groups that work with FWC Members within the HMO’s Service Areas;
|
|
|
• Participation of the community groups in assisting with the identification of FWC Members;
|
|
|
• Appropriate aggressive efforts to reach each identified FWC to provide timely medical checkups and follow up care if needed;
|
|
|
• Methods to maintain accurate, current lists of all identified FWC Members;
|
|
|
• Methods that the HMO and its Subcontractors will implement to maintain the confidentiality of information about the identity of FWC; and
|
|
|
• Methods to provide accelerated services to FWC.
|
|
|
1. Agree to accept the HMO’s Provider reimbursement rate for the provider type; and
|
|
|
2. Meet the standard credentialing requirements of the HMO, provided that lack of board certification or accreditation by the Joint Commission on Accreditation of Health Care Organizations (JCAHO) is not the sole grounds for exclusion from the Provider Network.
|
|
|
1. Prior to September 1, 2007: For claims accruing prior to September 1, 2007, cost settlements apply to all Service Areas except the Nueces Service Area and the STAR+PLUS Service Areas. The HMOs serving the Nueces Service Area and the STAR+PLUS Service Areas must pay the full encounter rates to the FQHCs and RHCs for claims accruing before September 1, 2007.
|
|
|
2. September 1, 2007 to September 1, 2008: For claims accruing on or after September 1, 2007 but prior to September 1, 2008, HMOs are not required to pay full encounter rates to the FQHCs and RHCs. Therefore, HHSC cost settlements for FQHC’s will continue to apply to all STAR and STAR+PLUS Service Areas for this period of time.
|
|
|
3. On or after September 1, 2008: HMOs are required to pay the full encounter rates to RHCs for claims accruing on or after September 1, 2008; therefore, HHSC cost settlements will not apply to RHCs for this period of time. However, HMOs are not required to pay the full encounter rates to FQHCs for claims accruing on or after September 1, 2008; therefore, HHSC cost settlements will apply to FQHCs for this period of time.
|
|
|
1. the Nueces Service Area and the STAR+PLUS Service Areas for claims accruing before September 1, 2007, since the HMOs in those Areas will pay the full encounter rates to the FQHCs and RHCs for this period of time; and
|
|
|
2. for claims paid to RHCs on or after September 1, 2008, because the HMOs will pay full encounter rates to RHCs for this period of time.
|
|
|
1. Date;
|
|
|
2. Identification of the individual filing the Complaint;
|
|
|
3. Identification of the individual recording the Complaint;
|
|
|
4. Nature of the Complaint;
|
|
|
5. Disposition of the Complaint (i.e., how the HMO resolved the Complaint);
|
|
|
6. Corrective action required; and
|
|
|
7. Date resolved.
|
|
|
1) Date notice is sent;
|
|
|
2) Effective date of the Action;
|
|
|
3) Date the Member or his or her representative requested the Appeal;
|
|
|
4) Date the Appeal was followed up in writing;
|
|
|
5) Identification of the individual filing;
|
|
|
6) Nature of the Appeal; and
|
|
|
7) Disposition of the Appeal, and notice of disposition to Member.
|
|
|
1. The Member or his or her representative files the Appeal timely as defined in this Contract:
|
|
|
2. The Appeal involves the termination, suspension, or reduction of a previously authorized course of treatment;
|
|
|
3. The services were ordered by an authorized provider;
|
|
|
4. The original period covered by the original authorization has not expired; and
|
|
|
5. The Member requests an extension of the benefits.
|
|
|
(1) Transfer the Appeal to the timeframe for standard resolution, and
|
|
|
(2) Make a reasonable effort to give the Member prompt oral notice of the denial, and follow up within two (2) calendar days with a written notice.
|
|
|
2. The Action the HMO has taken or intends to take;
|
|
|
3. The reasons for the Action (If the Action taken is based upon a determination that the requested service is not medically necessary, the HMO must provide an explanation of the medical basis for the decision, application of policy or accepted standards of medical practice to the individuals medical circumstances, in it’s notice to the member.);
|
|
|
4. The Member’s right to access the HMO’s Appeal process.
|
|
|
5. The procedures by which the Member may Appeal the HMO’s Action;
|
|
|
6. The circumstances under which expedited resolution is available and how to request it;
|
|
|
7. The circumstances under which a Member may continue to receive benefits pending resolution of the Appeal, how to request that benefits be continued, and the circumstances under which the Member may be required to pay the costs of these services;
|
|
|
8. The date the Action will be taken;
|
|
|
9. A reference to the HMO policies and procedures supporting the HMO’s Action;
|
|
|
10. An address where written requests may be sent and a toll-free number that the Member can call to request the assistance of a Member representative, file an Appeal, or request a Fair Hearing;
|
|
|
11. An explanation that Members may represent themselves, or be represented by a provider, a friend, a relative, legal counsel or another spokesperson;
|
|
|
12. A statement that if the Member wants a Fair Hearing on the Action, the Member must make the request for a Fair Hearing within 90 days of the date on the notice or the right to request a hearing is waived;
|
|
|
13. A statement explaining that the HMO must make its decision within 30 days from the date the Appeal is received by the HMO, or 3 business days in the case of an Expedited Appeal; and
|
|
|
14. A statement explaining that the hearing officer must make a final decision within 90 days from the date a Fair Hearing is requested.
|
|
|
1. For termination, suspension, or reduction of previously authorized Medicaid-covered services, within the timeframes specified in 42 C.F.R.§§ 431.211, 431.213, and 431.214;
|
|
|
2. For denial of payment, at the time of any Action affecting the claim;
|
|
|
3. For standard service authorization decisions that deny or limit services, within the timeframe specified in 42 C.F.R.§ 438.210(d)(1);
|
|
|
4. If the HMO extends the timeframe in accordance with 42 C.F.R. §438.210(d)(1), it must:
|
|
|
5. give the Member written notice of the reason for the decision to extend the timeframe and inform the Member of the right to file an Appeal if he or she disagrees with that decision; and
|
|
|
6. issue and carry out its determination as expeditiously as the Member’s health condition requires and no later than the date the extension expires;
|
|
|
7. For service authorization decisions not reached within the timeframes specified in 42 C.F.R.§ 438.210(d) (which constitutes a denial and is thus an adverse Action), on the date that the timeframes expire; and
|
|
|
8. For expedited service authorization decisions, within the timeframes specified in 42 C.F.R. 438.210(d).
|
|
|
1. The right to request a Fair Hearing;
|
|
|
2. How to request a Fair Hearing;
|
|
|
3. The circumstances under which the Member may continue to receive benefits pending a Fair Hearing;
|
|
|
4. How to request the continuation of benefits;
|
|
|
5. If the HMO’s Action is upheld in a Fair Hearing, the Member may be liable for the cost of any services furnished to the Member while the Appeal is pending; and
|
|
|
6. Any other information required by 1 T.A.C. Chapter 357 that relates to a managed care organization’s notice of disposition of an Appeal.
|
|
|
1. Their rights and responsibilities,
|
|
|
2. The Complaint process,
|
|
|
3. The Appeal process,
|
|
|
4. Covered Services available to them, including preventive services, and
|
|
|
5. Non-capitated Services available to them.
|
|
1. Describe the Behavioral Health Services indicated in detail in the Provider Procedures Manual and in the Texas Medicaid Bulletin, include the amount, duration, and scope of basic and Value-added Services, and the HMO’s responsibility to provide these services;
|
|
2. Describe criteria, protocols, procedures and instrumentation for referral of Medicaid Members from and to the HMO and the LMHA;
|
|
3. Describe processes and procedures for referring Members with SPMI or SED to the LMHA for assessment and determination of eligibility for rehabilitation or targeted case management services;
|
|
4. Describe how the LMHA and the HMO will coordinate providing Behavioral Health Services to Members with SPMI or SED;
|
|
5. Establish clinical consultation procedures between the HMO and LMHA including consultation to effect referrals and on-going consultation regarding the Member’s progress;
|
|
6. Establish procedures to authorize release and exchange of clinical treatment records;
|
|
7. Establish procedures for coordination of assessment, intake/triage, utilization review/utilization management and care for persons with SPMI or SED;
|
|
8. Establish procedures for coordination of inpatient psychiatric services (including Court- ordered Commitment of Members under 21) in state psychiatric facilities within the LMHA’s catchment area;
|
|
9. Establish procedures for coordination of emergency and urgent services to Members;
|
|
10. Establish procedures for coordination of care and transition of care for new Members who are receiving treatment through the LMHA; and
|
|
|
1. Sexually Transmitted Diseases (STDs) services;
|
|
|
2. Confidential HIV testing;
|
|
|
3. Immunizations;
|
|
|
4. Tuberculosis (TB) care;
|
|
|
5. Family Planning services;
|
|
|
6. Texas Health Steps medical checkups, and
|
|
|
7. Prenatal services.
|
|
|
1. Identify care managers who will be available to assist public health providers and PCPs in efficiently referring Members to the public health providers, specialists, and health-related service providers either within or outside the HMO’s Network; and
|
|
|
2. Inform Members that confidential healthcare information will be provided to the PCP, and educate Members on how to better utilize their PCPs, public health providers, emergency departments, specialists, and health-related service providers.
|
|
|
1. Report to public health entities regarding communicable diseases and/or diseases that are preventable by immunization as defined by state law;
|
|
|
2. Notify the local Public Health Entity, as defined by state law, of communicable disease outbreaks involving Members;
|
|
|
3. Educate Members and Providers regarding WIC services available to Members; and
|
|
|
4. Coordinate with local public health entities that have a child lead program, or with DSHS regional staff when the local public health entity does not have a child lead program, for follow-up of suspected or confirmed cases of childhood lead exposure.
|
|
|
1. Require Providers to use the DSHS Bureau of Laboratories for specimens obtained as part of a Texas Health Steps medical checkup, including Texas Health Steps newborn screens, lead testing, and hemoglobin/hematocrit tests;
|
|
|
2. Notify Providers of the availability of vaccines through the Texas Vaccines for Children Program;
|
|
|
3. Work with HHSC and Providers to improve the reporting of immunizations to the statewide ImmTrac Registry;
|
|
|
4. Educate Providers and Members about the Department of State Health Services (DSHS) Case Management for Children and Pregnant Women (CPW) services available;
|
|
|
5. Coordinate services with CPW specifically in regard to an HMO Member’s health care needs that are identified by CPW and referred to the HMO;
|
|
|
6. Participate, to the extent practicable, in the community-based coalitions with the Medicaid-funded case management programs in the Department of Assistive and Rehabilitative Services (DARS), the Department of Aging and Disability Services (DADS), and DSHS;
|
|
|
7. Cooperate with activities required of state and local public health authorities necessary to conduct the annual population and community based needs assessment;
|
|
|
8. Report all blood lead results, coordinate and follow-up of suspected or confirmed cases of childhood lead exposure with the Childhood Lead Poisoning Prevention Program in DSHS; and
|
|
|
9. Coordinate with Texas Health Steps.
|
|
|
1. A Member’s right to self-determination in making health care decisions;
|
|
|
2. The Advance Directives Act, Chapter 166, Texas Health and Safety Code, which includes:
|
|
|
a. A Member’s right to execute an advance written directive to physicians and family or surrogates, or to make a non-written directive to administer, withhold or withdraw life-sustaining treatment in the event of a terminal or irreversible condition;
|
|
|
b. A Member’s right to make written and non-written out-of-hospital do-not-resuscitate (DNR) orders;
|
|
|
c. A Member’s right to execute a Medical Power of Attorney to appoint an agent to make health care decisions on the Member’s behalf if the Member becomes incompetent; and
|
|
|
3. The Declaration for Mental Health Treatment, Chapter 137, Texas Civil Practice and Remedies Code, which includes: a Member’s right to execute a Declaration for Mental Health Treatment in a document making a declaration of preferences or instructions regarding mental health treatment.
|
|
Community Long-Term Care Services Available to All Members
|
|
|
Service
|
Licensure and Certification Requirements
|
|
Personal Attendant Services/Primary Home Care
|
The Provider must be licensed by DADS as a Home and Community Support Services Agency (HCSSA). The level of licensure required depends on the type of service delivered. NOTE: For primary home care and client managed attendant care, the agency may have only the Personal Assistance Services level of licensure.
|
|
Day Activity and Health Services (DAHS)
|
The Provider must be licensed by DADS Regulatory Division, as an adult day care provider. To provide DAHS, the Provider must provide the range of services required for DAHS.
|
|
Community Long-Term Care Services Under the 1915(c) STAR+PLUS Waiver
|
|
|
Service
|
Licensure and Certification Requirements
|
|
Personal Attendant Services
|
The Provider must be licensed by DADs as a Home and Community Support Services Agency (HCSSA). The level of licensure required depends on the type of service delivered. For Primary Home Care and Client Managed Attendant Care, the agency may have only the Personal Assistance Services level of licensure.
|
|
Assisted Living
|
The Provider must be licensed by the Texas Department of Aging and Disability Services, Long Term Care Regulatory Division in accordance with 40 T.A.C, Part 1, Chapter 92. The type of licensure determines what services may be provided.
|
|
Emergency Response Service Provider
|
Licensed by the Texas Deparement of State Health Services as a Personal Emergency Response Services Agency under T.A.C, Title 25, Part 1, Chapter 140, Subchapter B.
|
| Nursing Services | Licensed Registered Nurse by the Texas Board of Nursing under 22 T.A.C, Part 11, Chapter 217. |
|
Adult Foster Home
|
Adult foster care homes serving three (3) or fewer participants must comply with requirements outlined in 40 TAC, Part 1, Chapter 48, Subchapter K. Adult foster care homes serving four (4) participants must be licensed by DADS as an assisted living facility under 40 TAC Part 1, Chapter 92.
|
| Respite Care | Licensed by DADS as a Home and Community Support Services Agency (HCSSA) under T.A.C., Title 40, Part 1, Chapter 97. |
|
Home Delivered
Meals
|
Providers must comply with requirments for providing home delivered meal services, which include requirements such as dietary requirements, food temperature, delivery times, and training of volunteers and others who deliver meals. In accordance with T.A.C., Title 40, Part 1, Chapter 55.
|
|
Physical
Therapy (PT) Services
|
Licensed Physical Therapist through the Texas Board of Physical Therapy Examiners, Chapter 453.
|
|
Occupational
Therapy (OT) Services
|
Licensed Occupational Therapist through the Texas Board of Occupational Therapy Examiners, Chapter 454.
|
|
Speech, Hearing, and Language Therapy Services
|
Licensed Speech Therapist Through the Department of State Health Services under TAC, Part 32, Chapter 741.
|
|
Consumer Directed Services (CDS)
|
No licensure or certification requirements. Must have completed required training by DADS. CDSAs contracted by DADS are assumed to have completed the training.
|
|
Transition Assistance Services
|
The Provider must comply with the requirements for delivery of TAS, which includes requirements such as allowable purchases, cost limits, and time frames for delivery. TAS providers must demonstrate knowledge of, and experience in, successfully serving individuals who require home and community-based services.
|
|
Minor Home Modification
|
No licensure or certification requirements.
|
|
Adaptive Aids and Medicaid Equipment
|
No licensure or certification requirements.
|
|
Medical supplies
|
No licensure or certification requirements.
|
|
|
1. State/federal agencies (e.g., those agencies with jurisdiction over aging, public health, substance abuse, mental health/retardation, rehabilitation, developmental disabilities, income support, nutritional assistance, family support agencies, etc.);
|
|
|
2. social service agencies (e.g., Area Agencies on Aging, residential support agencies, independent living centers, supported employment agencies, etc.);
|
|
|
3. city and county agencies (e.g., welfare departments, housing programs, etc.);
|
|
|
4. civic and religious organizations; and
|
|
|
5. consumer groups, advocates, and councils (e.g., legal aid offices, consumer/family support groups, permanency planning, etc.).
|
|
|
1. review of existing DADS long-term care services plans;
|
|
|
2. preparation of a transition plan that ensures continuous care under the Member’s existing Care Plan during the transfer into the HMO’s Network while the HMO conducts an appropriate assessment and development of a new plan, if needed;
|
|
|
3. if durable medical equipment or supplies had been ordered prior to enrollment but have not been received by the time of enrollment, coordination and follow-through to ensure that the Member receives the necessary supportive equipment and supplies without undue delay; and
|
|
|
4. payment to the existing provider of service under the existing authorization until the HMO has completed the assessment and service plans and issued new authorizations.
|
|
|
• the state's treatment professionals determine that such placement is appropriate;
|
|
|
• the affected persons do not oppose such treatment; and
|
|
|
• the placement can be reasonably accommodated, taking into account the resources available to the state and the needs of others who are receiving state supported disability services.
|
|
|
• at initial assessment;
|
|
|
• at annual reassessment or annual contact with the STAR+PLUS Member;
|
|
|
• at any time when a STAR+PLUS Member receiving PAS requests the information; and
|
|
|
• in the Member Handbook.
|
|
|
1. Covered Services and the Provider’s responsibilities for providing such services to STAR+PLUS Members and billing the HMO for such services. The HMO must place special emphasis on Community Long-term Care Services and STAR+PLUS requirements, policies, and procedures that vary from Medicaid Fee-for-Service and commercial coverage rules, including payment policies and procedures.
|
|
|
2. Inpatient Stay hospital services and the authorization and billing of such services for STAR+PLUS Members.
|
|
|
3. Relevant requirements of the STAR+PLUS Contract, including the role of the Service Coordinator;
|
|
|
4. Processes for making referrals and coordinating Non-capitated Services;
|
|
|
5. The HMO’s quality assurance and performance improvement program and the Provider’s role in such programs; and
|
|
|
6. The HMO’s STAR+PLUS policies and procedures, including those relating to Network and Out-of-Network referrals.
|
|
8.4 Additional CHIP Scope of Work
|
|
|
1. Agree to accept the HMO’s Provider reimbursement rate for the provider type; and
|
|
|
2. Meet the standard credentialing requirements of the HMO, provided that lack of board certification or accreditation by the Joint Commission on Accreditation of Health Care Organizations (JCAHO) is not the sole grounds for exclusion from the Provider Network.
|
Subject: Attachment B-1 - HHSC Joint Medicia/CHIP HMO RFP, Section 9
|
DOCUMENT HISTORY LOG
|
||||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
|
Baseline
|
n/a
|
Initial version Attachment B-1, Section 7
|
||
|
Revision
|
1.1
|
June 30, 2006
|
Contract amendment to include STAR+PLUS program. No change to this Section.
|
|
|
Revision
|
1.2
|
September 1, 2006
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
|
Revision
|
1.3
|
September 1, 2006
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
|
Revision
|
1.8
|
September 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
| Revision | 1.10 | March 1, 2008 |
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
| Revision | 1.11 | September 1, 2008 |
Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements
|
|
| Revision | 1.12 | March 1, 2009 | Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements | |
| Revision | 1.13 | September 1, 2009 | Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements | |
| Revision | 1.14 | December 1, 2009 | Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements | |
| Revision | 1.15 | March 1, 2010 | Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements | |
| Revision | 1.16 | September 1, 2010 | Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements | |
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment B-1 Section 9 – Turnover Requirements | |
| Revision | 1.18 | March 1, 2011 | Contract amendment did not revise Attachment B-1 Section 9 - Turnover Requirements. | |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
||||
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
n/a
|
Initial version Attachment B-2, Covered Services
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Revised Attachment B-2, Covered Services, by adding Attachment B-2.1, STAR+PLUS Covered Services.
|
|
Revision
|
1.2
|
September 1. 2006
|
Revised Attachment B-2 to include provisions applicable to MCOs participating in the STAR and CHIP Programs.
STAR Covered Services, Services Included under the HMO Capitation Payment, is modified to clarify the STAR covered services related to “optometry” and “vision.”
CHIP Covered Services is modified to correct services related to artificial aids including surgical implants.
|
|
Revision
|
1.3
|
September 1, 2006
|
Contract amendment did not revise Attachment B-2, Covered Services.
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment did not revise Attachment B-2, Covered Services.
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-2, Covered Services.
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-2, Covered Services.
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-2, Covered Services.
|
|
Revision
|
1.8
|
September 1, 2007
|
CHIP Covered Services are modified to comply with legislative changes required by HB 109 to eliminate the 6 month enrollment period effective 9/1/07.
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-2, Covered Services.
|
| Revision | 1.10 | March 1, 2008 |
Contract amendment did not revise Attachment B-2, Covered Services.
|
| Revision | 1.11 | September 1, 2008 | Attachment B-2, Covered Services is modified to include additional covered services resulting from the Frew Settlement. |
| Revision | 1.12 | March 1, 2009 |
Contract amendment did not revise Attachment B-2, Covered Services.
|
| Revision | 1.13 | September 1, 2009 |
All references to “check-ups” are changed to “checkups”
Annual adult well check is removed from the list of enhanced benefits and added to “Services included under the HMO capitation payment”.
STAR Covered Services “Services included under the HMO capitation payment” is modified to remove “birthing center services” and add “Birthing services provided by a certified nurse midwife in a birthing center”.
CHIP Covered Services “Inpatient General Acute and Inpatient Rehabilitation Hospital Services” is modified clarify the requirements regarding miscarriage and non-viable pregnancy, as well as orthodontic services for treatment of craniofacial anomalies.
CHIP Covered Services “Outpatient Hospital, Comprehensive Outpatient Rehabilitation Hospital, Clinic (Including Health Center) and Ambulatory Health Care Center” is modified to clarify the requirements regarding miscarriage and non-viable pregnancy, as well as orthodontic services for treatment of craniofacial anomalies.
CHIP Covered Services “Physician/Physician Extender Professional Services” is modified to clarify the requirements regarding miscarriage and non-viable pregnancy.
CHIP Covered Services “Durable Medical Equipment (DME), Prosthetic Devices and Disposable Medical Supplies” is modified to clarify the requirements regarding dental devices.
CHIP Covered Services “Outpatient Mental Health Services” is revised to provide additional clarity as it relates to Qualified Mental Health Providers – Community Services (QMHP-CS).
CHIP Exclusions From Covered Services is modified to clarify requirements regarding dental devices.
CHIP DME/Supplies is modified to clarify the requirements regarding dental devices.
|
| Revision | 1.14 | December 1, 2009 |
“Services included under the HMO capitation payment” is modified to remove references to PACT.
CHIP Covered Services “Inpatient General Acute and Inpatient Rehabilitation Hospital Services” is modified to clarify the requirements regarding orthodontic services for treatment of craniofacial anomalies. It is also modified to clarify the requirements of Section 2103(f)(2) of the Social Security Act, as amended by CHIPRA. This provision requires CHIP health plans to comply with the Title 42 U.S.C., Chapter 6A, Subchapter XXV, Part A, Subpart 2, 300gg-6.
CHIP Covered Services “Outpatient Hospital, Comprehensive Outpatient Rehabilitation Hospital, Clinic (Including Health Center) and Ambulatory Health Care Center” is modified to clarify the requirements regarding orthodontic services for treatment of craniofacial anomalies. It is also modified to clarify the requirements of Section 2103(f)(2) of the Social Security Act, as amended by CHIPRA. This provision requires CHIP health plans to comply with Title 42 U.S.C., Chapter 6A, Subchapter XXV, Part A, Subpart 2, 300gg-6.
CHIP Covered Services “Physician/Provider Extender Professional Services” is modified to clarify the requirements regarding orthodontic services for treatment of craniofacial anomalies. It is also modified to clarify the requirements of 2103(f)(2) of the Social Security Act, as amended by CHIPRA. This provision requires CHIP health plans to comply with Title 42 U.S.C., Chapter 6A, Subchapter XXV, Part A, Subpart 2, 300gg-6.
CHIP Covered Services “Durable Medical Equipment (DME), Prosthetic Devices and Disposable Medical supplies” is modified to ad external breast prostheses.
CHIP Covered Services “Outpatient Mental Health Services” is revised to update the TAC citation.
|
| Revision | 1.15 | March 1, 2010 |
“Services included under the HMO capitation payment” is modified to add substance abuse services. This amendment will be effective the later of: September 1, 2010 or upon final approval of the Medicaid State Plan, 1915(b) STAR+PLUS waiver and/or the 1915(b) STAR waiver, as applicable to the HMO Program
|
| Revision | 1.16 | September 1, 2010 |
STAR Covered Services is modified to waive the 30 visit limit for outpatient mental health services (as required by Mental Health Parity requirements).
“Services included under the HMO capitation payment” is modified to clarify the substance abuse services; correct the error of adding the general category of “inpatient mental health services for Adults”; and to replace “certified nurse midwife” with “physician or Advanced Practice Nurse” and add the word “licensed” to Birthing Services. In addition, “mastectomy, breast reconstruction, and related follow-up procedures” and “Birthing services provided by a licensed birthing center” are added.
CHIP Covered Services “Inpatient General Acute and Inpatient Rehabilitation Hospital Services” is modified to add “external breast prostheses”.
CHIP Covered Services “Outpatient Hospital, Comprehensive Outpatient Rehabilitation Hospital, Clinic (Including Health Center) and Ambulatory Health Care Center” is modified to add “external breast prostheses”.
CHIP Covered Services “Physician/Physician Extender Professional Services” is modified to add “external breast prostheses”.
|
| Revision | 1.17 | December 1, 2010 | CHIP Hospice Care Services modified to require concurrent CHIP and hospice care services to comply with the federal requirements from Section 2302 of the Patient Protection and Affordable Care Acts of 2010 (P.L. 111-148). By law, CHIP health plans were required to provide concurrent hospice care services effective August 1, 2010. |
| Revision | 1.18 | March 1, 2011 |
Services included under the HMO capitation payment is modified to remove the services effective prior to the effective dates of the State Plan and 1915(b) STAR Waiver.
Services included under the HMO capitation payment is modified to add a reference to "Cancer screening, diagnostic, and treatment services". These services are already 1905(a) covered services, therefore adding this reference does not impact the HMOs' rates.
CHIP Inpatient Mental Health Services is modified to comply with the federal requirements of the Mental Health Parity and Addiction Equity Act of Children's Health Insurance Program Reauthorization Act of 2009 (P.L. 111-3). Also modified to clarify the court-ordered service requirement.
CHIP Inpatient Substance Abuse Treatment Services is modified to comply with the federal requirements of the Mental Health Parity and Additction Equity Act of 2008 (MHPAEA), as applied to CHIP by the Children's Health Insurance Program Reauthorization Act of 2009 (P.L. 111-3).
CHIP Outpatient Substance Abuse Treatment Services is modified to comply with the federal requirements of the Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA) as applied to CHIP by the Children's Health Insurance Program Reauthorization Act of 2009 (P.L. 111-3).
|
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|
|
1) waiver of the three-prescription per month limit;
|
|
|
2) waiver of the 30-day spell-of-illness limitation under fee-for-services; and
|
|
·
|
Ambulance services
|
|
·
|
Audiology services, including hearing aids, for adults (audiology services and hearing aids for children are a non-capitated service)
|
|
·
|
(These services are not subject to the quantitative treatment limitations that apply under traditional, fee-for-service Medicaid coverage. The services may be subject to the HMO's non-quantitative treatmetn limiations, provided such limitations comply with the requirements of the Mental Health Parity and Addiction Equity Act of 2008.) Behavioral Health Services, including:
|
|
·
|
Inpatient mental health services for Children (under age 21)
|
|
·
|
Outpatient mental health services
|
|
·
|
Psychiatry services
|
|
·
|
Counseling services for adults (21 years of age and over)
|
|
·
|
Outpatient substance use disorder treatment services including:
|
|
|
o Assessment
|
|
|
o Detoxification services
|
|
|
o Counseling treatment
|
|
|
o Medication assisted therapy
|
|
·
|
Residential substance use disorder treatment services including:
|
|
|
o Detoxification services
|
|
·
|
Substance use disorder treatment (including room and board)
|
|
·
|
Birthing services provided by a physician or Advanced Practice Nurse in a licensed birthing center
|
|
·
|
Birthing services provided by a licensed birthing center
|
|
·
|
Cancer screening, diagnostic, and treatment services
|
|
·
|
Chiropractic services
|
|
·
|
Dialysis
|
|
·
|
Durable medical equipment and supplies
|
|
·
|
Emergency Services
|
|
·
|
Family planning services
|
|
·
|
Home health care services
|
|
·
|
Hospital services, including inpatient and outpatient
|
|
·
|
Laboratory
|
|
·
|
Mastectomy, breast reconstruction, and related follow-up procedures, including:
|
|
·
|
inpatient services; outpatient services provided at an outpatient hospital and ambulatory health care center as clinically appropriate; and physician and professional services provided in an office, inpatient, or outpatient setting for:
|
|
·
|
all stages of reconstruction on the breast(s) on which medically necessary mastectomy procedure(s) have been performed;
|
|
·
|
surgery and reconstruction on the other breast to produce symmetrical appearance;
|
|
·
|
treatment of physical complications from the mastectomy and treatment of lymphedemas; and
|
|
·
|
prophylactic mastectomy to prevent the development of breast cancer.
|
|
·
|
external breast prosthesis for the breast(s) on which medically necessary mastectomy procedure(s) have been performed.
|
|
·
|
Medical checkups and Comprehensive Care Program (CCP) Services for children (under age 21) through the Texas Health Steps Program
|
|
·
|
Oral evaluation and fluoride varnish in the Medical Home in conjunction with Texas Health Steps medical checkup for children 6 months through 35 months of age.
|
|
·
|
Podiatry
|
|
·
|
Prenatal care
|
|
·
|
Primary care services
|
|
·
|
Preventive services including an annual adult well check for patients 21 years of age and over
|
|
·
|
Radiology, imaging, and X-rays
|
|
·
|
Specialty physician services
|
|
·
|
Therapies – physical, occupational and speech
|
|
·
|
Transplantation of organs and tissues
|
|
·
|
Vision (Includes optometry and glasses. Contact lenses are only covered if they are medically necessary for vision correction, which can not be accomplished by glasses.)
|
|
Covered Benefit
|
Description
|
|
Inpatient General Acute and Inpatient Rehabilitation Hospital Services
|
Services include, but are not limited to, the following:
Hospital-provided Physician or Provider services
Semi-private room and board (or private if medically necessary as certified by attending)
General nursing care
Special duty nursing when medically necessary
ICU and services
Patient meals and special diets
Operating, recovery and other treatment rooms
Anesthesia and administration (facility technical component)
Surgical dressings, trays, casts, splints
Drugs, medications and biologicals
Blood or blood products that are not provided free-of-charge to the patient and their administration
X-rays, imaging and other radiological tests (facility technical component)
Laboratory and pathology services (facility technical component)
Machine diagnostic tests (EEGs, EKGs, etc.)
Oxygen services and inhalation therapy
Radiation and chemotherapy
Access to DSHS-designated Level III perinatal centers or Hospitals meeting equivalent levels of care
In-network or out-of-network facility and Physician services for a mother and her newborn(s) for a minimum of 48 hours following an uncomplicated vaginal delivery and 96 hours following an uncomplicated delivery by caesarian section.
Hospital, physician and related medical services, such as anesthesia, associated with dental care
Inpatient services associated with (a) miscarriage or (b) a non-viable pregnancy (molar pregnancy, ectopic pregnancy, or a fetus that expired in utero). Inpatient services associated with miscarriage or non-viable pregnancy include, but are not limited to:
- dilation and curettage (D&C) procedures;
- appropriate provider-administered medications;
- ultrasounds, and
- histological examination of tissue samples.
Surgical implants
Other artificial aids including surgical implants
Inpatient services for a mastectomy and breast reconstruction include:
- all stages of reconstruction on the affected breast;
- external breast prosthesis for the breast(s) on which medically necessary mastectomy procedure(s) have been performed
- surgery and reconstruction on the other breast to produce symmetrical appearance; and
- treatment of physical complications from the mastectomy and treatment of lymphedemas.
Implantable devices are covered under Inpatient and Outpatient services and do not count towards the DME 12-month period limit
Pre-surgical or post-surgical orthodontic services for medically necessary treatment of craniofacial anomalies requiring surgical intervention and delivered as part of a proposed and clearly outlined plan to treat:
- cleft lip or palate;
- severe skeletal and/or congenital craniofacial deviations; or
- severe facial asymmetry secondary skeletal defects, congenital syndromal conditions and/or tumor growth or its treatment.
|
|
Skilled Nursing
Facilities
(Includes Rehabilitation
Hospitals)
|
Services include, but are not limited to, the following:
Semi-private room and board
Regular nursing services
Rehabilitation services
Medical supplies and use of appliances and equipment furnished by the facility
|
|
Outpatient Hospital, Comprehensive Outpatient Rehabilitation Hospital, Clinic (Including Health Center) and Ambulatory Health Care Center
|
Services include, but are not limited to, the following services provided in a hospital clinic or emergency room, a clinic or health center, hospital-based emergency department or an ambulatory health care setting:
X-ray, imaging, and radiological tests (technical component)
Laboratory and pathology services (technical component)
Machine diagnostic tests
Ambulatory surgical facility services
Drugs, medications and biologicals
Casts, splints, dressings
Preventive health services
Physical, occupational and speech therapy
Renal dialysis
Respiratory services
Radiation and chemotherapy
Blood or blood products that are not provided free-of-charge to the patient and the administration of these products
Outpatient services associated with (a) miscarriage or (b) a non-viable pregnancy (molar pregnancy, ectopic pregnancy, or a fetus that expired in utero). Inpatient services associated with miscarriage or non-viable pregnancy include, but are not limited to:
- dilation and curettage (D&C) procedures;
- appropriate provider-administered medications;
- ultrasounds, and
- histological examination of tissue samples.
Facility and related medical services, such as anesthesia, associated with dental care, when provided in a licensed ambulatory surgical facility.
Surgical implants
Other artificial aids including surgical implants
Outpatient services provided at an oupatient hospital and ambultory health care center for a mastectomy and breast reconstruction as clinically appropriate, include:
- all stages of reconstruction on the affected breast;
- external breast prosthesis for the breast(s) on which medically necessary mastectomy procedure(s) have been performed
- surgery and reconstruction on the other breast to produce symmetrical appearance; and
- treatment of physical complications from mastectomy and treatment of lymphedemas.
Implantable devices are covered under Inpatient and Outpatient services and do not count towards the DME 12-month period limit
Pre-surgical or post-surgical orthodontic services for medically necessary treatment of craniofacial anomalies requiring surgical intervention and delivered as part of a proposed and clearly outlined plan to treat:
- cleft lip or palate;
- severe skeletal and/or congenital craniofacial deviations; or
- severe facial asymmetry secondary skeletal defects, congenital syndromal conditions and/or tumor growth or its treatment.
|
|
Physician/Physician
Extender Professional Services
|
Services include, but are not limited to, the following:
American Academy of Pediatrics recommended well-child exams and preventive health services (including, but not limited to, vision and hearing screening and immunizations)
Physician office visits, in-patient and out-patient services
Laboratory, x-rays, imaging and pathology services, including technical component and/or professional interpretation
Medications, biologicals and materials administered in Physician’s office
Allergy testing, serum and injections
Professional component (in/outpatient) of surgical services, including:
- Surgeons and assistant surgeons for surgical procedures including appropriate follow-up care
- Administration of anesthesia by Physician (other than surgeon) or CRNA
- Second surgical opinions
- Same-day surgery performed in a Hospital without an over-night stay
- Invasive diagnostic procedures such as endoscopic examinations
Hospital-based Physician services (including Physician-performed technical and interpretive components)
Physician and professional services for a mastectomy and breast reconstruction include:
- all stages of reconstruction on the affected breast;
- external breast prosthesis for the breast(s) on which medically necessary mastectomy procedure(s) have been performed
- surgery and reconstruction on the other breast to produce symmetrical appearance; and
- treatment of physical complications from the mastectomy and treatment of lymphedemas.
In-network and out-of-network Physician services for a mother and her newborn(s) for a minimum of 48 hours following an uncomplicated vaginal delivery and 96 hours following an uncomplicated delivery by caesarian section.
Physician services associated with (a) miscarriage or (b) a non-viable pregnancy (molar pregnancy, ectopic pregnancy, or a fetus that expired in utero). Inpatient services associated with miscarriage or non-viable pregnancy include, but are not limited to:
- dilation and curettage (D&C) procedures;
- appropriate provider-administered medications;
- ultrasounds, and
- histological examination of tissue samples.
Physician services medically necessary to support a dentist providing dental services to a CHIP member such as general anesthesia or intravenous (IV) sedation.
Pre-surgical or post-surgical orthodontic services for medically necessary treatment of craniofacial anomalies requiring surgical intervention and delivered as part of a proposed and clearly outlined plan to treat:
- cleft lip or palate;
- severe skeletal and/or congenital craniofacial deviations; or
- severe facial asymmetry secondary skeletal defects, congenital syndromal conditions and/or tumor growth or its treatment.
|
|
Durable Medical Equipment (DME), Prosthetic Devices and
Disposable Medical Supplies
|
$20,000 12-month period limit for DME, prosthetics, devices and disposable medical supplies (diabetic supplies and equipment are not counted against this ccap). Services include DME (equipment which can withstand repeated use and is primarily and customarily used to serve a medical purpose, generally is not useful to a person in the absence of Illness, Injury, or Disability, and is appropriate for use in the home), including devices and supplies that are medically necessary and necessary for one or more activities of daily living and appropriate to assist in the treatment of a medical condition, including:
Orthotic braces and orthotics
Dental devices
Prosthetic devices such as artificial eyes, limbs, braces, and external breast prostheses
Prosthetic eyeglasses and contact lenses for the management of severe ophthalmologic disease
Hearing aids
Diagnosis-specific disposable medical supplies, including diagnosis-specific prescribed specialty formula and dietary supplements. (See Attachment A)
|
|
Home and Community Health Services
|
Services that are provided in the home and community, including, but not limited to:
Home infusion
Respiratory therapy
Visits for private duty nursing (R.N., L.V.N.)
Skilled nursing visits as defined for home health purposes (may include R.N. or L.V.N.).
Home health aide when included as part of a plan of care during a period that skilled visits have been approved.
Speech, physical and occupational therapies.
Services are not intended to replace the CHILD'S caretaker or to provide relief for the caretaker
Skilled nursing visits are provided on intermittent level and not intended to provide 24-hour skilled nursing services
Services are not intended to replace 24-hour inpatient or skilled nursing facility services
|
| Inpatient Mental Health Services |
Mental health services, including for serious mental illness, furnished in a free-standing psychiatric hospital, psychiatric units of general acute care hospitals and state-operated facilities, including, but not limited to:
Neuropsychological and psychological testing.
When inpatient psychiatric services are ordered by a court of competent jurisdiction under the provisions of Chapters 573 and 574 of the Texas Health and Safety Code, relating to court ordered commitments to psychiatric facilities, the court order serves as binding determination of medical necessity. Any modification or termination of services must be presented to the court with juridiction over the matter for determination.
Does not require PCP referral
|
| Outpatient Mental Health Services |
Mental health services, including for serious mental illness, provided on an outpatient basis, including, but not limited to:
The visits can be furnished in a variety of community-based settings (including school and home-based) or in a state-operated facility
Neuropsychological and psychological testing
Medication management
Rehabilitative day treatments
Residential treatment services
Sub-acute outpatient services (partial hospitalization or rehabilitative day treatment)
Skills training (psycho-educational skill development)
When outpatient psychiatric services are ordered by a court of competent jurisdiction under the provisions of Chapters 573 and 574 of the Texas Health and Safety Code, relating to court ordered commitments to psychiatric facilities, the court order serves as binding detemination of medical necessity. Any modification or termination of services must be presented to the court with jursidiction over the matter for determination
A Qualified Mental Health Provider – Community Services (QMHP-CS), is defined by the Texas Department of State Health Services (DSHS) in Title 25 T.A.C., Part I, Chapter 412, Subchapter G, Division 1, §412.303(48). QMHP-CSs shall be providers working through a DSHS-contracted Local Mental Health Authority or a separate DSHS-contracted entity. QMHP-CSs shall be supervised by a licensed mental health professional or physician and provide services in accordance with DSHS standards. Those services include individual and group skills training (which can be components of interventions such as day treatment and in-home services), patient and family education, and crisis services
Does not require PCP referral
|
| Inpatient Substance Abuse Treatment Services |
Services include, but are not limited to:
Inpatient and residential substance abuse treatment services including detoxification and crisis stabilization, and 24-hour residential rehabilitation programs
Does not require PCP referral
|
| Outpatient Substance Abuse Treatment Services |
Outpatient substance abuse treatment services include, but are not limited to, the following:
Prevention and intervention services that are provided by physician and non-physician providers, such as screening, assessment and referral for chemical dependency disorders.
Intensive outpatient services
Partial hospitalization
Intensive outpatient services is defined as an organized non-residential service providing structured group and individual therapy, education services, and life skills training which consists of at least 10 hours per week for four to 12 weeks, but less than 24 hours per day
Outpatient treatement service is defined as consisting of at least one or two hours per week providing structured group and individual therapy, educational services, and life skills training
Does not require PCP referral
|
| Rehabilitation Services |
Services include, but are not limited to, the following:
Habilitation (the process of supplying a child with the means to reach age-appropriate developmental milestones through therapy or treatment) and rehabilitation services include, but are not limited to the following:
Physical, occupational and speech therapy
Developmental assessment
|
| Hospice Care Services |
Services include, but are not limited to, the following:
Palliative care, including medical and support services, for those children who have six months or less to live, to keep patients comfortable during the last weeks and months before death
Treatment services , including treatment related to the terminal illness
Up to a maximum of 120 days with a 6 month life expectancy
Patients electing hospice services may cancel this election at anytime
Services apply to the hospice diagnosis
|
| Emergency Services, including Emergency Hospitals, Physicians, and Ambulance Services |
HMO cannot require authorization as a condition for payment for emergency conditions or labor and delivery.
Covered services include, but are not limited to, the following:
Emergency services based on prudent lay person definition of emergency health condition
Hospital emergency department room and ancillary services and physician services 24 hours a day, 7 days a week, both by in-network and out-of-network providers
Medical screening examination
Stabilization services
Access to DSHS designated Level 1 and Level II trauma centers or hospitals meeting equivalent levels of care for emergency services
Emergency ground, air and water transportation
Emergency dental services, limited to fractured or dislocated jaw, traumatic damage to teeth, and removal of cysts.
|
| Transplants |
Services include, but are not limited to, the following:
Using up-to-date FDA guidelines, all non-experimental human organ and tissue transplants and all forms of non-experimental corneal, bone marrow and peripheral stem cell transplants, including donor medical expenses.
|
| Vision Benefit |
The health plan may reasonably limit the cost of the frames/lenses.
Services include:
One examination of the eyes to determine the need for and prescription for corrective lenses per 12-month period, without authorization
One pair of non-prosthetic eyewear per 12-month period
|
| Chiropractic Services |
Services do not require physician prescription and are limited to spinal subluxation
|
|
Tobacco Cessation
Program
|
Covered up to $100 for a 12- month period limit for a plan- approved program
Health Plan defines plan-approved program.
May be subject to formulary requirements.
|
|
[Value-added services]
|
See Attachment B-3
|
|
|
Inpatient and outpatient infertility treatments or reproductive services other than prenatal care, labor and delivery, and care related to disease, illnesses, or abnormalities related to the reproductive system
|
|
|
Personal comfort items including but not limited to personal care kits provided on inpatient admission, telephone, television, newborn infant photographs, meals for guests of patient, and other articles which are not required for the specific treatment of sickness or injury
|
|
|
Experimental and/or investigational medical, surgical or other health care procedures or services which are not generally employed or recognized within the medical community
|
|
|
Treatment or evaluations required by third parties including, but not limited to, those for schools, employment, flight clearance, camps, insurance or court
|
|
|
Private duty nursing services when performed on an inpatient basis or in a skilled nursing facility.
|
|
|
Mechanical organ replacement devices including, but not limited to artificial heart
|
|
|
Hospital services and supplies when confinement is solely for diagnostic testing purposes, unless otherwise pre-authorized by Health Plan
|
|
|
Prostate and mammography screening
|
|
|
Elective surgery to correct vision
|
|
|
Gastric procedures for weight loss
|
|
|
Cosmetic surgery/services solely for cosmetic purposes
Dental devices soley for cosmetic purposes
|
|
|
Out-of-network services not authorized by the Health Plan except for emergency care and physician services for a mother and her newborn(s) for a minimum of 48 hours following an uncomplicated vaginal delivery and 96 hours following an uncomplicated delivery by caesarian section
|
|
|
Services, supplies, meal replacements or supplements provided for weight control or the treatment of obesity, except for the services associated with the treatment for morbid obesity as part of a treatment plan approved by the Health Plan
|
|
|
Acupuncture services, naturopathy and hypnotherapy
|
|
|
Immunizations solely for foreign travel
|
|
|
Routine foot care such as hygienic care
|
|
|
Diagnosis and treatment of weak, strained, or flat feet and the cutting or removal of corns, calluses and toenails (this does not apply to the removal of nail roots or surgical treatment of conditions underlying corns, calluses or ingrown toenails)
|
|
|
Replacement or repair of prosthetic devices and durable medical equipment due to misuse, abuse or loss when confirmed by the Member or the vendor
|
|
|
Corrective orthopedic shoes
|
|
|
Convenience items
|
|
|
Orthotics primarily used for athletic or recreational purposes
|
|
|
Custodial care (care that assists a child with the activities of daily living, such as assistance in walking, getting in and out of bed, bathing, dressing, feeding, toileting, special diet preparation, and medication supervision that is usually self-administered or provided by a parent. This care does not require the continuing attention of trained medical or paramedical personnel.) This exclusion does not apply to hospice services.
|
|
|
Housekeeping
|
|
|
Public facility services and care for conditions that federal, state, or local law requires be provided in a public facility or care provided while in the custody of legal authorities
|
|
|
Services or supplies received from a nurse, which do not require the skill and training of a nurse
|
|
|
Vision training and vision therapy
|
|
|
Reimbursement for school-based physical therapy, occupational therapy, or speech therapy services are not covered except when ordered by a Physician/PCP
|
|
|
Donor non-medical expenses
|
|
|
Charges incurred as a donor of an organ when the recipient is not covered under this health plan
|
|
SUPPLIES
|
COVERED
|
EXCLUDED
|
COMMENTS/MEMBER
CONTRACT PROVISIONS
|
|
Ace Bandages
|
X
|
Exception: If provided by and billed through the clinic or home care agency it is covered as an incidental supply.
|
|
|
Alcohol, rubbing
|
X
|
Over-the-counter supply.
|
|
|
Alcohol, swabs (diabetic)
|
X
|
Over-the-counter supply not covered, unless RX provided at time of dispensing.
|
|
|
Alcohol, swabs
|
X
|
Covered only when received with IV therapy or central line kits/supplies.
|
|
|
Ana Kit Epinephrine
|
X
|
A self-injection kit used by patients highly allergic to bee stings.
|
|
|
Arm Sling
|
X
|
Dispensed as part of office visit.
|
|
|
Attends (Diapers)
|
X
|
Coverage limited to children age 4 or over only when prescribed by a physician and used to provide care for a covered diagnosis as outlined in a treatment care plan
|
|
|
Bandages
|
X
|
||
|
Basal Thermometer
|
X
|
Over-the-counter supply.
|
|
|
Batteries – initial
|
X
|
.
|
For covered DME items
|
|
Batteries – replacement
|
X
|
For covered DME when replacement is necessary due to normal use.
|
|
|
Betadine
|
X
|
See IV therapy supplies.
|
|
|
Books
|
X
|
||
|
Clinitest
|
X
|
For monitoring of diabetes.
|
|
|
Colostomy Bags
|
See Ostomy Supplies.
|
||
|
Communication Devices
|
X
|
||
|
Contraceptive Jelly
|
X
|
Over-the-counter supply. Contraceptives are not covered under the plan.
|
|
|
Cranial Head Mold
|
X
|
||
|
Diabetic Supplies
|
X
|
Monitor calibrating solution, insulin syringes, needles, lancets, lancet device, and glucose strips.
|
|
| Dental Devices | X | Coverage limited to dental devices used for treatment of craniofacial anomalies requiring surgical intervention. | |
|
Diapers/Incontinent Briefs/Chux
|
X
|
Coverage limited to children age 4 or over only when prescribed by a physician and used to provide care for a covered diagnosis as outlined in a treatment care plan
|
|
|
Diaphragm
|
X
|
Contraceptives are not covered under the plan.
|
|
|
Diastix
|
X
|
For monitoring diabetes.
|
|
|
Diet, Special
|
X
|
||
|
Distilled Water
|
X
|
||
|
Dressing Supplies/Central Line
|
X
|
Syringes, needles, Tegaderm, alcohol swabs, Betadine swabs or ointment, tape. Many times these items are dispensed in a kit when includes all necessary items for one dressing site change.
|
|
|
Dressing Supplies/Decubitus
|
X
|
Eligible for coverage only if receiving covered home care for wound care.
|
|
|
Dressing Supplies/Peripheral IV Therapy
|
X
|
Eligible for coverage only if receiving home IV therapy.
|
|
|
Dressing Supplies/Other
|
X
|
||
|
Dust Mask
|
X
|
||
|
Ear Molds
|
X
|
Custom made, post inner or middle ear surgery
|
|
|
Electrodes
|
X
|
Eligible for coverage when used with a covered DME.
|
|
|
Enema Supplies
|
X
|
Over-the-counter supply.
|
|
|
Enteral Nutrition
Supplies
|
X
|
Necessary supplies (e.g., bags, tubing, connectors, catheters, etc.) are
eligible for coverage. Enteral nutrition products are not covered except for those prescribed for hereditary metabolic disorders, a non-function or disease of the structures that normally permit food to reach the small bowel, or malabsorption due to disease
|
|
|
Eye Patches
|
X
|
Covered for patients with amblyopia.
|
|
|
Formula
|
X
|
Exception: Eligible for coverage only for chronic hereditary metabolic disorders a non-function or disease of the structures that normally permit food to reach the small bowel; or malabsorption due to disease (expected to last longer than 60 days when prescribed by the physician and authorized by plan.) Physician documentation to justify prescription of formula must include:
• Identification of a metabolic disorder, dysphagia that results in a medical need for a liquid diet, presence of a gastrostomy, or disease resulting in malabsorption that requires a medically necessary nutritional product
Does not include formula:
• For members who could be sustained on an age-appropriate diet.
• Traditionally used for infant feeding
• In pudding form (except for clients with documented oropharyngeal motor dysfunction who receive greater than 50 percent of their daily caloric intake from this product)
• For the primary diagnosis of failure to thrive, failure to gain weight, or lack of growth or for infants less than twelve months of age unless medical necessity is documented and other criteria, listed above, are met.
Food thickeners, baby food, or other regular grocery products that can be blenderized and used with an enteral system that are not medically necessary, are not covered, regardless of whether these regular food products are taken orally or parenterally.
|
|
|
Gloves
|
X
|
Exception: Central line dressings or wound care provided by home care agency.
|
|
|
Hydrogen Peroxide
|
X
|
Over-the-counter supply.
|
|
|
Hygiene Items
|
X
|
||
|
Incontinent Pads
|
X
|
Coverage limited to children age 4 or over only when prescribed by a physician and used to provide care for a covered diagnosis as outlined in a treatment care plan
|
|
|
Insulin Pump (External) Supplies
|
X
|
Supplies (e.g., infusion sets, syringe reservoir and dressing, etc.) are eligible for coverage if the pump is a covered item.
|
|
|
Irrigation Sets, Wound Care
|
X
|
Eligible for coverage when used during covered home care for wound care.
|
|
|
Irrigation Sets, Urinary
|
X
|
Eligible for coverage for individual with an indwelling urinary catheter.
|
|
|
IV Therapy Supplies
|
X
|
Tubing, filter, cassettes, IV pole, alcohol swabs, needles, syringes and any other related supplies necessary for home IV therapy.
|
|
|
K-Y Jelly
|
X
|
Over-the-counter supply.
|
|
|
Lancet Device
|
X
|
Limited to one device only.
|
|
|
Lancets
|
X
|
Eligible for individuals with diabetes.
|
|
|
Med Ejector
|
X
|
||
|
Needles and
Syringes/Diabetic
|
See Diabetic Supplies
|
||
|
Needles and Syringes/IV and Central Line
|
See IV Therapy and Dressing Supplies/Central Line.
|
||
|
Needles and Syringes/Other
|
X
|
Eligible for coverage if a covered IM or SubQ medication is being administered at home.
|
|
|
Normal Saline
|
See Saline, Normal
|
||
|
Novopen
|
X
|
||
|
Ostomy Supplies
|
X
|
Items eligible for coverage include: belt, pouch, bags, wafer, face plate, insert, barrier, filter, gasket, plug, irrigation kit/sleeve, tape, skin prep, adhesives, drain sets, adhesive remover, and pouch deodorant.
Items not eligible for coverage include: scissors, room deodorants, cleaners, rubber gloves, gauze, pouch covers, soaps, and lotions.
|
|
|
Parenteral Nutrition/Supplies
|
X
|
Necessary supplies (e.g., tubing, filters, connectors, etc.) are eligible for coverage when the Health Plan has authorized the parenteral nutrition.
|
|
|
Saline, Normal
|
X
|
Eligible for coverage:
a) when used to dilute medications for nebulizer treatments;
b) as part of covered home care for wound care;
c) for indwelling urinary catheter irrigation.
|
|
|
Stump Sleeve
|
X
|
||
|
Stump Socks
|
X
|
||
|
Suction Catheters
|
X
|
||
|
Syringes
|
See Needles/Syringes.
|
||
|
Tape
|
See Dressing Supplies, Ostomy Supplies, IV Therapy Supplies.
|
||
|
Tracheostomy Supplies
|
X
|
Cannulas, Tubes, Ties, Holders, Cleaning Kits, etc. are eligible for coverage.
|
|
|
Under Pads
|
See Diapers/Incontinent Briefs/Chux.
|
||
|
Unna Boot
|
X
|
Eligible for coverage when part of wound care in the home setting. Incidental charge when applied during office visit.
|
|
|
Urinary, External Catheter & Supplies
|
X
|
Exception: Covered when used by incontinent male where injury to the urethra prohibits use of an indwelling catheter ordered by the PCP and approved by the plan
|
|
|
Urinary, Indwelling Catheter & Supplies
|
X
|
Cover catheter, drainage bag with tubing, insertion tray, irrigation set and normal saline if needed.
|
|
|
Urinary, Intermittent
|
X
|
Cover supplies needed for intermittent or straight catherization.
|
|
|
Urine Test Kit
|
X
|
When determined to be medically necessary.
|
|
|
Urostomy supplies
|
See Ostomy Supplies.
|
|
DOCUMENT HISTORY LOG
|
||||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
|
Baseline
|
n/a
|
Initial version of Attachment B-2, Covered Services.
|
||
|
Revision
|
1.1
|
June 30, 2006
|
Revised Attachment B-2, Covered Services, by adding Attachment B-2.1, STAR+PLUS Covered Services. This is the initial version of Attachment B-2.1, STAR+PLUS Covered Services, which lists the Acute Care Services and the Community Based Long Term Care Services.
|
|
|
Revision
|
1.2
|
September 1, 2006
|
Contract Amendment did not revise Attachment B-2.1- STAR+PLUS Covered Services.
|
|
|
Revision
|
1.3
|
September 1, 2006
|
Contract Amendment did not revise Attachment B-2.1- STAR+PLUS Covered Services.
|
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract Amendment did not revise Attachment B-2.1- STAR+PLUS Covered Services.
|
|
|
Revision
|
1.5
|
January 1, 2007
|
Revised Attachment B-2.1, STAR+PLUS Covered Services, to include inpatient and outpatient mental health services for adults.
|
|
|
Revision
|
1.6
|
February 1, 2007
|
Revised Attachment B-2.1, STAR+PLUS Covered Services, to exclude inpatient mental health services for adults and children, and to establish monetary limits on Transition Assistance Services.
Personal Attendant Services is clarified to include the three service delivery options described in Attachment B-1, Section 8.3.5. Consumer Directed Personal Attendant Services is deleted from the list since it is one of the three service delivery options under Personal Attendant Services.
|
|
|
Revision
|
1.7
|
June 1, 2007
|
Revised Attachment B-2.1, STAR+PLUS Covered Services, to include inpatient mental health services for adults and children and to include effective dates by service area.
|
|
|
Revision
|
1.8
|
September 1, 2007
|
Contract Amendment did not revise Attachment B-2.1- STAR+PLUS Covered Services.
|
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract Amendment did not revise Attachment B-2.1- STAR+PLUS Covered Services.
|
|
| Revision | 1.10 | March 1, 2008 |
Contract Amendment did not revise Attachment B-2.1- STAR+PLUS Covered Services.
|
|
| Revision | 1.11 | September 1, 2008 | Attachment B-2.1 - STAR+PLUS Covered Services is modified to include additional covered services resulting from the Frew Settlement. | |
| Revision | 1.12 | March 1, 2009 | Attachment B-2.1- STAR+PLUS Covered Services is modified to exclude nursing home services. | |
| Revision | 1.13 | September 1, 2009 |
All references to “check-ups” are changed to “checkups”
Annual adult well check is removed from the list of enhanced benefits and added to “Services included under the HMO capitation payment”.
“Services included under the HMO capitation payment” is modified to remove “birthing center services” and add “Birthing services provided by a certified nurse midwife in a birthing center”.
“1915(c) NF Waiver Services” is modified to add “In-Home or Out-of-Home Respite Services”, to clarify that all covered services are medically necessary, and to clarify that that Medical Supplies not available under the Medicaid State Plan are covered.
|
|
| Revision | 1.14 | December 1, 2009 |
"Acute Care Services" is modified to clarify that the 30-day spell-of-illness limit is waived for inpatient behavioral health services.
Services included under the HMO capitation payment" is modified to remove references to PACT.
|
|
| Revision | 1.15 | March 1, 2010 |
“Services included under the HMO capitation payment” is modified to add substance abuse services. This amendment will be effective the later of: September 1, 2010 or upon final approval of the Medicaid State Plan, 1915(b) STAR+PLUS waiver and/or the 1915(b) STAR waiver, as applicable to the HMO Program.
|
|
| Revision | 1.16 | September 1, 2010 |
“Acute Care Services” is modified to add an enhanced benefit (waiver of 30 visit limit for outpatient mental health services).
“Services included under the HMO capitation payment” is modified to clarify the substance abuse services added by the last amendment; and to replace “certified nurse midwife” with “physician or Advanced Practice Nurse” and add the word “licensed” to Birthing Services. In addition, “mastectomy, breast reconstruction, and related follow-up procedures” and “Birthing services provided by a licensed birthing center” are added.
|
|
| Revision | 1.17 | December 1, 2010 |
Contract Amendment did not revise Attachment B-2.1- STAR+PLUS Covered Services.
|
|
| Revision | 1.18 | March 1, 2011 |
Services included under the HMO capitation payment is modified to remove the services effective prior to the effective dates of the State Plan and 1915(b) STAR Waiver.
Services included under the HMO capitation payment is modified to add "Cancer screening, diagnostic, and treatment services". These services are already 1905(a) covered services, therefore adding this reference does not impact the HMOs' rates.
|
|
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
||||
|
|
1. waiver of the three-prescription per month limit, for members not covered by Medicare; and
|
|
|
2. waiver of the 30-day spell-of-illness limit for inpatient behavioral health services.
|
|
|
• Ambulance services
|
|
|
• (These services are not subject to the quantitative treatment limitations that apply under traditional, fee-for-service Medicaid coverage. The services may be subject to the HMO's non-quantitative treatment limiations, provided such limitations comply with the requirments of the Mental Health Parity and Addiction Equity Act of 2008.) Behavioral Health Services, including:
|
|
|
o Inpatient mental health services for Adults and Children (Effective 6/01/07 in the Harris Service Area; and effective 9/01/07 in the Bexar, Nueces and Travis Service Areas.)
|
|
|
o Outpatient mental health services for Adults and Children
|
|
|
o Psychiatry services
|
|
|
o Counseling services for adults (21 years of age and over)
|
|
|
o Substance use disorder treatment services, including
|
|
|
o Outpatient services, including:
|
|
|
o Assessment
|
|
|
o Detoxification services
|
|
|
o Counseling treatment
|
|
|
o Medication assisted therapy
|
|
|
o Residential services, including
|
|
|
o Detoxification services
|
|
|
o Substance use disorder treatment (including room and board)
|
|
|
o Medication assisted therapy
|
|
|
• Birthing services provided by a physician or Advanced Practice Nurse in a licensed birthing center
|
|
|
• Birthing services provided by a licensed birthing center
|
|
|
• Cancer screening, diagnostic, and treatment services
|
|
|
• Chiropractic services
|
|
|
• Dialysis
|
|
|
• Durable medical equipment and supplies
|
|
|
• Emergency Services
|
|
|
• Family planning services
|
|
|
• Home health care services
|
|
|
• Hospital services, outpatient
|
|
|
• Laboratory
|
|
|
• Mastectomy, breast reconstruction, and related follow-up procedures, including:
|
|
|
o outpatient services provided at an outpatient hospital and ambulatory health care center as clinically appropriate; and physician and professional services provided in an office, inpatient, or outpatient setting for:
|
|
|
o all stages of reconstruction on the breast(s) on which medically necessary mastectomy procedure(s) have been performed;
|
|
|
o surgery and reconstruction on the other breast to produce symmetrical appearance;
|
|
|
o treatment of physical complications from the mastectomy and treatment of lymphedemas; and
|
|
|
o prophylactic mastectomy to prevent the development of breast cancer.
|
|
|
o external breast prosthesis for the breast(s) on which medically necessary mastectomy procedure(s) have been performed.
|
|
|
• Medical checkups and Comprehensive Care Program (CCP) Services for children (under age 21) through the Texas Health Steps Program
|
|
|
• Oral evaluation and fluoride varnish in the Medical Home in conjunction with Texas Health Steps medical checkup for children 6 months through 35 months of age.
|
|
|
• Optometry, glasses, and contact lenses, if medically necessary
|
|
|
• Podiatry
|
|
|
• Prenatal care
|
|
|
• Primary care services
|
|
|
• Preventive services including an annual adult well check for patients 21 years of age and over
|
|
|
• Radiology, imaging, and X-rays
|
|
|
• Specialty physician services
|
|
|
• Therapies – physical, occupational and speech
|
|
|
• Transplantation of organs and tissues
|
|
|
• Vision
|
|
|
o Personal Attendant Services – All Members of a STAR+PLUS HMO may receive medically and functionally necessary Personal Attendant Services (PAS).
|
|
|
o Day Activity and Health Services – All Members of a STAR+PLUS HMO may receive medically and functionally necessary Day Activity and Health Care Services (DAHS).
|
|
• 1915 (c) Nursing Facility Waiver Services for those Members who qualify for such services
|
|
|
o Personal Attendant Services (including the three service delivery options: Self-Directed; Agency Model, Self-Directed; and Agency Model)
o In-Home or Out-of-Home Respite Services
|
|
|
o Nursing Services (in home)
|
|
|
o Emergency Response Services (Emergency call button)
|
|
|
o Home Delivered Meals
|
|
|
o Minor Home Modifications
|
|
|
o Adaptive Aids and Medical Equipment
|
|
|
o Medical Supplies
|
|
|
o Physical Therapy, Occupational Therapy, Speech Therapy
|
|
|
o Adult Foster Care
|
|
|
o Assisted Living
|
| o Transition Assistance Services (These services are limited to a maximum of $2,500.00. If the HMO determines that no other resources are available to pay for the basic services/items needed to assist a Member, who is leaving a nursing facility, with setting up a household, the HMO may authorize up to $2,500.00 for Transition Assistance Services (TAS). The $2,500.00 TAS benefit is part of the expense ceiling when determining the Total Annual Individual Service Plan (ISP) Cost.) |
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
n/a
|
Initial version of Attachment B-2, Covered Services
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Revised Attachment B-2, Covered Services, by adding Attachment B-2.1, STAR+PLUS Covered Services.
|
|
Revision
|
1.2
|
September 1, 2006
|
Revised Attachment B-2, Covered Services, by updating provisions applicable to MCOs participating in the STAR and CHIP Programs.
|
|
Revision
|
1.3
|
September 1, 2006
|
Revised Attachment B-2, Covered Services, by adding Attachment B-2.2, CHIP Perinatal Covered Services. This is the initial version of Attachment B-2.2, which lists the CHIP Perinatal Covered Services, exclusions and DME/Supplies.
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
|
Revision
|
1.8
|
September 1, 2007
|
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
| Revision | 1.10 | March 1, 2008 |
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
| Revision | 1.11 | September 1, 2008 |
Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services.
|
| Revision | 1.12 | March 1, 2009 | Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services. |
| Revision | 1.13 | September 1, 2009 |
CHIP Perinatal Covered Services “Inpatient General Acute and Inpatient Rehabilitation Hospital Services” is modified to clarify the requirements regarding miscarriage and non-viable pregnancy.
CHIP Perinatal Covered Services “Outpatient Hospital, Comprehensive Outpatient Rehabilitation Hospital, Clinic (Including Health Center) and Ambulatory Health Care Center” is modified to clarify the requirements regarding miscarriage and non-viable pregnancy.
CHIP Perinatal Covered Services “Physician/Physician
Extender Professional Services” is modified to clarify the requirements regarding miscarriage and non-viable pregnancy.
CHIP Perinatal Covered Services “Emergency Services, including Emergency Hospitals, Physicians, and Ambulance Services” is modified to clarify the requirements regarding miscarriage and non-viable pregnancy.
“Outpatient Mental Health Services” is revised to provide additional clarity as it relates to Qualified Mental Health Providers – Community Services (QMHP-CS).
CHIP Perinatal Program Exclusions From Covered Services For CHIP Perinates is modified to clarify the requirements regarding miscarriage and non-viable pregnancy.
|
| Revision | 1.14 | December 1, 2009 | Outpatient Mental Health Services is revised to update the TAC citation. |
| Revision | 1.15 | March 1, 2010 | Contract Amendment did not revise Attachment B-2.2- CHIP Perinatal Covered Services. |
| Revision | 1.16 | September 1, 2010 |
Attachment B-2.2 is modified to clarify the 12-month enrollment period is for the CHIP Perinate Newborn beginning with the month of enrollment as a CHIP Perinate.
CHIP Perinatal Covered Services “Inpatient General Acute and Inpatient Rehabilitation Hospital Services” for Perinate Newborns is modified to remove the CHIP Perinate Newborn 0% to 185% category and to add outpatient services and orthodontic services to conform to CHIP Covered Services in Attachment B-2.
CHIP Perinatal Covered Services “Inpatient General Acute and Inpatient Rehabilitation Hospital Services” for Perinates is modified to remove the CHIP Perinate Newborn 0% to 185% category.
CHIP Perinatal Covered Services “Outpatient Hospital, Comprehensive Outpatient Rehabilitation Hospital, Clinic (Including Health Center) and Ambulatory Health Care Center” for Perinate Newborns is modified to add outpatient services and orthodontic services to conform to CHIP Covered Services in Attachment B-2.
CHIP Perinatal Covered Services “Physician/Physician Extender Professional Services” for Perinate Newborns is modified to add outpatient services and orthodontic services to conform to CHIP Covered Services in Attachment B-2.
CHIP Perinatal Covered Services “Durable Medical Equipment (DME), Prosthetic Devices and Disposable Medical Supplies” for Perinate Newborns is modified to add dental devices and external breast prostheses to conform to CHIP Covered Services in Attachment B-2.
The first bullet under “Exclusions from Covered Services for CHIP Perinates” is clarified.
The first bullet under “Exclusions from Covered Services for CHIP Perinate Newborns” is removed. “Dental Devices solely for cosmetic purposes” is added to conform to CHIP Covered Services in Attachment B-2.
“CHIP & CHIP Perinatal Program DME/Supplies” is modified to add “Dental Devices” to conform to CHIP Covered Services in Attachment B-2.
|
| Revision | 1.17 | December 1, 2010 | CHIP Hospice Care Services is modified to require concurrent CHIP and hospice care services to comply with the federal requirements from Section 2302 of the Patient Protection and Affordable Care Act of 2010 (P.L. 111-148). By law, CHIP health plans were required to provide concurrent hospice care services effective August 1, 2010. |
| Revision | 1.18 | March 1, 2010 |
Inpatient Mental Health Services for CHIP Perinate Newborns is modified to comply with the federal requirements of the Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA), as applied to CHIP by the Children’s Health Insurance Program Reauthorization Act of 2009 (P.L. 111-3). Also modified to clarify the court-ordered service requirement.
Outpatient Mental Health Services for CHIP Perinate Newborns is modified to comply with the federal requirements of the Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA) as applied to CHIP by the Children’s Health Insurance Program Reauthorization Act of 2009 (P.L. 111-3). Also modified to clarify the court-ordered service requirement.
Inpatient Substance Abuse Treatment Services for CHIP Perinate Newborns is modified to comply with the federal requirements of the Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA) as applied to CHIP by the CHIP Reauthorization Act of 2009 (P.L. 111-3).
Outpatient Substance Abuse Treatment Services for CHIP Perinate Newborns is modified to comply with the federal requirements of the Mental Health Parity and Addiction Equity Act of 2008 (MHPAEA) as applied to CHIP by the CHIP Reauthorization Act of 2009 (P.L. 111-3).
CHIP Perinatal Program Exclusions from Covered Services for CHIP Perinates is modified to clarify that CHIP does not provide coverage for members traveling outside of the U.S. CHIP Perinatal Program Exclusions from Covered Services for CHIP Perinate Newborns is modified to clarify that CHIP does not provide coverage for members traveling outside of the U.S.
|
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
Covered
Benefit
|
CHIP Perinate Newborn
|
CHIP Perinate
|
|
Inpatient General Acute and Inpatient Rehabilitation Hospital Services
|
Services include, but are not limited to, the following:
Hospital-provided Physician or Provider services
Semi-private room and board (or private if medically necessary as certified by attending)
General nursing care
Special duty nursing when medically necessary
ICU and services
Patient meals and special diets
Operating, recovery and other treatment rooms
Anesthesia and administration (facility technical component)
Surgical dressings, trays, casts, splints
Drugs, medications and biologicals
Blood or blood products that are not provided free-of-charge to the patient and their administration
X-rays, imaging and other radiological tests (facility technical component)
Laboratory and pathology services (facility technical component)
Machine diagnostic tests (EEGs, EKGs, etc.)
Oxygen services and inhalation therapy
Radiation and chemotherapy
Access to DSHS-designated Level III perinatal centers or Hospitals meeting equivalentlevels of care
In-network or out-of-network facility and Physician services for a mother and her newborn(s) for a minimum of 48 hours following an uncomplicated vaginal delivery and 96 hours following an uncomplicated delivery by caesarian section.
Hospital, physician and related medical services, such as anesthesia, associated with dental care
Surgical implants
Other artificial aids including surgical implants
Inpatient services for a mastectomy and breast reconstruction include:
all stages of reconstruction on the affected breast;
surgery and reconstruction on the other breast to produce symmetrical appearance; and
treatment of physical complications from the mastectomy and treatment of lymphedemas.
Implantable devices are covered under Inpatient and Outpatient services and do not count towards the DME 12-month period limit.
Pre-surgical or post-surgical orthodontic services for medically necessary treatment of craniofacial anomalies requiring surgical intervention and delivered as part of a proposed and clearly outlined treatment plan to treat:
cleft lip and/or palate; or
severe traumatic skeletal and/or congenital craniofacial deviations; or
severe facial asymmetry secondary to skeletal defects, congenital syndromal conditions and/or tumor growth or its treatment.
|
For CHIP Perinates in families with incomes at or below 185% of the Federal Poverty Level, the facility charges are not a covered benefit; however, professional services charges associated with labor with delivery are a covered benefit.
For CHIP Perinates in families with incomes between 185% and 200% of the Federal Poverty Level, benefits are limited to professional service charges and facility charges associated with labor with delivery until birth, and services related tomiscarriage or a non-viable pregnancy.
Services include:
Operating, recovery and other treatment rooms
Anesthesia and administration (facility technical component
Medically necessary surgical services are limited to services that directly relate to the delivery of the unborn child, and services related to miscarriage or non-viable pregnancy (molar pregnancy, ectopic pregnancy, or a fetus that expired in utero).
Inpatient services associated with (a) miscarriage or (b) a non-viable pregnancy (molar pregnancy, ectopic pregnancy, or a fetus that expired in utero) are a covered benefit. Inpatient services associated with miscarriage or non-viable pregnancy include, but are not limited to:
dilation and curettage (D&C) procedures;
appropriate provider-administered medications;
ultrasounds, and
histological examination of tissue samples
|
|
Skilled Nursing
Facilities
(Includes Rehabilitation
Hospitals)
|
Services include, but are not limited to, the following:
Semi-private room and board
Regular nursing services
Rehabilitation services
Medical supplies and use of appliances and equipment furnished by the facility
|
Not a covered benefit.
|
|
Outpatient Hospital, Comprehensive Outpatient Rehabilitation Hospital, Clinic (Including Health Center) and Ambulatory Health Care Center
|
Services include, but are not limited to, the following services provided in a hospital clinic or emergency room, a clinic or health center, hospital-based emergency department or an ambulatory health care setting:
X-ray, imaging, and radiological tests (technical component)
Laboratory and pathology services (technical component)
Machine diagnostic tests
Ambulatory surgical facility services
Drugs, medications and biologicals
Casts, splints, dressings
Preventive health services
Physical, occupational and speech therapy
Renal dialysis
Respiratory services
Radiation and chemotherapy
Blood or blood products that are not provided free-of-charge to the patient and the administration of these products
Facility and related medical services, such as anesthesia, associated with dental care, when provided in a licensed ambulatory surgical facility.
Surgical implants
Other artificial aids including surgical implants
Outpatient services provided at an outpatient hosptial or ambulatory health care center for a mastectomy and breast reconstruction as clinically appropriate, include:
- all stages of reconstruction on the affected breast;
- surgery and reconstruction on the other breast to produces symmetrical appearance; and
- treatment of physical complications from the mastectomy and treatment of lymphedemas.
Implantable devices are covered under Inpatient and Outpatient services and do not count towards the DME 12-month period limit.
Pre-surgical or post-surgical orthodontic services for medically necessary treatment of craniofacial anomalies requiring surgical intervention and delivered as part of a proposed and clearly outlined treatment plan to treat:
cleft lip and/or palate; or
severe traumatic skeletal and/or congenital craniofacial deviations; or
severe facial asymmetry secondary to skeletal defects, congenital syndromal conditions and/or tumor growth or its treatment.
|
Services include, the following services provided in a hospital clinic or emergency room, a clinic or health center, hospital-based emergency department or an ambulatory health care setting:
X-ray, imaging, and radiological tests (technical component)
Laboratory and pathology services (technical component)
Machine diagnostic tests
Drugs, medications and biologicals that are medically necessary prescription and injection drugs.
Outpatient services associated with (a) miscarriage or (b) a non-viable pregnancy (molar pregnancy, ectopic pregnancy, or a fetus that expired in utero) are a covered benefit. Inpatient services associated with miscarriage or non-viable pregnancy include, but are not limited to:
dilation and curettage (D&C) procedures;
appropriate provider-administered medications;
ultrasounds, and
histological examination of tissue samples
(1) Laboratory and radiological services are limited to services that directly relate to ante partum care and/or the delivery of the covered CHIP Perinate until birth.
(2) Ultrasound of the pregnant uterus is a covered benefit when medically indicated. Ultrasound may be indicated for suspected genetic defects, high-risk pregnancy, fetal growth retardation, or gestational age confirmation or miscarriage or non-viable pregnancy.
(3) Amniocentesis, Cordocentesis, Fetal Intrauterine Transfusion (FIUT) and Ultrasonic Guidance for Cordocentesis, FIUT are covered benefits with an appropriate diagnosis.
(4) Laboratory tests are limited to: nonstress testing, contraction, stress testing, hemoglobin or hematocrit repeated once a trimester and at 32-36 weeks of pregnancy; or complete blood count (CBC), urinanalysis for protein and glucose every visit, blood type and RH antibody screen; repeat antibody screen for Rh negative women at 28 weeks followed by RHO immune globulin
administration if indicated; rubella antibody titer, serology for syphilis, hepatitis B surface antigen, cervical cytology, pregnancy test, gonorrhea test, urine culture, sickle cell test, tuberculosis (TB) test, human immunodeficiency virus (HIV) antibody screen, Chlamydia test, other laboratory tests not specified but deemed medically necessary, and multiple marker screens for neural tube defects (if the client initiates care between 16 and 20 weeks); screen for gestational diabetes at 24-28 weeks of pregnancy; other lab tests as indicated by medical condition of client.
|
|
Physician/
Physician
Extender Professional Services
|
Services include, but are not limited to, the following:
American Academy of Pediatrics recommended well-child exams and preventive health services (including, but not limited to, vision and hearing screening and immunizations)
Physician office visits, in-patient and out-patient services
Laboratory, x-rays, imaging and pathology services, including technical component and/or professional interpretation
Medications, biologicals and materials administered in Physician’s office
Allergy testing, serum and injections
Professional component (in/outpatient) of surgical services, including:
- Surgeons and assistant surgeons for surgical procedures including appropriate follow-up care
- Administration of anesthesia by Physician (other than surgeon) or CRNA
- Second surgical opinions
- Same-day surgery performed in a Hospital without an over-night stay
- Invasive diagnostic procedures such as endoscopic examinations
Hospital-based Physician services (including Physician-performed technical and interpretive components)
Physician and professional services for mastectomy and breast reconstruction include:
- all stages of reconstruction on the affected breast;
- surgery and reconstruction on the other breast to produces symmetrical appearance; and
- treatment of physical complications from the mastectomy and treatment of lymphedemas.
In-network and out-of-network Physician services for a mother and her newborn(s) for a minimum of 48 hours following an uncomplicated vaginal delivery and 96 hours following an uncomplicated delivery by caesarian section.
Physician services medically necessary to support a dentist providing dental services to a CHIP member such as general anesthesia or intravenous (IV) sedation.
Pre-surgical or post-surgical orthodontic services for medically necessary treatment of craniofacial anomalies requiring surgical intervention and delivered as part of a proposed and clearly outlined treatment plan to treat:
cleft lip and/or palate; or
severe traumatic skeletal and/or congenital craniofacial deviations; or
severe facial asymmetry secondary to skeletal defects, congenital syndromal conditions and/or tumor growth or its treatment.
|
Services include, but are not limited to the following:
Medically necessary physician services are limited to prenatal and postpartum care and/or the delivery of the covered unborn child until birth
Physician office visits, in-patient and out-patient services
Laboratory, x-rays, imaging and pathology services including technical component and /or professional interpretation
Medically necessary medications, biologicals and materials administered in Physician’s office
Professional component (in/outpatient) of surgical services, including:
o Surgeons and assistant surgeons for surgical procedures directly related to the labor with delivery of the covered unborn child until birth.
o Administration of anesthesia by Physician (other than surgeon) or CRNA
o Invasive diagnostic procedures directly related to the labor with delivery of the unborn child.
Hospital-based Physician services (including Physician performed technical and interpretive components)
Professional component of the ultrasound of the pregnant uterus when medically indicated for suspected genetic defects, high-risk pregnancy, fetal growth retardation, or gestational age confirmation.
Professional component of Amniocentesis, Cordocentesis, Fetal Intrauterine Transfusion (FIUT) and Ultrasonic Guidance for Amniocentesis, Cordocentrsis, and FIUT.
Professional component associated with (a) miscarriage or (b) a non-viable pregnancy (molar pregnancy, ectopic pregnancy, or a fetus that expired in utero) are a covered benefit. Inpatient services associated with miscarriage or non-viable pregnancy include, but are not limited to:
dilation and curettage (D&C) procedures;
appropriate provider-administered medications;
ultrasounds, and
histological examination of tissue samples
|
|
Prenatal Care and Pre-Pregnancy Family Services and Supplies
|
Not a covered benefit.
|
Services are limited to an initial visit and subsequent prenatal (ante partum) care visits that include:
(1) One visit every four weeks for the first 28 weeks or pregnancy;
(2) one visit every two to three weeks from 28 to 36 weeks of pregnancy; and
(3) one visit per week from 36 weeks to delivery.
More frequent visits are allowed as Medically Necessary. Benefits are limited to:
Limit of 20 prenatal visits and 2 postpartum visits (maximum within 60 days) without documentation of a complication of pregnancy. More frequent visits may be necessary for high-risk pregnancies. High-risk prenatal visits are not limited to 20 visits per pregnancy. Documentation supporting medical necessity must be maintained in the physician’s files and is subject to retrospective review.
Visits after the initial visit must include:
interim history (problems, marital status, fetal status);
physical examination (weight, blood pressure, fundalheight, fetal position and size, fetal heart rate, extremities) and
laboratory tests (urinanalysis for protein and glucose every visit; hematocrit or hemoglobin repeated once a trimester and at 32-36 weeks of pregnancy; multiple marker screen for fetal abnormalities offered at 16-20 weeks of pregnancy; repeat antibody screen for Rh negative women at 28 weeks followed by Rho immune globulin administration if indicated; screen for gestational diabetes at 24-28 weeks of pregnancy; and other lab tests as indicated by medical condition of client).
|
|
Durable Medical Equipment (DME), Prosthetic Devices and
Disposable Medical Supplies
|
$20,000 12-month period limit for DME, prosthetics, devices and disposable medical supplies (diabetic supplies and equipment are not counted against this cap). Services include DME (equipment which can withstand repeated use and is primarily and customarily used to serve a medical purpose, generally is not useful to a person in the absence of Illness, Injury, or Disability, and is appropriate for use in the home), including devices and supplies that are medically necessary and necessary for one or more activities of daily living and appropriate to assist in the treatment of a medical condition, including:
Orthotic braces and orthotics
Dental devices
Prosthetic devices such as artificial eyes, limbs, braces and external breast prostheses
Prosthetic eyeglasses and contact lenses for the management of severe ophthalmologic disease
Hearing aids
Diagnosis-specific disposable medical supplies, including diagnosis-specific prescribed specialty formula and dietary supplements. (See Attachment A)
|
Not a covered benefit.
|
|
Home and Community Health Services
|
Services that are provided in the home and community, including, but not limited to:
Home infusion
Respiratory therapy
Visits for private duty nursing (R.N., L.V.N.)
Skilled nursing visits as defined for home health purposes (may include R.N. or L.V.N.).
Home health aide when included as part of a plan of care during a period that skilled visits have been approved.
Speech, physical and occupational therapies.
Services are not intended to replace the CHILD'S caretaker or to provide relief for the caretaker
Skilled nursing visits are provided on intermittent level and not intended to provide 24-hour skilled nursing services
Services are not intended to replace 24-hour inpatient or skilled nursing facility services
|
Not a covered benefit.
|
|
Inpatient Mental Health Services
|
Mental health services, including for serious mental illness, furnished in a free-standing psychiatric hospital, psychiatric units of general acute care hospitals and state-operated facilities, including, but not limited to:
Neuropsychological and psychological testing.
When inpatient psychiatric services are ordered by a court of competent jurisdiction under the provisions of Chapters 573 and 574 of the Texas Health and Safety Code, relating to court ordered commitments to psychiatric facilities, the court order serves as binding determination of medical necessity. Any modification or termination of services must be presented to the court with jurisdiction over the matter for determination
Does not require PCP referral |
Not a covered benefit.
|
|
Outpatient Mental Health Services
|
Mental health services, including for serious mental illness, provided on an outpatient basis, including, but not limited to:
Medication management visits do not count against the outpatient visit limit.
The visits can be furnished in a variety of community-based settings (including school and home-based) or in a state-operated facility
Neuropsychological and psychological testing
Medication management
Rehabilitative day treatments
Residential treatment services
Sub-acute outpatient services (partial hospitalization or rehabilitative day treatment)
Skills training (psycho-educational skill development)
When outpatient psychiatric services are ordered by a court of competent jurisdiction under the provisions of Chapters 573 and 574 of the Texas Health and Safety Code, relating to court ordered commitments to psychiatric facilities, the court order serves as binding determination of medical necessity. Any modification or termination of services must be presented to the court with jurisdiction over the matter for determination
A Qualified Mental Health Provider – Community Services (QMHP-CS), is defined by the Texas Department of State Health Services (DSHS) in Title 25 T.A.C., Part I, Chapter 412, Subchapter G, Division 1, §412.303(48). QMHP-CSs shall be providers working through a DSHS-contracted Local Mental Health Authority or a separate DSHS-contracted entity. QMHP-CSs shall be supervised by a licensed mental health professional or physician and provide services in accordance with DSHS standards. Those services include individual and group skills training (which can be components of interventions such as day treatment and in-home services), patient and does not require PCP referral |
|
Not a covered benefit.
|
||
|
Inpatient Substance Abuse Treatment Services
|
Services include, but are not limited to:
Inpatient and residential substance abuse treatment services including detoxification and crisis stabilization, and 24-hour residential rehabilitation programs
Does not require PCP referral
|
Not a covered benefit.
|
|
Outpatient Substance Abuse Treatment Services
|
Services include, but are not limited to, the following:
Prevention and intervention services that are provided by physician and non-physician providers, such as screening, assessment and referral for chemical dependency disorders.
Intensive outpatient services
Partial hospitalization
Intensive outpatient services is defined as an organized non-residential service providing structured group and individual therapy, educational services, and life skills training which consists of at least 10 hours per week for four to 12 weeks, but less than 24 hours per day
Outpatient treatment service is defined as consisting of at least one to two hours per week providing structured group and individual therapy, educational services, and life skills training
Does not require PCP referral
|
Not a covered benefit.
|
|
Rehabilitation Services
|
Services include, but are not limited to, the following:
Habilitation (the process of supplying a child with the means to reach age-appropriate developmental milestones through therapy or treatment) and rehabilitation services include, but are not limited to the following:
Physical, occupational and speech therapy
Developmental assessment
|
Not a covered benefit.
|
|
Hospice Care Services
|
Services include, but are not limited to:
Palliative care, including medical and support services, for those children who have six months or less to live, to keep patients comfortable during the last weeks and months before death
Treatment services, including treatment related to the terminal illness
Up to a maximum of 120 days with a 6 month life expectancy
Patients electing hospice services may cancel this election at anytime
Services apply to the hospice diagnosis
|
Not a covered benefit.
|
|
Emergency Services, including Emergency Hospitals, Physicians, and Ambulance Services
|
HMO cannot require authorization as a condition for payment for emergency conditions labor and
delivery.
Covered services include, but are not limited to, the following:
Emergency services based on prudent lay person definition of emergency health condition
Hospital emergency department room and ancillary services and physician services 24 hours a day, 7 days a week, both by in-network and out-of-network providers
Medical screening examination
Stabilization services
Access to DSHS designated Level 1 and Level II trauma centers or hospitals meeting equivalent levels of care for emergency services
Emergency ground, air and water transportation
Emergency dental services, limited to fractured or dislocated jaw, traumatic damage to teeth, and removal of cysts.
|
HMO cannot require authorization as a condition for payment for emergency conditions related to labor with delivery.
Covered services are limited to those emergency services that are directly related to the delivery of the unborn child until birth.
Emergency services based on prudent lay person definition of emergency health condition
Medical screening examination to determine emergency when directly related to the delivery of the covered unborn child.
Stabilization services related to the labor with delivery of the covered unborn child.
Emergency ground, air and water transportation for labor and threatened labor is a covered benefit
Benefit limits: Post-delivery services or complications resulting in the need for emergency services for the mother of the CHIP Perinate are not a covered benefit.
|
|
Transplants
|
Services include, but are not limited to, the following:
Using up-to-date FDA guidelines, all non-experimental human organ and tissue transplants and all forms of non-experimental corneal, bone marrow and peripheral stem cell transplants, including donor medical expenses.
|
Not a covered benefit.
|
|
Vision Benefit
|
The health plan may reasonably limit the cost of the frames/lenses.
Services include:
One examination of the eyes to determine the need for and prescription for corrective lenses per 12-month period, without authorization
One pair of non-prosthetic eyewear per 12-month period
|
Not a covered benefit.
|
|
Chiropractic Services
|
Services do not require physician prescription and are limited to spinal subluxation.
|
Not a covered benefit.
|
|
Tobacco Cessation
Program
|
Covered up to $100 for a 12- month period limit for a plan- approved program
Health Plan defines plan-approved program.
May be subject to formulary requirements.
|
Not a covered benefit.
|
|
Case Management and Care Coordination Services
|
These services include outreach informing, case management, care coordination and community referral.
|
Covered benefit.
|
|
Value-added services
|
See Attachment B-3.2
|
|
|
For CHIP Perinates in families with incomes at or below 185% of the Federal Poverty Level, inpatient facility charges are not a covered benefit if associated with the initial Perinatal Newborn admission. "Initial Perinatal Newborn admission" means the hospitalization associated with the birth.
|
|
|
Inpatient and outpatient treatments other than prenatal care, labor with delivery, and postpartum care related to (a) miscarriage and (b) a non-viable pregnancy, and postpartum care related to the covered unborn child until birth.
|
|
|
Inpatient mental health services.
|
|
|
Outpatient mental health services.
|
|
|
Durable medical equipment or other medically related remedial devices.
|
|
|
Disposable medical supplies.
|
|
|
Home and community-based health care services.
|
|
|
Nursing care services.
|
|
|
Dental services.
|
|
|
Inpatient substance abuse treatment services and residential substance abuse treatment services.
|
|
|
Outpatient substance abuse treatment services.
|
|
|
Physical therapy, occupational therapy, and services for individuals with speech, hearing, and language disorders.
|
|
|
Hospice care.
|
|
|
Skilled nursing facility and rehabilitation hospital services.
|
|
|
Emergency services other than those directly related to the labor with delivery of the covered unborn child.
|
|
|
Transplant services.
|
|
|
Tobacco Cessation Programs.
|
|
|
Chiropractic Services.
|
|
|
Medical transportation not directly related to the labor or threatened labor and/or delivery of the covered unborn child.
|
|
|
Personal comfort items including but not limited to personal care kits provided on inpatient admission, telephone, television, newborn infant photographs, meals for guests of patient, and other articles which are not required for the specific treatment related to labor with delivery or post partum care.
|
|
|
Experimental and/or investigational medical, surgical or other health care procedures or services which are not generally employed or recognized within the medical community
|
|
|
Treatment or evaluations required by third parties including, but not limited to, those for schools, employment, flight clearance, camps, insurance or court
|
|
|
Private duty nursing services when performed on an inpatient basis or in a skilled nursing facility.
|
|
|
Coverage while traveling outside of the United States and U.S. Terriotries (including Puerto Rico, U.S. Virgin Islands, Commonwealth of Northern Mariana Islands, Guam, and American Samoa).
|
|
|
Mechanical organ replacement devices including, but not limited to artificial heart
|
|
|
Hospital services and supplies when confinement is solely for diagnostic testing purposes and not a part of labor with delivery
|
|
|
Prostate and mammography screening
|
|
|
Elective surgery to correct vision
|
|
|
Gastric procedures for weight loss
|
|
|
Cosmetic surgery/services solely for cosmetic purposes
|
|
|
Out-of-network services not authorized by the Health Plan except for emergency care related to the labor with delivery of the covered unborn child.
|
|
|
Services, supplies, meal replacements or supplements provided for weight control or the treatment of obesity
|
|
|
Acupuncture services, naturopathy and hypnotherapy
|
|
|
Immunizations solely for foreign travel
|
|
|
Routine foot care such as hygienic care
|
|
|
Diagnosis and treatment of weak, strained, or flat feet and the cutting or removal of corns, calluses and toenails (this does not apply to the removal of nail roots or surgical treatment of conditions underlying corns, calluses or ingrown toenails)
|
|
|
Corrective orthopedic shoes
|
|
|
Convenience items
|
|
|
Orthotics primarily used for athletic or recreational purposes
|
|
|
Custodial care (care that assists with the activities of daily living, such as assistance in walking, getting in and out of bed, bathing, dressing, feeding, toileting, special diet preparation, and medication supervision that is usually self-administered or provided by a caregiver. This care does not require the continuing attention of trained medical or paramedical personnel.)
|
|
|
Housekeeping
|
|
|
Public facility services and care for conditions that federal, state, or local law requires be provided in a public facility or care provided while in the custody of legal authorities
|
|
|
Services or supplies received from a nurse, which do not require the skill and training of a nurse
|
|
|
Vision training, vision therapy, or vision services
|
|
|
Reimbursement for school-based physical therapy, occupational therapy, or speech therapy services are not covered
|
|
|
Donor non-medical expenses
|
|
|
Charges incurred as a donor of an organ
|
|
|
Inpatient and outpatient infertility treatments or reproductive services other than prenatal care, labor and delivery, and care related to disease, illnesses, or abnormalities related to the reproductive system
|
|
|
Personal comfort items including but not limited to personal care kits provided on inpatient admission, telephone, television, newborn infant photographs, meals for guests of patient, and other articles which are not required for the specific treatment of sickness or injury
|
|
|
Experimental and/or investigational medical, surgical or other health care procedures or services which are not generally employed or recognized within the medical community
|
|
|
Treatment or evaluations required by third parties including, but not limited to, those for schools, employment, flight clearance, camps, insurance or court
|
|
|
Private duty nursing services when performed on an inpatient basis or in a skilled nursing facility.
|
|
|
Coverage while traveling outside of the United States and U.S. Terriotries (including Puerto Rico, U.S. Virgin Islands, Commonwealth of Northern Mariana Islands, Guam, and American Samoa).
|
|
|
Mechanical organ replacement devices including, but not limited to artificial heart
|
|
|
Hospital services and supplies when confinement is solely for diagnostic testing purposes, unless otherwise pre-authorized by Health Plan
|
|
|
Prostate and mammography screening
|
|
|
Elective surgery to correct vision
|
|
|
Gastric procedures for weight loss
|
|
|
Cosmetic surgery/services solely for cosmetic purposes
|
|
|
Dental Devices solely for cosmetic purposes
Out-of-network services not authorized by the Health Plan except for emergency care and physician services for a mother and her newborn(s) for a minimum of 48 hours following an uncomplicated vaginal delivery and 96 hours following an uncomplicated delivery by caesarian section
|
|
|
Services, supplies, meal replacements or supplements provided for weight control or the treatment of obesity, except for the services associated with the treatment for morbid obesity as part of a treatment plan approved by the Health Plan
|
|
|
Acupuncture services, naturopathy and hypnotherapy
|
|
|
Immunizations solely for foreign travel
|
|
|
Routine foot care such as hygienic care
|
|
|
Diagnosis and treatment of weak, strained, or flat feet and the cutting or removal of corns, calluses and toenails (this does not apply to the removal of nail roots or surgical treatment of conditions underlying corns, calluses or ingrown toenails)
|
|
|
Replacement or repair of prosthetic devices and durable medical equipment due to misuse, abuse or loss when confirmed by the Member or the vendor
|
|
|
Corrective orthopedic shoes
|
|
|
Convenience items
|
|
|
Orthotics primarily used for athletic or recreational purposes
|
|
|
Custodial care (care that assists a child with the activities of daily living, such as assistance in walking, getting in and out of bed, bathing, dressing, feeding, toileting, special diet preparation, and medication supervision that is usually self-administered or provided by a parent. This care does not require the continuing attention of trained medical or paramedical personnel.) This exclusion does not apply to hospice services.
|
|
|
Housekeeping
|
|
|
Public facility services and care for conditions that federal, state, or local law requires be provided in a public facility or care provided while in the custody of legal authorities
|
|
|
Services or supplies received from a nurse, which do not require the skill and training of a nurse
|
|
|
Vision training and vision therapy
|
|
|
Reimbursement for school-based physical therapy, occupational therapy, or speech therapy services are not covered except when ordered by a Physician/PCP
|
|
|
Donor non-medical expenses
|
|
|
Charges incurred as a donor of an organ when the recipient is not covered under this health plan
|
|
SUPPLIES
|
COVERED
|
EXCLUDED
|
COMMENTS/MEMBER
CONTRACT PROVISIONS
|
|
Ace Bandages
|
X
|
Exception: If provided by and billed through the clinic or home care agency it is covered as an incidental supply.
|
|
|
Alcohol, rubbing
|
X
|
Over-the-counter supply.
|
|
|
Alcohol, swabs (diabetic)
|
X
|
Over-the-counter supply not covered, unless RX provided at time of dispensing.
|
|
|
Alcohol, swabs
|
X
|
Covered only when received with IV therapy or central line kits/supplies.
|
|
|
Ana Kit Epinephrine
|
X
|
A self-injection kit used by patients highly allergic to bee stings.
|
|
|
Arm Sling
|
X
|
Dispensed as part of office visit.
|
|
|
Attends (Diapers)
|
X
|
Coverage limited to children age 4 or over only when prescribed by a physician and used to provide care for a covered diagnosis as outlined in a treatment care plan.
|
|
|
Bandages
|
X
|
||
|
Basal Thermometer
|
X
|
Over-the-counter supply.
|
|
|
Batteries – initial
|
X
|
.
|
For covered DME items
|
|
Batteries – replacement
|
X
|
For covered DME when replacement is necessary due to normal use.
|
|
|
Betadine
|
X
|
See IV therapy supplies.
|
|
|
Books
|
X
|
||
|
Clinitest
|
X
|
For monitoring of diabetes.
|
|
|
Colostomy Bags
|
See Ostomy Supplies.
|
||
|
Communication Devices
|
X
|
||
|
Contraceptive Jelly
|
X
|
Over-the-counter supply. Contraceptives are not covered under the plan.
|
|
|
Cranial Head Mold
|
X
|
||
| Dental Devices | X | Coverage limited to dental devices used for treatment of craniofacial anomalies requiring surgical intervention. | |
|
Diabetic Supplies
|
X
|
Monitor calibrating solution, insulin syringes, needles, lancets, lancet device, and glucose strips.
|
|
|
Diapers/Incontinent Briefs/Chux
|
X
|
Coverage limited to children age 4 or over only when prescribed by a physician and used to provide care for a covered diagnosis as outlined in a treatment care plan
|
|
|
Diaphragm
|
X
|
Contraceptives are not covered under the plan.
|
|
|
Diastix
|
X
|
For monitoring diabetes.
|
|
|
Diet, Special
|
X
|
||
|
Distilled Water
|
X
|
||
|
Dressing Supplies/Central Line
|
X
|
Syringes, needles, Tegaderm, alcohol swabs, Betadine swabs or ointment, tape. Many times these items are dispensed in a kit when includes all necessary items for one dressing site change.
|
|
|
Dressing Supplies/Decubitus
|
X
|
Eligible for coverage only if receiving covered home care for wound care.
|
|
|
Dressing Supplies/Peripheral IV Therapy
|
X
|
Eligible for coverage only if receiving home IV therapy.
|
|
|
Dressing Supplies/Other
|
X
|
||
|
Dust Mask
|
X
|
||
|
Ear Molds
|
X
|
Custom made, post inner or middle ear surgery
|
|
|
Electrodes
|
X
|
Eligible for coverage when used with a covered DME.
|
|
|
Enema Supplies
|
X
|
Over-the-counter supply.
|
|
|
Enteral Nutrition Supplies
|
X
|
Necessary supplies (e.g., bags, tubing, connectors, catheters, etc.) are eligible for coverage. Enteral nutrition products are not covered except for those prescribed for hereditary metabolic disorders, a non-function or disease of the structures that normally permit food to reach the small bowel, or malabsorption due to disease
|
|
|
Eye Patches
|
X
|
Covered for patients with amblyopia.
|
|
|
Formula
|
X
|
Exception: Eligible for coverage only for chronic hereditary metabolic disorders a non-function or disease of the structures that normally permit food to reach the small bowel; or malabsorption due to disease (expected to last longer than 60 days when prescribed by the physician and authorized by plan.) Physician documentation to justify prescription of formula must include:
• Identification of a metabolic disorder, dysphagia that results in a medical need for a liquid diet, presence of a gastrostomy, or disease resulting in malabsorption that requires a medically necessary nutritional product
Does not include formula:
• For members who could be sustained on an age-appropriate diet.
• Traditionally used for infant feeding
• In pudding form (except for clients with documented oropharyngeal motor dysfunction who receive greater than 50 percent of their daily caloric intake from this product)
• For the primary diagnosis of failure to thrive, failure to gain weight, or lack of growth or for infants less than twelve months of age unless medical necessity is documented and other criteria, listed above, are met.
Food thickeners, baby food, or other regular grocery products that can be blenderized and used with an enteral system that are not medically necessary, are not covered, regardless of whether these regular food products are taken orally or parenterally.
|
|
|
Gloves
|
X
|
Exception: Central line dressings or wound care provided by home care agency.
|
|
|
Hydrogen Peroxide
|
X
|
Over-the-counter supply.
|
|
|
Hygiene Items
|
X
|
||
|
Incontinent Pads
|
X
|
Coverage limited to children age 4 or over only when prescribed by a physician and used to provide care for a covered diagnosis as outlined in a treatment care plan
|
|
|
Insulin Pump (External) Supplies
|
X
|
Supplies (e.g., infusion sets, syringe reservoir and dressing, etc.) are eligible for coverage if the pump is a covered item.
|
|
|
Irrigation Sets, Wound Care
|
X
|
Eligible for coverage when used during covered home care for wound care.
|
|
|
Irrigation Sets, Urinary
|
X
|
Eligible for coverage for individual with an indwelling urinary catheter.
|
|
|
IV Therapy Supplies
|
X
|
Tubing, filter, cassettes, IV pole, alcohol swabs, needles, syringes and any other related supplies necessary for home IV therapy.
|
|
|
K-Y Jelly
|
X
|
Over-the-counter supply.
|
|
|
Lancet Device
|
X
|
Limited to one device only.
|
|
|
Lancets
|
X
|
Eligible for individuals with diabetes.
|
|
|
Med Ejector
|
X
|
||
|
Needles and Syringes/Diabetic
|
See Diabetic Supplies
|
||
|
Needles and Syringes/IV and Central Line
|
See IV Therapy and Dressing Supplies/Central Line.
|
||
|
Needles and Syringes/Other
|
X
|
Eligible for coverage if a covered IM or SubQ medication is being administered at home.
|
|
|
Normal Saline
|
See Saline, Normal
|
||
|
Novopen
|
X
|
||
|
Ostomy Supplies
|
X
|
Items eligible for coverage include: belt, pouch, bags, wafer, face plate, insert, barrier, filter, gasket, plug, irrigation kit/sleeve, tape, skin prep, adhesives, drain sets, adhesive remover, and pouch deodorant.
Items not eligible for coverage include: scissors, room deodorants, cleaners, rubber gloves, gauze, pouch covers, soaps, and lotions.
|
|
|
Parenteral Nutrition/Supplies
|
X
|
Necessary supplies (e.g., tubing, filters, connectors, etc.) are eligible for coverage when the Health Plan has authorized the parenteral nutrition.
|
|
|
Saline, Normal
|
X
|
Eligible for coverage:
a) when used to dilute medications for nebulizer treatments;
b) as part of covered home care for wound care;
c) for indwelling urinary catheter irrigation.
|
|
|
Stump Sleeve
|
X
|
||
|
Stump Socks
|
X
|
||
|
Suction Catheters
|
X
|
||
|
Syringes
|
See Needles/Syringes.
|
||
|
Tape
|
See Dressing Supplies, Ostomy Supplies, IV Therapy Supplies.
|
||
|
Tracheostomy Supplies
|
X
|
Cannulas, Tubes, Ties, Holders, Cleaning Kits, etc. are eligible for coverage.
|
|
|
Under Pads
|
See Diapers/Incontinent Briefs/Chux.
|
||
|
Unna Boot
|
X
|
Eligible for coverage when part of wound care in the home setting. Incidental charge when applied during office visit.
|
|
|
Urinary, External Catheter & Supplies
|
X
|
Exception: Covered when used by incontinent male where injury to the urethra prohibits use of an indwelling catheter ordered by the PCP and approved by the plan
|
|
|
Urinary, Indwelling Catheter & Supplies
|
X
|
Cover catheter, drainage bag with tubing, insertion tray, irrigation set and normal saline if needed.
|
|
|
Urinary, Intermittent
|
X
|
Cover supplies needed for intermittent or straight catherization.
|
|
|
Urine Test Kit
|
X
|
When determined to be medically necessary.
|
|
|
Urostomy supplies
|
See Ostomy Supplies.
|
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
n/a
|
Initial version of Attachment B-3, Value-added Services.
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.2
|
September 1, 2006
|
Revised the Physical Health Value-added Services to include Home Visits to New Mothers. Revised the certification provision by changing the start date for the 12-month provision of services.
|
|
Revision
|
1.3
|
September 1, 2006
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment removed the separate signature requirement for Attachment B-3, Value-added Services. By signing the Contract and/or Contract Amendment, the HMO certifies that it will provide the Value-added Services from September 1, 2006 through August 31, 2007.
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.8
|
September 1, 2007
|
Revised Attachment B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2008.
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.10 | March 1, 2008 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.11 | September 1, 2008 | Revised Attachment B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2009. |
| Revision | 1.12 | March 1, 2009 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.13 | September 1, 2009 | Revised Attachment B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2010. |
| Revision | 1.14 | December 1, 2009 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.15 | March 1, 2010 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.16 | September 1, 2010 | Revised Attachement B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2011. |
| Revision | 1.17 | December 1, 2010 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.18 | March 1, 2011 | Revised Attachement B-3, Value-added Services, to reflect mid-year negotiated Value-added Services for FY 2011. |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
Physical Health Value-added Services
|
||||||||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|||||
| NurseWise | Twenty-four hour nurse advice line | Available to all members by calling the Member Services toll-free number | NurseWIse, an affiliate of Centene Corporation | |||||
| Transportation |
HMO will offer alternative transportation to HMO members that have trouble accessing the State's Medical Transportation Program in a timely manner to ensure access to their provider appointments. In addition, HMO will provide transportation to non-medical services such as health education programs, nutrition classes, and birth preparation classes. HMO's member service staff will approve and coordinate the transportation service and the type of transportation provided.
|
Members in the Nueces Service Area. The Transportation Authority in this area will not agree to allow the plan to purchase bus vouchers or tokens.
The bus tokens or other alternative transportation must be requested in advance of a provider visit and authorized by Superior’s Member Services Department.
|
Transit Authorities in applicable Service Area. | |||||
| Dental Benefit |
Basic dental benefits for pregnant Members age 21 and over. The following services, categorized by procedural code, are covered:
Preventive
D0120 Periodic oral evaluation
D0140 Limited oral evaluation
D0150 Comprehensive oral evaluation (initial)
D0170 Re-evaluation limited, problem focused
Radiographs
D0220 Intraoral periapical first film
D0230 Intraoral periapical each add'l film
D0270 Bitewing single film
D0272 Bitewings two film
D0274 Bitewings four film
D0330 Panoramic
Cleanings
D1110 Prophy-adult
D1204 Topical application of fluoride (prophy not included) adult
D1206 Fluoride varnish
|
Each Member is eligible to receive $250 in dental services per benefit year, from dentists who are contracted with Delta Dental Insurance Company. The Member must be pregnant at the time of receiving any dental service to be covered under this benefit.
|
Licensed dentists under contract with Delta Dental Insurance Company
|
|||||
|
Vision
|
Members can choose between an enhanced selection of prescription eyeglasses OR $100 towards the cost of any features or frames not covered under Medicaid. Members will be offered a selection of 50 standard-size frames at no cost to Member. Member will be able to choose from three frame styles, each in a choice of three colors.
|
If Member opts for the $100 allowance, Members are responsible for any charges that exceed the $100 allowance. Disposable contact lenses are excluded from this $100 allowance. This Value-Added benefit is only allowed one time per benefit period (i.e. 24-months).
OR
The enhanced choice of new prescription eyeglasses is available once per 24-month period. Coverage is for new frames and lenses and does not cover additional features such as tints and coating.
Providers must prescribe new glasses in compliance with the following specifications:
Frames
• American-made, unless foreign-made frames are comparable in quality and are less expensive
• Serviceable and able to meet statutory quality standards
• Composed of new materials
Lenses
• Plastic or clear glass (if applicable)
• Heat or chemically treated dress eyewear able to meet standards of the American Standard Prescription Requirements for first-quality glass lenses
• Composed of new materials
• A minimum kryptoc of 22 mm flat top lens or equivalent if bifocal
• A minimum flat top 7/25 lens or equivalent if trifocal
|
Total Vision Health Plan’s provider network which includes Optometrists and Opticians
|
|||||
|
Pre-programmed Cell Phones for High-Risk Pregnant Women
|
Superior will provide pre-programmed cell phones to pregnant women who have been identified as high-risk through its OB case management program. The cell phones may be used to contact the Member’s OB, Superior, NurseWise and any other key representative of Member’s choice at any time the Member has a concern she wishes to discuss over the telephone, including the appropriateness of seeking medical care in person.
|
Only one cell phone will be provided per high-risk pregnant Member (although lost phones will be replaced). The phone must be returned to Superior within 4 weeks of the Member’s delivery of the baby.
|
Superior HealthPlan Case Management staff
|
|||||
|
Prenatal health and birthing classes
|
Classes will be provided by SHP staff or facilitated by SHP and offered in SHP offices and other locations convenient to Members throughout the Service Areas. The classes are led by a registered nurse with the assistance of a CONNECTIONS/Promotoras representative. They cover the basics of prenatal care, including nutrition; the risk of smoking and benefits of smoking cessation; the progress of a fetus through the pregnancy; the importance of regular follow-up with medical providers; common health issues that occur during pregnancy; and, a review of SHP StartSmart and CONNECTIONS programs (e.g., availability of pre-programmed cell phones for high-risk pregnant women without good telecommunication support).
|
None
|
Superior’s CONNECTIONS staff
|
|||||
|
Home visits to New Mothers
|
Superior Social Work and/or CONNECTIONS staff will make home visits to any Member with a new baby. This visit provides for resource and education coordination as identified in the visit, and ensures Members and the new babies are keeping all post natal and newborn doctor visits. This benefit is available to all Superior Members who have delivered a baby.
|
Only that a member consent to the home visit.
|
Superior’s CONNECTIONS and Social Work staff provide this service.
|
|||||
|
Gift Program Pregnant Members
|
Gift for health-related items for pregnant Members completing visits during pregnancy. Members will receive gift catalog upon presenting documentation of visits. Gifts valued at approximately $50 each.
|
Member must complete 8 prenatal exams from an SHP network provider. The Provider overseeing OB care for the pregnant Member must sign plan-provided document showing all 8 visits completed
|
Superior Network OB Providers
|
|||||
| Gift Program for Pregnant Women | Infant Car Safety seat for members who attend at least one baby shower. Baby Showers will be held no less than monthly, in each of the El Paso and Nueces SDAs. Members will be allowed one care seat per pregnancy and must show their Superior ID card at the shower to qualify. Member must be pregnant and currently enrolled with Superior to be eligible for the infant car seat. | STAR Pregnant women in Nueces and El Paso SDA ONLY | MCA | |||||
|
Behavioral Health Value-added Services for Members Under 21
|
|||||||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
||||
|
Behavioral Health
|
Diversionary Services: These are services
intended to provide support to Members at high risk for hospitalization or acute care readmissision by helping them remain in the community setting, where they will be eligible to receive wraparound care, acute residential treatment, crisis stabilization services or other services that would help avoid unnecessary hospitalization.
|
These services must be authorized by Superior’s Behavioral Health Subcontractor on a case-by-case basis.
|
It is anticipated that these services will be rendered by providers under contract with Superior’s Behavioral Health Subcontractor.
|
||||
|
Behavioral Health
|
Superior’s Behavioral Health Subcontractor will authorize Behavioral Health practitioners in medical settings to provide health psychology interventions focused on the effective management of chronic medical conditions. These might include psycho-educational groups for chronic conditions, individual coaching for patients with chronic disease states, or skills training activities.
|
These services must be authorized by Superior’s Behavioral Health Subcontractor. The authorization will be tied to medical necessity.
|
It is anticipated that these services will be rendered by Superior’s behavioral health practitioners located in Superior’s contracted Federally Qualified Health Centers.
|
||||
|
Behavioral Health
|
Intensive Outpatient Treatment/Day Treatment (IOP)- Used as an alternative to or step down from more restrictive levels of care. | These services must be authorized by Superior’s Behavioral Health Material Subcontractor. In addition, the service will be authorized for greater than one and one half hours, but less than five hours per day. Amount, duration, and scope are based on medical necessity. |
It is anticipated that Superior’s contracted Behavioral Health Providers in each Service Area will render this service.
|
||||
|
Behavioral Health
|
Partial Hospitalization/Extended Day Treatment- An alternative to, or a step down from, inpatient care.
|
These services must be authorized by Superior’s Behavioral Health Subcontractor. Services are authorized for a minimum of five hours, but for less than 24-hours per day. The amount, duration, and scope will be based on medical necessity.
|
It is anticipated that Superior’s contracted Behavioral Health Providers in each Service Area will render this service.
|
||||
| Behavioral Health | Rehabilitation/skills training. These are services provided to pregnant and parenting substance abusers at MHMR centers or in other treatment settings, focusing both on substance abuse and parenting issues. An augmentation of standard substance abuse treatment to focus on the special needs of this population. This benefit is available to all Members. It is geared to pregnant women and parenting Members. | These services must be authorized by Superior’s Behavioral Health Subcontractor. In addition, the service will be authorized for15-minute increments. The amount, duration, and scope are based on medical necessity. |
It is anticipated that Superior’s contracted MHMR providers specializing in Rehabilitation/Skills training in each Service Area will render this service.
|
||||
|
Behavioral Health Value-added Services for Members 21 and Over
|
||||||||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|||||
|
Behavioral Health
|
Diversionary Services: These are services
intended to provide support to Members at high risk for hospitalization or acute care readmissision by helping them remain in the community setting, where they will be eligible to receive wraparound care, acute residential treatment, crisis stabilization services or other services that would help avoid unnecessary hospitalization.
|
These services must be authorized by Superior’s Behavioral Health Subcontractor on a case-by-case basis.
|
It is anticipated that these services will be rendered by providers under contract with Superior’s Behavioral Health Subcontractor.
|
|||||
|
Behavioral Health
|
Superior’s Behavioral Health Subcontractor, will authorize Behavioral Health practitioners in medical settings to provide health psychology interventions focused on the effective management of chronic medical conditions. These might include psycho-educational groups for chronic conditions, individual coaching for patients with chronic disease states, or skills training activities.
|
These services must be authorized by Superior’s Behavioral Health Subcontractor. The authorization will be tied to medical necessity.
|
It is anticipated that these services will be rendered by Superior’s behavioral health practitioners located in Superior’s contracted Federally Qualified Health Centers.
|
|||||
|
Behavioral Health
|
Intensive Outpatient Treatment/Day Treatment (IOP)- Used as an alternative to or step down from more restrictive levels of care.
|
These services must be authorized by Superior’s Behavioral Health Subcontractor. In addition, the service will be authorized for greater than one and one half hours, but less than five hours per day. Amount, duration, and scope are based on medical necessity.
|
It is anticipated that Superior’s contracted Behavioral Health Providers in each Service Area will render this service.
|
|||||
|
Behavioral Health
|
Partial Hospitalization/Extended Day Treatment- An alternative to, or a step down from, inpatient care.
|
These services must be authorized by Superior’s Behavioral Health Subcontractor. Services are authorized for a minimum of five hours, but for less than 24-hours per day. The amount, duration, and scope will be based on medical necessity.
|
It is anticipated that Superior’s contracted Behavioral Health Providers in each Service Area will render this service.
|
|||||
| Behavioral Health | Rehabilitation/skills training. These are services provided to pregnant and parenting substance abusers at MHMR centers or in other treatment settings, focusing both on substance abuse and parenting issues. An augmentation of standard substance abuse treatment to focus on the special needs of this population. This benefit is available to all Members. It is geared to pregnant women and parenting Members. | These services must be authorized by Superior’s Behavioral Health Subcontractor. In addition, the service will be authorized for15-minute increments. The amount, duration, and scope are based on medical necessity. | It is anticipated that Superior’s contracted MHMR providers specializing in Rehabilitation/Skills training in each Service Area will render this service. | |||||
|
1. Explain how and when Providers and Members will be notified about the availability of the value-added services to be provided.
|
|
Value Added Services information will be included in the Superior Provider Manual and also during training sessions. Members will receive this information via the Plan Comparison Chart, in the Member Handbook, with New Member Packets, Connections/Promotoras and during orientations. Periodically, Superior will also highlight Value Added Services in the Provider and Member Newsletters.
Members in the Nueces and El Paso SDAs will be made aware of this benefit, in addition to the mediums listed above, also through Member Advisory Committees, OB Case Management Program materials and staff, Plan-sponsored baby showers, OB START SMART Pregnancy Program and Materials, Plan-sponsored health events, or other HHSC-approved/sponsored events in which Superior participates. In addition, Providers will be informed about this VAS through email communications, and face to face orientations and visits with providers.
|
|
2. Describe how a Member may obtain or access the value-added services to be provided.
|
|
See explanations provided above for accessing services.
A Member may access the Home Visits to New Mothers service by accepting a home visit appointment from a Superior Social Work or CONNECTIONS staff member.
With respect to the Transportation Value-added Service, “alternative transportation” refers to taxi cab services, which will be pre-authorized on a case-by-case basis for Members with respect to whom bus service is not accessible or convenient or where the particular health condition of the Member makes taxi cab services a medically preferable alternative to waiting for and riding a bus to a medical appointment.
With respect to the Gift Card Program for Prenatal Care, in order for Member to receive gift catalog, the Member must submit to SHP the plan provider signed document showing that all 8 visits were completed. To receive the gift catalog, eight (8) visits must be completed regardless of when in her pregnancy the Member joins the health plan. If the Member changes OB providers before completing the 8 visits, visits completed with the prior OB provider will count toward the 8 visit total.
|
|
Superior will track the value added services through our claims system for those value-adds for which HIPAA-compliant procedural codes are available (vision, dental, behavioral health). Superior will create a specific benefit category to track and report the value added services 'separately' from our 'capitated' service data. In addition, Superior will have the ability to pass this information to the State utilizing the encounter submission process, as long as the State is able to segregate the value adds data from the capitated services data.
For transportation services, Superior will maintain an electronic file of transportation services provided for Superior’s membership.
Home visits to new mothers are tracked through Superior’s case management system. Each staff member logs each member visit and the outcome/findings of the visit in Superior’s computer system. Superior will work with HHSC to establish the most efficient transmission of the data.
Distribution of pre-programmed cell phones will be tracked via the OB Case Management Team
Attendance at prenatal classes will be tracked via Connections/Promotoras staff.
The Diversionary Behavioral Health Services will be identified by Rev 900, CPT 90899, and HCPC code H2021/H2022.
|
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
n/a
|
Initial version of Attachment B-3, Value-added Services.
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.2
|
September 1. 2006
|
Revised Physical Health Value-added Services to include Home Visits to New Mothers. Revised the certification provision by changing the start date for the 12-month provision of services.
|
|
Revision
|
1.3
|
September 1, 2006
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment removed the separate signature requirement for Attachment B-3, Value-added Services. By signing the Contract and/or Contract Amendment, the HMO certifies that it will provide the Value-added Services from September 1, 2006 through August 31, 2007.
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
|
Revision
|
1.8
|
September 1, 2007
|
Revised Attachment B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2008.
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.10 | March 1, 2008 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.11 | September 1, 2008 |
Revised Attachment B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2009.
|
| Revision | 1.12 | March 1, 2009 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.13 | September 1, 2009 |
Revised Attachment B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2010.
|
| Revision | 1.14 | December 1, 2009 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.15 | March 1, 2010 |
Contract amendment did not revise Attachment B-3, Value-added Services.
|
| Revision | 1.16 | September 1, 2010 |
Revised Attachment B-3, Value-added Services, to reflect newly negotiated Value-added Services for FY 2011.
|
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment B-3, Value-added Services. |
| Revision | 1.18 | March 1, 2011 | Contract amendment did not revise Attachment B-3, Value-added Services. |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
Physical Health Value-added Services
|
|||||||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
||||
|
NurseWise
|
Twenty-four hour nurse advice line
|
Available to all members by calling the Member Services toll-free number
|
NurseWise, an affiliate of Centene Corporation
|
|
Transportation
|
For Members in need of transportation that cannot access transportation in a timely manner, Superior will provide alternative transportation to ensure that Members have a means of accessing their provider appointment.
|
Members in the Nueces Service Area. The Transportation Authority in this area will not agree to allow the plan to purchase bus vouchers or tokens.
The bus tokens or other alternative transportation must be requested in advance of a provider visit and authorized by Superior’s Member Services
Department. |
Transit Authorities in applicable Service Area.
|
|
Vision
|
20% discount off of Upgraded Hardware- The Member will receive a 20% discount on upgraded hardware.
|
There is no limitation on the number of times the discount can be utilized.
|
TVHP contracted providers.
|
|
Behavioral Health Value-added Services for Members Under 21
|
|||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|
Behavioral Health Value-added Services for Members 21 and Over
|
|||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|
1. Explain how and when Providers and Members will be notified about the availability of the value-added services to be provided.
|
|
Value Added Services information will be included in the Superior Provider Manual and also during training sessions. Members will receive this information via the Plan Comparison Chart, in the Member Handbook, with New Member Packets and during orientations. Periodically, Superior will also highlight Value Added Services in the Provider and Member Newsletters.
|
|
2. Describe how a Member may obtain or access the value-added services to be provided.
|
|
See explanations provided above for accessing services.
With respect to the Transportation Value-added Service, “alternative transportation” refers to taxi cab services, which will be pre-authorized on a case-by-case basis for members with respect to whom bus service is not accessible or convenient or where the particular health condition of the member makes taxi cab services a medically preferable alternative to waiting for and riding a bus to a medical appointment.
|
3. Describe how the HMO will identify the Value-added Service in administrative (encounter) data.
|
Superior will track the value added services through our claims system for those value-adds for which HIPAA-compliant procedural codes are available (such as vision). Superior will create a specific benefit category to track and report the value added services 'separately' from our 'capitated' service data. In addition, Superior will have the ability to pass this information to the State utilizing the encounter submission process, as long as the State is able to segregate the value adds data from the capitated services data.
For transportation services, Superior will maintain an electronic file of transportation services provided for Superior’s membership.
|
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
1.0
|
Initial version of Attachment B-3, Value-added Services
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Revised Attachment B-3, Value Added Services, by adding Attachment B-3.1, STAR+PLUS Value Added Services. This is the initial version of Attachment B-3.1, STAR+PLUS VAS.
|
|
Revision
|
1.2
|
September 1, 2006
|
Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services
|
|
Revision
|
1.3
|
September 1, 2006
|
Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment removed the separate signature requirement for Attachment B-3.1, STAR+PLUS Value-added Services. By signing the Contract and/or Contract Amendment, the HMO certifies that it will provide the Value-added Services from January 1, 2007 through August 31, 2007.
|
|
Revision
|
1.5
|
January 1, 2007
|
Revised Attachment B-3.1, STAR+PLUS Value Added Services to state that only non-dual members are eligible for dental benefits and to clarify description of Out-of-Home Respite.
|
|
Revision
|
1.6
|
February 1, 2007
|
Revised Attachment B-3.1, STAR+PLUS Value Added Services, to clarify the coverage period for the VAS.
|
|
Revision
|
1.7
|
July 1, 2007
|
Revised Attachment B-3.1, STAR+PLUS Value Added Services, to clarify the coverage period for the VAS.
|
|
Revision
|
1.8
|
September 1, 2007
|
Revised Attachment B-3-1, STAR+PLUS Value-added Services, to reflect newly negotiated Value-added Services for FY 2008.
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services
|
| Revision | 1.10 | March 1, 2008 | Revised Attachment B-3-1, STAR+PLUS Value-added Services, to reflect mid year negotiated Value-added Services for FY 2008. |
| Revision | 1.11 | September 1, 2008 |
Revised Attachment B-3-1, STAR+PLUS Value-added Services, to reflect newly negotiated Value-added Services for FY 2009.
|
| Revision | 1.12 | March 1, 2009 |
Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services
|
| Revision | 1.13 | September 1, 2009 |
Revised Attachment B-3-1, STAR+PLUS Value-added Services, to reflect newly negotiated Value-added Services for FY 2010.
|
| Revision | 1.14 | December 1, 2009 |
Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services
|
| Revision | 1.15 | March 1, 2010 |
Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services
|
| Revision | 1.16 | September 1, 2010 |
Revised Attachment B-3-1, STAR+PLUS Value-added Services, to reflect newly negotiated Value-added Services for FY 2011.
|
| Revision | 1.17 | December 1, 2010 |
Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services
|
| Revision | 1.18 | March 1, 2011 | Contract amendment did not revise Attachment B-3.1, STAR+PLUS Value Added Services |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
Physical Health Value-added Services
|
|||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|
NurseWise
|
Twenty-four hour nurse advice line
|
Available to all members by calling the Member Services toll-free number
|
NurseWise, an affiliate of Centene Corporation
|
|
Dental
|
Basic dental coverage. The following services, categorized by CPT code, are covered:
Preventive
D0120 Periodic oral evaluation
D0140 Limited oral evaluation
D0150 Comprehensive oral evaluation (initial)
D0170 Re-evaluation limited, problem focused
Radiographs
D0220 Intraoral periapical first film
D0230 Intraoral periapical each add'l film
D0270 Bitewing single film
D0272 Bitewings two film
D0274 Bitewings four film
D0330 Panoramic
Cleanings
D1110 Prophy-adult
D1204 Topical application of fluoride (prophy not included) adult
D1206 Fluoride varnish
|
Only non-dual Members aged 21 years and over are eligible for dental benefits.
Each non-dual Member is eligible to receive $250 in dental services per benefit year, from dentists who are contracted with Delta Dental Insurance Company.
|
Licensed dentists under contract with Delta Dental Insurance Company
|
| Vision |
Members will be provided an enhanced choice of prescription eyeglasses. Members will be offered a selection of 50 standard-size frames at no cost to Member. The Member will be able to choose from three frame styles, each in a choice of three colors. The provider must include an all-metal frame in lieu of a colored frame.
|
Only non-dual Members aged 21 years and over are eligible for vision benefits.
The enhanced choice of new prescription eyeglasses is available once per 24-month period. Coverage is for new frames and lenses and does not cover additional features such as tints and coating.
Providers must prescribe new glasses in compliance with the following specifications:
Frames
• American-made, unless foreign-made frames are comparable in quality and are less expensive
• Serviceable and able to meet statutory quality standards
• Composed of new materials
Lenses
• Plastic or clear glass (if applicable)
• Heat or chemically treated dress eyewear able to meet standards of the American Standard Prescription Requirements for first-quality glass
lenses
• Composed of new materials
• A minimum kryptoc of 22 mm flat top lens or equivalent if bifocal
• A minimum flat top 7/25 lens or equivalent if trifocal
|
Total Vision Health Plan’s provider network which includes Optometrists and Opticians
|
|
Pre-programmed Cell Phones for High-Risk Pregnant Women
|
Superior will provide pre-programmed cell phones to pregnant women who have been identified as high-risk through its OB case management program. The cell phones may be used to contact the Member’s OB, Superior, NurseWise and any other key representative of Member’s choice at any time the Member has a concern she wishes to discuss over the telephone, including the appropriateness of seeking medical care in person
|
Only non-dual Members are eligible for the cell phone
Only one cell phone will be provided per high-risk pregnant Member (although lost phones will be replaced). The phone must be returned to Superior within 4 weeks of the Member’s delivery of the baby.
|
Superior HealthPlan Case Management staff
|
|
Prenatal health and birthing classes
|
Classes will be provided by SHP staff or facilitated by SHP and offered in SHP offices and other locations convenient to Members throughout the Service Areas. The classes are led by a registered nurse with the assistance of a CONNECTIONS/Promotoras representative. They cover the basics of prenatal care, including nutrition; the risk of smoking and benefits of smoking cessation; the progress of a fetus through the pregnancy; the importance of regular follow-up with medical providers; common health issues that occur during pregnancy; and, a review of SHP StartSmart and CONNECTIONS programs (e.g., availability of pre-programmed cell phones for high-risk pregnant women without good telecommunication support). |
None.
|
Superior’s CONNECTIONS staff
|
|
Gift Program for Pregnant Members
|
Gift for health-related items for pregnant Members completing visits during pregnancy. Members will receive gift catalog upon presenting documentation of visits. Gifts valued at approximately $50 each.
|
Only non-dual Members are eligible for the gift program.
The Member must complete 8 prenatal exams from an SHP network provider. The Provider overseeing OB care for the pregnant Member must sign a plan-provided document showing that all 8 visits were completed
|
Superior Network OB Providers
|
|
Transportation
|
HMO will offer tokens or vouchers for alternative transportation to HMO members that have trouble accessing the State's Medical Transportation Program in a timely manner to ensure access to their provider appointments. HMO's Member Services staff will approve and coordinate the transportation service and the type of transportation provided.
|
Bus tokens or other alternative transportation must be requested in advance of a provider visit and authorized by Superior’s Member Services Department.
|
Transit Authorities in applicable Service Area
|
|
Behavioral Health Value-added Services for Members 21 and Over
|
||||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|
|
Behavioral Health
|
Health Psychology Interventions provided by a behavioral health practitioner in a medical setting that focuses on the effective management of chronic medical conditions. This might include psycho-educational groups for chronic conditions, individual coaching for patients with chronic disease states, or skills training activities.
|
Limited to non-dual Members only. Services must be authorized and is based on medical necessity.
|
Network Federally Qualified Health Centers (FQHCs)
|
|
|
Behavioral Health
|
Intensive Outpatient Treatment/Day Treatment (IOP)- Used as an alternative to step down from more restrictive levels of care.
|
Limited to non-dual Members only. Services must be authorized and is based on medical necessity. Services will be authorized for greater than one and one half hours, but less than five hours per day.
|
It is anticipated that behavioral health providers within the Service Area will render this service.
|
|
|
Behavioral Health
|
Partial Hospitalization/Extended Day Treatment- An alternative to, or a step down from, inpatient care.
|
Limited to non-dual Members only. Services must be authorized and is based on medical necessity. Services will be authorized for a minimum of five hours, but for less than 24-hours per day.
|
It is anticipated that behavioral health providers within the Service Area will render this service.
|
|
|
Behavioral Health
|
Diversionary Services: These are services
intended to provide support to Members at high risk for hospitalization or acute care readmissision by helping them remain in the community setting, where they will be eligible to receive wraparound care, acute residential treatment, crisis stabilization services or other services that would help avoid unnecessary hospitalization.
|
These services must be authorized by Superior's Behavioral Health Subcontractor on a case-by-case basis.
|
It is anticipated that behavioral health providers within the Service Area will render this service.
|
|
|
1. Explain how and when Providers and Members will be notified about the availability of the value-added services to be provided.
|
|
|
Value added services information will be included in the Superior Provider Manual and also during training sessions. Members will receive this information via the Plan Comparison Chart, in the Member Handbook, with New Member Packets, through Service Coordination and Member Services, and during orientations. Periodically, Superior will also highlight Value Added Services in the Provider and member Newsletters.
|
|
2. Describe how a Member may obtain or access the value-added services to be provided.
|
|
See explanations provided above for accessing services.
|
|
3. Describe how the HMO will identify the Value-added Service in administrative (encounter) data.
|
|
Superior will track value added services through our claims system for those value-adds for which HIPAA-compliant procedural codes are available (podiatry, etc.). Superior will create specific benefit categories to track and report the value added services “separately” from our “capitated” service data. In addition, Superior will have the ability to pass this information to the State utilizing the encounter submission process, as long as the State is able to segregate the value adds data from the capitated services data.
For dental and vision services, Superior will receive a data file from the dental and vision vendors to capture all utilization of dental value added benefits.
Distribution of pre-programmed cell phones will be tracked via the Superior OB Case Management Team
Attendance at prenatal classes will be tracked via Superior’s Connections/Promotoras staff.
For transportation services, Superior will maintain an electronic file of transportation services provided for Superior’s membership.
The Diversionary Behavioral Health Services will be identified by Rev 900, CPT 90899, and HCPC code H2021/H2022.
|
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
1.0
|
Initial version of Attachment B-3, Value-added Services
|
|
|
Revision
|
1.1
|
June 30, 2006
|
Revised Attachment B-3, Value Added Services, by adding Attachment B-3.1, STAR+PLUS Value Added Services.
|
|
Revision
|
1.2
|
September 1, 2006
|
Contract amendment did not revise Attachment B-3, Value Added Services
|
|
Revision
|
1.3
|
September 1, 2006
|
Revised Attachment B-3, Value Added Services, by adding Attachment B-3.2, CHIP Perinatal Program Value Added Services. This is the initial version of Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment removed the separate signature requirement for Attachment B-3.2, CHIP Perinatal Program Value-added Services. By signing the Contract and/or Contract Amendment, the HMO certifies that it will provide the Value-added Services from January 1, 2007 through August 31, 2007.
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
|
Revision
|
1.8
|
September 1, 2007
|
Revised Attachment B-3.2, CHIP Perinatal Program Value-added Services, to reflect newly negotiated Value-added Services for FY 2008.
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
| Revision | 1.10 | March 1, 2008 | Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services |
| Revision | 1.11 | September 1, 2008 |
Revised Attachment B-3.2, CHIP Perinatal Program Value-added Services, to reflect newly negotiated Value-added Services for FY 2009.
|
| Revision | 1.12 | March 1, 2009 |
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
| Revision | 1.13 | September 1, 2009 | Revised Attachment B-3.2, CHIP Perinatal Program Value-added Services, to reflect newly negotiated Value-added Services for FY 2010. |
| Revision | 1.14 | December 1, 2009 |
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
| Revision | 1.15 | March 1, 2010 |
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
| Revision | 1.16 | September 1, 2010 | Revised Attachment B-3.2, CHIP Perinatal Program Value-added Services, to reflect newly negotiated Value-added Services for FY 2011. |
| Revision | 1.17 | December 1, 2010 |
Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services.
|
| Revision | 1.18 | March 1, 2011 | Contract amendment did not revise Attachment B-3.2, CHIP Perinatal Program Value Added Services. |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
Physical Health Value-added Services
|
|||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|
Behavioral Health Value-added Services for Members Under 21
|
|||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|
Behavioral Health Value-added Services for Members 21 and Over
|
|||
|
Value-added Service
|
Description of Value-added Services and Members Eligible to Receive the Services
|
Limitations or Restrictions
|
Provider(s) responsible for providing this service
|
|
1. Explain how and when Providers and Members will be notified about the availability of the value-added services to be provided.
|
|
2. Describe how a Member may obtain or access the value-added services to be provided.
|
|
3. Describe how the HMO will identify the Value-added Service in administrative (encounter) data.
|
|
DOCUMENT HISTORY LOG
|
||||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
|
Baseline
|
n/a
|
Initial version Attachment B-4, Performance Improvement Goals.
|
||
|
Revision
|
1.1
|
June 30, 2006
|
Contract amendment to include STAR+PLUS Program. Revised Attachment B-4, Performance Improvement Goals Template, by adding Attachment B-4.1, FY2008 Performance Improvement Goals Template. No change to this Section.
|
|
|
Revision
|
1.2
|
September 1, 2006
|
Revised version of Attachment B-4 that includes provisions applicable to MCOs participating in the STAR and CHIP Programs.
Updates the attachment to reflect the changes made in Attachment B-1, Section 8.1.1.1.
|
|
|
Revision
|
1.3
|
September 1, 2006
|
Contract amendment did not revise Attachment B-4, Performance Improvement Goals.
|
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amended to include Attachment B-4 Performance Improvement Goals for SFY2007 and format change
|
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-4, Performance Improvement Goals.
|
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-4, Performance Improvement Goals.
|
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-4, Performance Improvement Goals.
|
|
|
Revision
|
1.8
|
September 1, 2007
|
Revised Attachment B-4, to replace FY2007 Performance Improvement Goals with newly negotiated FY2008 Performance Improvement Goals by Program and by Service Area. Attachment B-4.1, FY2008 Performance Improvement Goals Template, is deleted as duplicative.
|
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-4, Performance Improvement Goals.
|
|
| Revision | 1.10 | March 1, 2008 |
Contract amendment did not revise Attachment B-4, Performance Improvement Goals.
|
|
| Revision | 1.11 | September 1, 2008 | Revised Attachment B-4, to replace FY2008 Performance Improvement Goals with newly negotiated FY2009 Performance Improvement Goals by Program and by Service Area. | |
| Revision | 1.12 | March 1, 2009 | Contract amendment did not revise Attachment B-4, Performance Improvement Goals | |
| Revision | 1.13 | September 1, 2009 |
Revised Attachment B-4, to replace FY2009 Performance Improvement Goals with newly negotiated FY2010 Performance Improvement Goals by Program and by Service Area.
Attachment B-4 is modified to clarify the aplicability of Goals 1 and 2, updated Goal 3 for STAR, CHIP, and CHIP Perinatal, and add a Goal 3 for STAR+PLUS.
|
|
| Revision | 1.14 | December 1, 2009 | Contract amendment did not revise Attachment B-4, Performance Improvement Goals | |
| Revision | 1.15 | March 1, 2010 | Contract amendment did not revise Attachment B-4, Performance Improvement Goals | |
| Revision | 1.16 | September 1, 2010 |
Revised Attachment B-4, to replace FY2010 Performance Improvement Goals with newly negotiated FY2011 Performance Improvement Goals by Program.
Attachment B-4 is modified to remove Service Areas as a category for sub-goals; update Goal 1 for STAR, STAR+PLUS, CHIP, and CHIP Perinatal; update Goal 2 for STAR, STAR+PLUS, and CHIP; and remove Goal 3 for all programs.
|
|
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment B-4, Performance Improvement Goals | |
| Revision | 1.18 | March 1, 2011 | Attachment B-4 is revised to change the name from "Performance Improvement Goals" to "Performance Improvement Projects" and to reflect negotiated Performance Improvement Projects for FY 2011. | |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
||||
|
A. Health Plan Information
Plan Name: Superior HealthPlan
HMO Program: CHIP
|
||
|
B. Overarching Goal
|
C. Sub Goals:
|
|
|
Goal 1:
Improve treatment for ACSC through reduction of inpatient admissions and/or emergency department visits.
|
Reduce ER utilization rate for ACSCs by 2% for PCPs with over 100 covered lives (members included must have been with PCP for 90 days).
Reduce inpatient admissions related to asthma by 2% by year-end.
|
|
|
Goal 2:
Increase access to needed care and specialized services, including behavioral health treatment and counseling.
|
Increase the rate of 7 day follow-up after behavioral health hospitalization to the 50th percentile of HEDIS.
Increase access to behavioral health appointments for urgent care by 5 percentage points for the year.
|
|
|
Goal 3:
|
||
|
A. Health Plan Information
Plan Name: Superior HealthPlan
HMO Program: STAR
|
|
B. Overarching Goal
|
C. Sub Goals:
|
|
|
Goal 1:
Improve treatment for ACSC through reduction of inpatient admissions.
|
Reduce inpatient admissions of uncontrolled DM by 2% by year-end.
Reduce inpatient admissions of asthma by 2% by year-end.
|
|
|
Goal 2:
Improve treatment for ACSC through reduction of emergency department visits.
|
Reduce ER utilization rate for ACSCs by 1% for PCPs with over 100 covered lives (members included must have been with PCP for 90 days).
Reduce ER Utilization for asthma by 2% by year-end.
|
|
|
Goal 3:
|
|
A. Health Plan Information
Plan Name: Superior HealthPlan
HMO Program: STAR+PLUS
|
||
|
B. Overarching Goal
|
C. Sub Goals:
|
|
|
Goal 1:
Improve treatment for ACSC through reduction of inpatient admissions.
|
Reduce inpatient admissions of uncontrolled DM by 2% by year-end.
Reduce inpatient admissions of asthma by 2% by year-end.
|
|
|
Goal 2:
Improve treatment for ACSC through reduction of emergency department visits.
|
Reduce ER utilization rate for ACSCs by 1% for PCPs with over 100 covered lives (members included must have been with PCP for 90 days).
Reduce ER utilization of uncontrolled DM by 2% by year-end.
|
|
|
Goal 3:
|
||
|
A. Health Plan Information
Plan Name: Superior HealthPlan
HMO Program: CHIP Perinatal
|
|
B. Overarching Goal
|
C. Sub Goals:
|
|
|
Goal 1:
Improve prenatal care received by CHIP Perinate members
|
Increase the percentage of deliveries by 1% that received a prenatal care visit in the first trimester or within 42 days of enrollment in the organization.
Increase 17P utilization by 5% by year-end.
|
|
|
Goal 3:
|
|
DOCUMENT HISTORY LOG
|
||||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
|
Baseline
|
n/a
|
Initial version of Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
||
|
Revision
|
1.1
|
June 30, 2006
|
Contract amendment did not revise Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
|
|
Revision
|
1.2
|
September 1, 2006
|
Amended Attachment B-5, Deliverables/Liquidated Damages Matrix, to add a footnote clarifying the deliverable due dates. Also amended the provisions regarding Claims Processing Requirements and the Reporting Requirements for the Claims Summary Report.
|
|
|
Revision
|
1.3
|
September 1, 2006
|
Amended Attachment B-5, Deliverables/Liquidated Damages Matrix, performance standard for Provider Directories for the CHIP Perinatal Program.
|
|
|
Revision
|
1.4
|
September 1, 2006
|
Contract amendment did not revise Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
|
|
Revision
|
1.5
|
January 1, 2007
|
Contract amendment did not revise Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
|
|
Revision
|
1.7
|
July 1, 2007
|
Amended Attachment B-5, Deliverables/Liquidated Damages Matrix, to add clarifications to the provisions addressing Claims Processing Requirements and the Reporting Requirements for the Claims Summary Report.
|
|
|
Revision
|
1.8
|
September 1, 2007
|
Contract amendment did not revise Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
|
| Revision | 1.10 | March 1, 2008 |
Amended Attachment B-5 to add or revise performance standards and liquidated damages regarding: Failure to Perform an Administrative Service; Failure to Provide a Covered Service; Behavioral Health Services Hotline; Member Services Hotline; and Provider Hotline.
|
|
| Revision | 1.11 | September 1, 2008 |
Amended Attachment B-5 to revise performance standards regarding: Line 1 – Failure to Perform an Administrative Service and Line 2 – Failure to Provide a Covered Service; and to replace the MDS-HC instrument with the Community Medical Necessity and Level of Care Assessment Instrument in the Performance Standard for Line 21 – Contract Amendment B-1 RFP §8.3.3 – STAR+PLUS Assessment Instruments
|
|
| Revision | 1.12 | March 1, 2009 |
Lines 8, 9, and 13 are modified to add a performance standard, measurement assessment, and damages for each 30 second time increment, or portion thereof, by which the average hold time exceeds the maximum acceptable hold time.
Line 15 is modified to clarify reporting timeframes and requirements.
|
|
| Revision | 1.13 | September 1, 2009 |
Line 16.5 Contract Attachment B-1 RFP §8.1.18.1 Encounter Data is added.
Line 21 Performance Standard is amended to clarify type of wiaver services.
|
|
| Revision | 1.14 | December 1, 2009 | Line 21 Service/Component is amended to clarify contract references and Performance Standard is modified to require that assessment instructions must be submitted within 45 days | |
| Revision | 1.15 | March 1, 2010 | Line 3 modified to conform to language in Attachment A, Sections 4.08(b)(3) and (4). | |
| Revision | 1.16 | September 1, 2010 |
Item 3 is modified to conform to language in Attachment A, Sections 4.08(b)(3) and (4).
Item 8 is added to add liquidated damages for Out-of-Network Utilization.
Item 22 is added to add liquidated damages for timely HMO response to complaints.
All subsequent items are renumbered.
|
|
| Revision | 1.17 | December 1, 2010 |
Contract amendment did not revise Attachment B-5, Deliverables/Liquidated Damage Matrix.
|
|
| Revision | 1.18 | March 1, 2011 |
Item 11 modified to add liquidated damages for failing to submit timely HMO response to Provider complaints.
|
|
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
||||
|
Service/
Component1
|
Performance Standard2
|
Measurement Period3
|
Measurement Assessment4
|
Liquidated Damages
|
|
General Requirement:
Failure to Perform an Administrative Service
Contract Attachment A HHSC Uniform Managed Care Contract Terms and Conditions,
Contract Attachment B-1 RFP §§ 6, 7, 8 and 9
|
The HMO fails to timely perform an HMO Administrative Service that is not otherwise associated with a performance standard in this matrix and, in the determination of HHSC, such failure either: (1) results in actual harm to a Member or places a Member at risk of imminent harm, or (2) materially affects HHSC’s ability to administer the Program(s).
|
Ongoing
|
Each incident of non-compliance per HMO Program and SA.
|
HHSC may assess up to $5,000 per calendar day for each incident of non-compliance per HMO Program and SA.
|
|
General Requirement:
Failure to Profide a Covered Service
Contract Attachment A HHSC Uniform Managed Care Contract Terms and Conditions,
Contract Attachment B-1 RFP §§ 6, 7, 8 and 9
|
The HMO fails to timely provide a HMO Covered Service that is not otherwise associated with a performance standard in this matrix and, in the determination of HHSC, such failure results in actual harm to a Member or places a Member at risk of imminent harm.
|
Ongoing | Each calendar day of non-compliance. |
HHSC may assess up to $7,500.00 per day for each incident of non-compliance.
|
| Contract Attachment A HHSC Uniform Managed Care Contract Terms and Conditions, Section 4.08 Subcontractors |
(i) three (3) Business Days after receiving notice from a Material Subcontractor of its intent to terminate a Subcontract;
(ii) 180 calendar days prior to the termination date of a Material Subcontract for MIS systems operation or reporting;
(iii) 90 calendar days prior to the termination date of a Material Subcontract for non-MIS HMO Administrative Services; and
(iv) 30 calendar days prior to the termination date of any other Material Subcontract.
|
Transition, Measured Quarterly during the Operations Period | Each calendar day of non-compliance, per HMO Program, per SA.. | HHSC may assess up to $5,000 per calendar day of non-compliance |
|
Contract Attachment B-1 RFP §§ 6, 7, 8 and 9
Uniform Managed Care Manual
|
All reports and deliverables as specified in Sections 6, 7, 8 and 9 of Attachment B-1 must be submitted according to the timeframes and requirements stated in the Contract (including all attachments) and HHSC’s Uniform Managed Care Manual. (Specific Reports or deliverables listed separately in this matrix are subject to the specified liquidated damages.) |
Transition Period, Quarterly during Operations Period
|
Each calendar day of non-compliance, per HMO Program, per SA.
|
HHSC may assess up to $250 per calendar day if the report/deliverable is late, inaccurate, or incomplete.
|
|
Contract Attachment B-1, RFP §7.3 --Transition Phase Schedule
Contract Attachment B-1, RFP §7.3.1 -- Transition Phase Tasks
Contract Attachment B-1, RFP §8.1 -- General Scope
|
The HMO must be operational no later than the agreed upon Operations Start Date. HHSC, or its agent, will determine when the HMO is considered to be operational based on the requirements in Section 7 and 8 of Attachment B-1. | Operations Start Date | Each calendar da of non-compliance, per HMO Program, per Service Area (SA). | HHSC may asses up to $10,000 per calendar day for each day beyond the Operations Start date that the HMO is not operational until the day that the HMO is operational, including all systems. |
|
Contract Attachment B-1 RFP §7.3.1.5 -- Systems Readiness Review
|
The HMO must submit to HHSC or to the designated Readiness Review Contractor the following plans for review, by December 14, 2005 for STAR and CHIP, and by July 31, 2006 for STAR+PLUS:
• Joint Interface Plan;
• Disaster Recovery Plan;
• Business Continuity Plan;
• Risk Management Plan; and
- Systems Quality Assurance Plan.
|
Transition Period
|
Each calendar day of non-compliance, per report, per HMO Program, and per SA.
|
HHSC may asses up to $1,000 per calendar day for each day a deliverable is late, inaccurate or incomplete.
|
|
Contract Attachment B-1 RFP 7.3.1.7 - Operations Readiness
|
Final versions of the Provider Directory must be submitted to the Administrative Services Contractor no later than 95 days prior to the Operational Start Date for the CHIP, STAR, and STAR+PLUS HMOs, and no later than 30 days prior to the Operational Start Date for the CHIP Perinatal HMOs.
|
Transition Peroid |
Each calendar day of non-compliance, per directory, per HMO Program and per SA.
|
HHSC may assess up to $1,000 per calendar day for each day the directory is late, inaccurate or incomplete.
|
|
Contract Attachment B-1 RFP §8.1.4 Provider Network
UMCM Chapter 5.38 Out of Network Utilization Report
|
(1) No more than 15 percent of an MCO's total hospital admissions, by service delivery area, may occur in out-of-network facilities.
(2) No more than 20 percent of an MCO's total emergency room visits, by service delivery area, may occur in out-of-network facilities
(3) No more than 20 percent of total dollars billed to an MCO for "other outpatient services" may be billed by out-of-network providers.
|
Measured Quarterly beginning March 1, 2010.
|
Per incident of non-compliance, per Medicaid HMO, per Service Area.
|
HHSC may assess up to $25,000 per quarter, per standard, per Medicaid HMO, per Service Area.
|
|
Contract Attachment B-1 RFP §8.1.4.7 -- Provider Hotline
|
A. The HMO must operate a toll-free Provider telephone hotline that Provider inquiries from 8 AM - 5 PM, local time for the Service Area, Monday through Friday, excluding State-approved holidays.
B. Performance Standards.
1. Call pickup rate - At least 99% of calls are answered on or before the fourth ring or an automated call pick up system is used.
2. Call hold rate - The average hold time is two minutes or less.
3. Call abandonment rate - Call abandonment rate is 7% or less.
C. Average hold time is 2 minutes or less.
|
Operations and Turnover |
A. Each incident of non-compliance per. HMO Program and SA.
B. Each percentage point below the standard for 1 and 2 and each percentage point above the standard for 3 per HMO Program and SA.
C Per month, for each 30 second time increment, or portion thereof, by which the average hold time exceeds the maximum acceptable hold time.
|
HHSC may assess:
A. Per HMO Program and SA, up to $100.00 for each hour or portion thereof that appropriately staffed toll-free lines are not operational. If the MCO's failure to meet the performance standard is caused by a Force Majeure Event, HHSC will not assess liquidated damages unless the MCO fails to implement its Disaster Recovery Plan.
B.Up to $100.00 per HMO Program and SA for each percentage point for each standard that the HMO fails to meet the requirements for a monthly reporting period for any HMO operated toll-free lines.
C. Up to $100.00 may be assessed fore each 30 second time increment, or portion thereof, by which the MCO's average hold time exceeds the maximum acceptable hold time.
|
| Contract Attachment B-1 RFP §8.1.5.6 -- Member Services Hotline | A. The HMO must operate a toll-free hotline that Members can call 24 hours a day, seven (7) days a week.
B. Performance Standards.
1. Call pickup rate - At least 99% of calls are answered on or before the fourth ring or an automated call pick up system is used.
2. Call hold rate - At least 80% of calls must be answered by toll-free line staff within 30 seconds.
3. Call abandonment rate - Call abandonment rate is 7% or less.
C. Averag hold time is 2 minutes or less.
|
Ongoing during Operations Turnover |
A. Each incident of non-compliance per. HMO Program and SA.
B. Each percentage point below the standard for 1 and 2 and each percentage point above the standard for 3 per HMO Program and SA.
C. Per month, for each 30 second time increment, or portion threof, by which the average hold time exceeds the maximum acceptable hold time.
|
HHSC may assess:
A. Per HMO Program and SA, up to $100.00 for each hour or portion thereof that toll-free lines are not operational. If the MCO's failure to meet the performance standard is caused by a Force Majeure Event, HHSC will not assess liquidated damages unless the MCO fails to implement its Disaster Recovery Plan.
B. Per HMO Program and SA, up to $100.00 for each percentage point for each standard that the HMO fails to meet the requirements for a monthly reporting period for any HMO operated toll-free lines.
C. Up to $100.00 may be assessed fore each 30 second time increment, or portion thereof, by which the MCO's average hold time exceeds the maximum acceptable hold time.
|
|
Contract Attachment B-1 RFP §8.1.5.9 -- Member Complaint and Appeal Process
Contract Attachment B-1 RFP §8.2.5.1 -- Provider Complaints
Contract Attachment B-1 RFP §8.2.7.1 -- Member Complaint Process
Contract Attachment B-1 RFP §8.4.3 – CHIP Member Complaint and Appeal Process
|
The HMO must resolve at least 98% of Member Complaints within 30 calendar days from the date the Complaint is received by the HMO.
|
Measured Quarterly during the Operations Period | Per reporting period, per HMO Program, per SA. | HHSC may assess up to $250 per reporting period if the HMO fails to meet the performance standard. |
|
Contract Attachment B-1 RFP §8.1.5.9 -- Member Complaint and Appeal Process
Contract Attachment B-1 RFP §8.2.7.2 -- Mediciad Standard Member Appeal Process
Contract Attachment B-1 RFP §8.4.3 – CHIP Member Complaint and Appeal Process
|
The HMO must resolve at least 98% of Member Appeals within 30 calendar days from the date the Appeal is filed with the HMO. | Measured Quarterly during the Operations Period | Per reporting peorid, per HMO Program, per SA. | HHSC may assess up to $500 per reporting period if the HMO fails to meet the performance standard. |
|
Contract Attachment B-1 RFP §8.1.6 -- Marketing & Prohibited Practices
Uniform Managed Care Manual
|
The HMO may not engage in prohobited marketing practices. |
Transition, Measured Quarterly during the Operations Period
|
Per incident of non-compliance.
|
HHSC may assess up to $1,000 per incident of non-compliance.
|
| Contract Attachment B-1 RFP §8.1.15.3 -- Behavioral Health services Hotline |
A. The HMO must have an emergency and crisis Behavioral Health services Hotline available 24 hours a day, seven (7) days a week, toll-free throught the Service Area(s).
B. Crisis hotline staff must include
or have access to qualified Behavioral Health Service professionals to assess behavioral health emergencies.
C. The HMO must ensure that the toll-free Behavioral Health Services Hotline meets the following minimum requiremetns for the HMO Program:
1. Call pickup rate - At least 99% of calls are answered on or before the fourth ring or an automated call pick up system.
2. Call hold rate - At least 80% of calls must be answered by toll-free line staff within 30 seconds.
3. Call abandonment rate - Call abandonment rate is 7% or less.
|
Operations and Turnover |
A. Each incident of non-compliance per HMO Program and SA.
B. Each incident of non-compliance per HMO Program and SA.
C. Per HMO Program and SA, per month, each percentage point below the standard for 1 and 2 and each percentage point above the standard for 3.
D. Per month, for each 30 second time increment, or portion threof, by which the average hold time exceeds the maximum acceptable hold time.
|
HHSC may assess:
A. Up to $100.00 for each hour or portion thereof that appropriately staffed toll-free lines are not operational. If the MCO's failure to meet the performance standard is caused by a Force Majeure Event, HHSC will not assess liquidated damages unless the MCO fails to implement its Disaster Recovery Plan.
B. Up to $100.00 per incident for each occurence that HHSC identifies through its recurring monitoring process that toll-free line staff were not qualified or did not have access to qualified professionals to assess behavioral health emergencies.
C.Up to $100.00 for each percentage point for each standard that the HMO fails to meet the requirements for a monthly reporting period for any HMO operated toll-free lines.
D. Up to $100.00 may be assessed fore each 30 second time increment, or portion thereof, by which the MCO's average hold time exceeds the maximum acceptable hold time.
|
|
Contract Attachment B-1 RFP §8.1.17.2 --Financial Reporting Requirements
Uniform Managed Care Manual - Chapter 5
|
Financial Statistical Reports (FSR):
For each HMO Program and SA, the HMO must file quarterly and annual FSRs. Quarterly reports are due no later than 30 days after the conclusion of each State Fiscal Quarter (SFQ). The first annual report is due no later than 120 days after the end of each Contract Year and the second annual report is due no later than 365 days after the end of each Contract Year.
|
Quarterly during the Operations Period
|
Per calendar day of non-compliance, per HMO Program, per SA.
|
HHSC may assess up to $1,000 per calendar day, a quarterly or annual report is late, inaccurate or incomplete.
|
|
Contract Attachment B-1 RFP §8.1.17.2 -- Financial Reporting Requirements:
Uniform Managed Care Manual - Chapter 5
|
Medicaid Disproportionate Share Hospital (DSH) Reports: The Medicaid HMO must submit, on an annual basis, preliminary and final DSH Reports. The Preliminary report is due no later than June 1st after each reporting year, and the final report is due no later than July 1st after each reporting year.
This standard does not apply to CHIP HMOs.
Any claims added after July 1st shall include supporting claim documentation for HHSC validation.
|
Measured during 4th Quarter of the Operations Period (6/1 - 8/31)
|
Per calendar day of non-compliance per HMO Program, per SA.
|
HHSC may assess up to $1,000 per calendar day, per program, per service area, for each day the report is late, incorrect, inaccurate or incomplete
|
|
Contract Attachment B-1 RFP §8.1.18 – Management Information System (MIS) Requirements
|
The HMO’s MIS must be able to resume operations within 72 hours of employing its Disaster Recovery Plan. |
Measured Quarterly during the Operations Period
|
Per calendar day of non-compliance per HMO Program, per SA.
|
HHSC may assess up to $5,000 per calendar day of non-compliance
|
| Contract Attachment B-1 RFP §8.1.18.n Encounter Data |
The HMO must submit Encounter Data transmissions and include all Encounter Data and Encounter Data adjustments processed by the HMO on a monthly basis, not later than the 30th calendar day after the last day of the month in which the claim(s) are adjudicated. Additionally, the HMO will be subject to liquidated damages if the Quarterly Encounter Reconciliation Report (which reconciles the year-to-date paid claims reported in the Financial Statistical Report (FSR) to the appropriate paid dollars reported in the Texas Encounter Data (TED) Warehouse) includes more than a 2% variance (i.e., less than a 98% match).
|
Measured Quarterly during Operations Period
|
Per incident of non-compliance, per HMO Program, per Service Area (SA)
|
HHSC may assess up to $2,500 per Quarter, per Program, per SA if the HMO fails to submit monthly encounter data. HHSC may assess up to $5,000 per quarter, per Program, per SA for each additional quarter that the HMO fails to submit monthly Encounter Data.
SA if the MCO falls below the 98% match standard. HHSC may assess up to $5,000 per Quarter, per Program, per SA for each additional Quarter that the MCO falls below the 98% match standard.
|
|
Contract Attachment B-1 RFP §8.1.18.3 – Management Information System (MIS) Requirements: System-Wide Functions
|
The HMO’s MIS system must meet all requirements in Section 8.1.18.3 of Attachment B-1.
|
Measured Quarterly during the Operations Period |
Per calendar day of non-compliance per HMO Program, per SA.
|
HHSC may assess up to $5,000 per calendar day of non-compliance.
|
|
Contract Attachment B-1 RFP §8.1.18.5 -- Claims Processing Requirements
Unifrom Managed Care Manual Chapter 2
|
The HMO must adjudicate all provider Clean Claims within 30 days of receipt by the HMO. The HMO must pay providers interest at an 18% per annum, calculated daily for the full period in which the Clean
Claim remains unadjudicated beyond the 30-day claims processing deadline. Interest owed the provider must be paid on the same date that the claim is adjudicated.
|
Measured Quarterly during the Operations Period |
Per incident of non-compliance.
|
HHSC may assess up to $1,000 per claim if the HMO fails to timely pay interest.
|
|
Contract Attachment B-1 RFP §8.1.18.5 -- Claims Processing Requirements
Unifrom Managed Care Manual - Chapter 2
|
The HMO must comply with the claims processing requirements and standards as described in Section 8.1.18.5 of Attachment B-1 and in Chapter 2 of the Uniform Managed Care Manual.
|
Measured Quarterly during the Operations Period |
Per quarterly reporting period, per HMO Program, per Service Area, per claim type.
|
HHSC may assess liquidated damages of up to $5,000 for the first quarter that an HMO’s Claims Performance percentages by claim type, by Program, and by service area, fall below the performance standards. HHSC may assess up to $25,000 per quarter for each additional quarter that the Claims Performance percentages by claim type, by Program, and by service area, fall below the performance standards.
|
|
Attachment B-1 RFP §8.1.20 Reporting Requirements
Attachment B-1 RFP §8.2.5.1 Provider Complaints
Attachment B-1 RFP §8.2.7.1 Member Complaint Process
|
The HMO fails to submit a timely response to an HHSC Member or Provider Complaint by the specified due date. The HMO response must be submitted according to the timeframes and requirements stated within the HMO Notification Correspondence (letter, email, etc).
|
Measured on a Quarterly Basis | Each incident of non-compliance per HMO Program and SA |
HHSC may assess up to $250 per calendar day for each day beyond the due date specified within the HMO Notification Correspondence.
|
|
Contract Attachment B-1 RFP §8.1.20.2-- Reporting Requirements
Uniform Managed Care Manual Chapters 2 and 5
|
Claims Summary Report:
The HMO must submit quarterly, Claims Summary Reports to HHSC by HMO Program, by Service Area, and by claim type, by the 30th day following the reporting period unless otherwise specified.
|
Measured Quarterly during the Operations Period | Per calendar day of non-compliance, per HMO Program, Service Area, per claim type. |
HHSC may assess up to $1,000 per calendar day the report is late, inaccurate, or incomplete.
|
|
Contract Attachment B-1 RFP §8.3.3 – STAR+PLUS Assessment Instruments
Attachment B-1 RFP §8.3.4.1 - For Members
Attachment B-1 RFP §8.3.4.2 - For Medical Assistance Only (MAO) Non-Member Applicants
|
The Community Medical Necessity and Level of Care (MN LOC) Assessment Instrument must be completed and electronically submitted via the TMHP portal in the specified format within 45 days: 1) from the date of referral for 1915(c) Waiver services for MAO applicants; 2) from the date of the Member's request for 1915(c) Waiver services for current Members requesting an upgrade; or 3) prior to the annual ISP expiration date for all Members receiving 1915(c) Waiver services as specified in Section 8.3.3.
|
Operations, Turnover | Per calendar day of non-compliance, per Service Area. |
HHSC may assess up to $500 per calendar day per Service Area, for each day a report is late, inaccurate or incomplete.
|
| Contract Attachment B-1 RFP §9.2 -- Transfer of Data | The HMO must transfer all data regarding the provision of Covered Services to Members to HHSC or a new HMO, at the sole discrection of HHSC and as directed by HHSC. All transferred data must comply with the Contract requirements, including HIPAA. | Measured at Time of Transfer of Data and ongoing after the Transfer of Data until satisfactorily completed | Per incident of non-compliance (failure to provide data and/or failure to provide data in required format), per HMO Program, per SA. | HHSC may assess up to $10,000 per calendar day the data is late, inaccurate or incomplete. |
| Contract Attachment B-1 RFP §9.3 -- Turnover Services | Six months prior to the end of the contract period or any extension thereof, the HMO must propose a Turnover Plan covering the possible turnover of the records and information maintained to either the State (HHSC) or a successor HMO. | Measured at Six Months prior to the end of the contract period or any extension thereof and ongoing until satisfactorily completed | Each calendar day of non-compliance per HMO Program, per SA. |
HHSC may assess up to $1,000 per calendar day the Plan is late, inaccurate, or incomplete.
|
|
Contract Attachment B-1 RFP §9.4-- Post-Turnover Services
|
The HMO must provide the State (HHSC) with a Turnover Results report documenting the completion and results of each step of the Turnover Plan 30 days after the Turnover of Operations. | Measured 30 days after the Turnover of Operations | Each calendar day of non-compliance per HMO Program, per SA. | HHSC may assess up to $250 per calendar day the report is late, inaccurate or incomplete. |
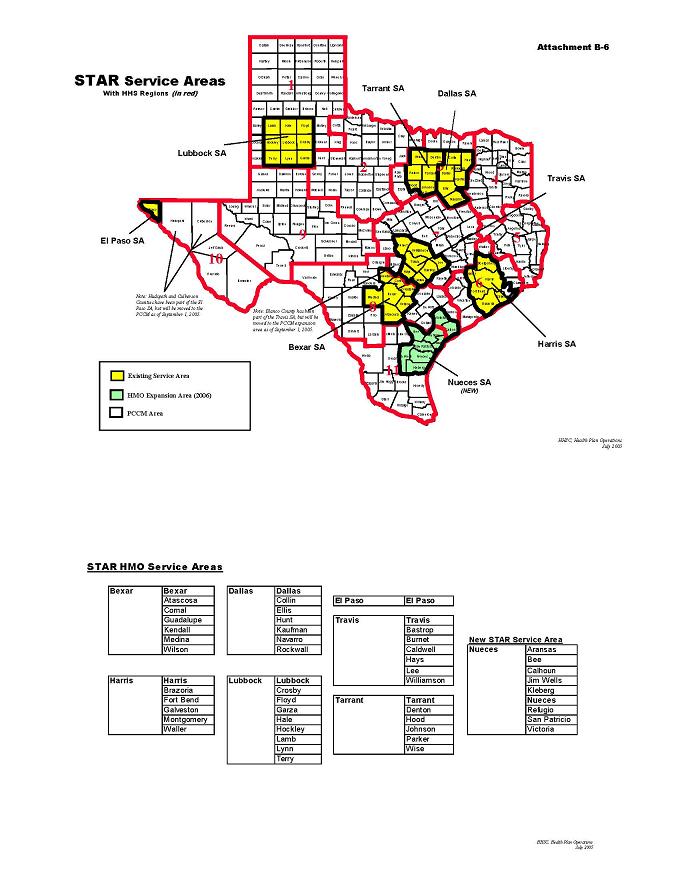
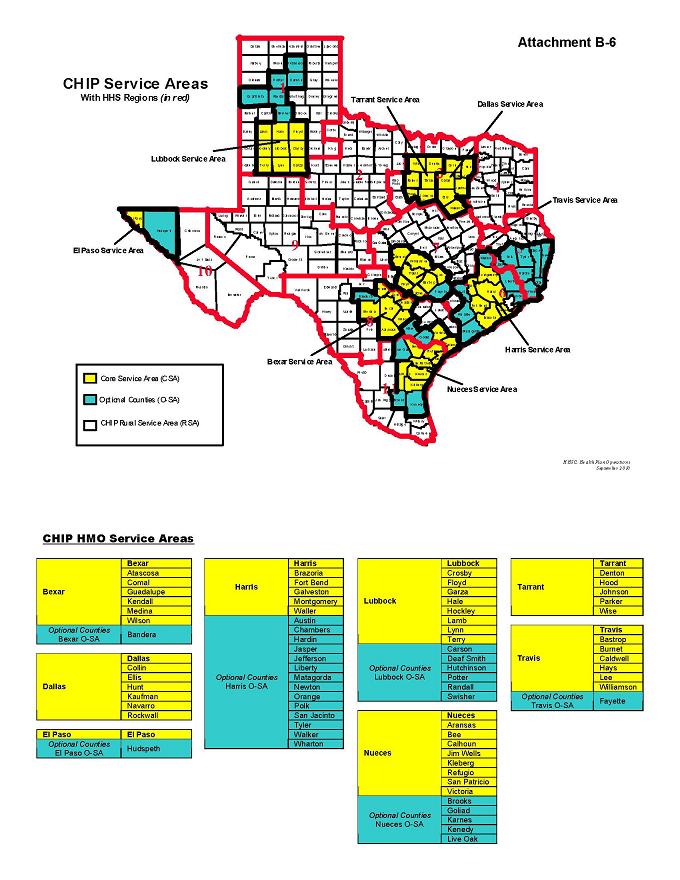
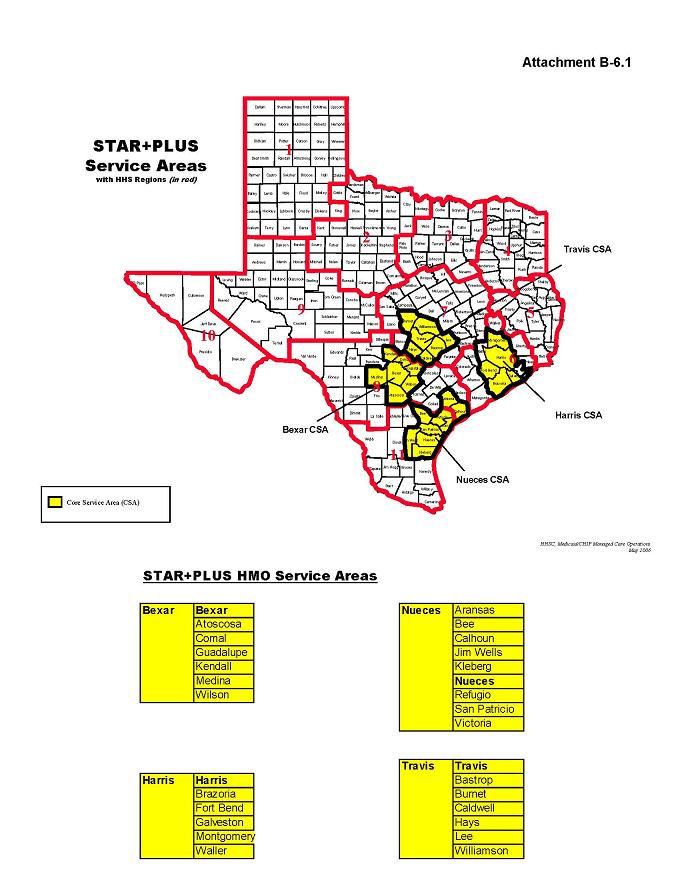
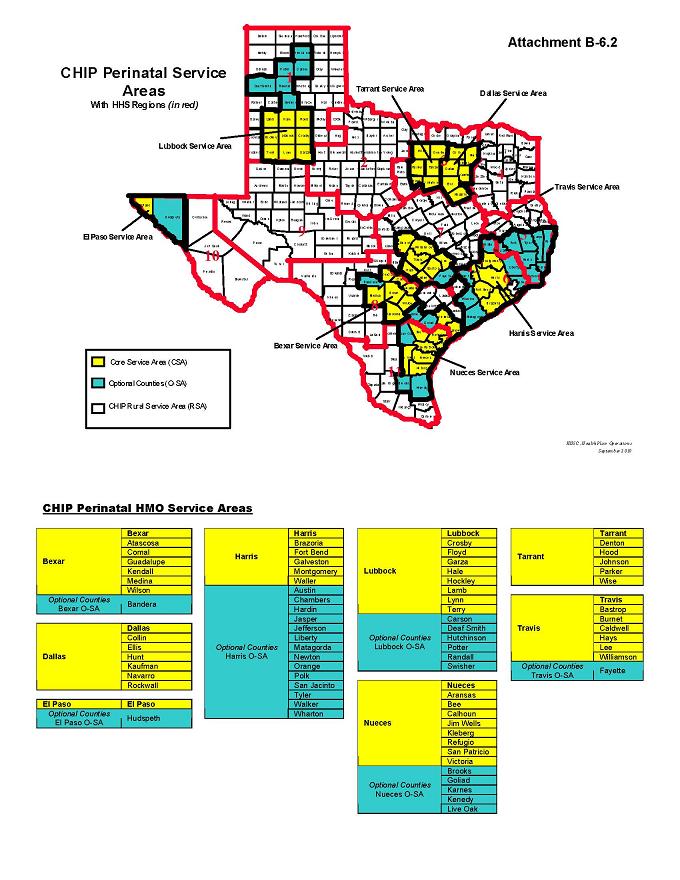
|
DOCUMENT HISTORY LOG
|
|||
|
STATUS1
|
DOCUMENT
REVISION2
|
EFFECTIVE
DATE
|
DESCRIPTION3
|
|
Baseline
|
n/a
|
January 1, 2007
|
Initial version of Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology, was incorporated into Version 1.5 of the Contract.
|
|
Revision
|
1.6
|
February 1, 2007
|
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
|
Revision
|
1.7
|
July 1, 2007
|
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
|
Revision
|
1.8
|
September 1, 2007
|
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
|
Revision
|
1.9
|
December 1, 2007
|
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
| Revision | 1.10 | March 1, 2008 |
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
| Revision | 1.11 | September 1, 2008 |
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
| Revision | 1.12 | March 1, 2009 |
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
| Revision | 1.13 | September 1, 2009 | Attachment B-7 is modified to remove references to the DADS enhancement program. |
| Revision | 1.14 | December 1, 2009 |
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
| Revision | 1.15 | March 1, 2010 |
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
| Revision | 1.16 | September 1, 2010 |
Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology.
|
| Revision | 1.17 | December 1, 2010 | Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Payments Methodology. |
| Revision | 1.18 | March 1, 2011 | Contract amendment did not revise Attachment B-7, STAR+PLUS Attendant Care Enhanced Paymetns Methodology. |
|
1 Status should be represented as “Baseline” for initial issuances, “Revision” for changes to the Baseline version, and “Cancellation” for withdrawn versions
2 Revisions should be numbered in accordance according to the version of the issuance and sequential numbering of the revision—e.g., “1.2” refers to the first version of the document and the second revision.
3 Brief description of the changes to the document made in the revision.
|
|||
|
I. Provider Contracting
|
(a) Description of criteria the HMO will use to allow participation in the STAR+PLUS Attendant Care Enhanced Payments.
(b) Description of any limitations or restrictions.
|
||
|
Superior HealthPlan will only allow those providers that are currently participating in the DADS Attendant Compensation Rate Enhancements to participate in the STAR+PLUS Attendant Care Enhanced Payments. SHP will have an enrollment period corresponding to the DADS enrollment period to allow new providers to participate in the SHP Attendant Care Enhanced Payments.
|
|||
|
II. Payment for STAR+PLUS Attendant Care Enhanced Payments
|
Description of methodology the HMO will use to pay for the Attendant Care Enhanced Payments. Provide sufficient detail to fully explain the planned methodology.
|
||
|
Superior will not use the DADS rates. SHP will establish an additional amount to be added on to the unit rate by type of service.
|
|||
|
III. Timing of the Attendant Care Enhanced Payments
|
Description of when the payments will be made to the Providers and the frequency of payments. Also include timeframes for Providers complaints and appeals regarding enhanced payments.
|
||
|
The enhanced rate payment amount will be paid at the time of claims payment so the frequency will depend on the frequency with which providers file their claims. Provider complaints and appeals will be handled through the normal complaint and appeal process and finalized within 30 days from receipt.
|
|||
|
IV. Assurances from Participating Providers
|
Description of how the HMO will ensure that the participating Providers are using the enhancement funds to compensate direct care workers as intended by the 2000-01 General Appropriations Act (Rider 27, House Bill 1, 76th Legislature, Regular Session, 1999) and by T.A.C. Title 1, Part 15, Chapter 355.
|
||
|
Participating Providers will be required by contract to complete and submit an affidavit annually stating they applied the enhancement funds to the compensation for direct care staff. Compensation may include increased hourly rates, bonuses, paid holidays or additional benefits such as employer paid insurance.
|
|||
|
V. Monitoring of Attendant Care Enhanced Payments
|
Explanation of the Monitoring Process that the HMO will use to monitor whether the Attendant Care Enhanced Payments are used for the purposes intended by the Texas Legislature.
|
||
|
Each Provider’s compliance with the attendant compensation spending requirement for the reporting period will be monitored on an annual basis via the submission of the affidavit stating they applied the enhancement funds to the compensation for direct care staff. Compensation may include increased hourly rates, bonuses, paid holidays or additional benefits such as employer paid insurance. In addition, providers may be audited on as as-needed basis to ensure financial records support the pass through of the enhanced funds. Enhanced payments could potentially be recouped for those Providers who fail to pass the funds to their direct care staff.
|